This article has been verified for CPD. Click the button below to answer a few
short questions and download a form to be included in your CPD folder.
While Botulinum toxin A, dermal fillers, chemical peels and laser resurfacing are well studied and recognised anti-ageing treatments, the concept of skin biorevitalisation has gained more attention in the past few years.
Skin health has become the driving force behind the booming of new rejuvenating approaches, with the global market projection for anti-ageing products growing from US$37.1 billion in 2022 to US$45.6 billion by 2026 [1]. Social media platforms are permeated by photo filtering and editing to create a template of youthful and healthy looking skin.
Biorevitalisation is fundamentally related to mesotherapy; it is a non-surgical, minimally invasive transdermal injection technique using low dosage of active substances administered directly into the area of skin on which they are intended to act. It is also known as skinboosters, intradermal therapy, biorejuvenation, mesolift or mesoglow. The injected agents subsequently and gradually spread to the underlying tissues with little significant side-effects [2].
A plethora of premixed and multicomponents such as vitamins, amino acids and mineral solutions are available for this purpose; in this article we will solely focus on hyaluronic acid (HA), which is the most established biorevitaliser component.
Skin ageing
Facial ageing results from a combination of changes in bone, muscles, adipose tissues, ligaments and skin. External factors such as UV radiation, smoking, poor nutrition, stress and air pollution, in conjunction with chronological or intrinsic factors, contribute to cumulative cutaneous ageing leading to deterioration of structural stability and degeneration of physiological function [3].
Intrinsic ageing is well depicted in areas such as upper inner aspects of arms, hips and buttocks, usually protected from UV exposure. Extrinsic or photoageing is commonly represented on areas more exposed to UV radiation such as face, decolletage, forearms, dorsal of hands and neck, with an amplification of the clinical changes including dryness, atrophy, dyspigmentation and wrinkles [4].
Histological and structural hallmarks of skin ageing are reflected in both the epidermis and dermis, and include lower lipid content in the stratum corneum, flattening of dermal-epidermal junction, decline in the capacity of re-epithelisation, dermal atrophy, general vascular and cellular deterioration [5].
Both types of ageing share molecular similarities, with recent evidence indicating that they are initiated and many times promoted by oxidation events.
Reactive oxygen species (ROS) are molecules that cause direct detrimental modifications to the cellular components and lipid membranes; other events that derive from these oxidative processes include mitochondrial dysfunction, genomic instability and cellular senescence [6,7].
Another noteworthy change is the fragmentation of collagen and elastin fibres in the once organised extracellular matrix (ECM) leading to a decrease in the stretching properties of fibroblasts and an adverse effect in the overall skin quality [8].
The aim of biorevitalisation is to boost cellular function and optimise the ECM micro-environment with a consequent enhancement of skin structural support and metabolic recovery [9].
Hyaluronic acid
The name ‘hyaluronic acid’ is derived from hyaloid (vitreous) and uronic acid. This nomenclature is primarily attributed to Karl Meyer and his assistant, John Palmer, who in 1934 isolated a novel glysosaminoglycan from the vitreous of bovine eyes.
Nowadays, this macromolecule is frequently referred to as ‘hyaluronan’ when related to ‘in vivo’ status [10].
HA is a naturally occurring glycosaminoglican polysaccharide synthesised by fibroblasts within the cell membrane before being released in the extracellular matrix of connective tissue, synovial fluid, and other tissues. Here it plays an important role in the homeostasis and hydration.
Additionally, this endogenous HA contributes to the inherent skin defence mechanism by scavenging free radicals induced by detrimental extrinsic elements such as UV irradiation, pollution and other oxidative stresses.
Found in high concentrations in young and healthy skin, studies support its biochemical role in the healing process, interaction with proteoglycans such as aggrecan, modulation of inflammatory cells and normal cellular functionality in the extracellular space [11].
These glycosaminoglycans are notably reduced during the ageing process, leading to reduction of collagen density and elasticity, skin atrophy and dryness.
Biorevitalisation with HA
Skin biorevitalisation with injectables has been explored by many authors as a unique treatment to boost overall skin quality and health. HA is the most studied component of the many biorevitalising products available on the market and due to its well-known viscoelastic properties and high affinity to water, it is easy to understand its capacity to restore skin hydration, elasticity and firmness. Moreover, being a natural component of the dermal extracellular matrix, it renders the beneficial biocompatible and biodegradable qualities [12].
HA dermal fillers have been routinely used for volumisation, augmentation, contouring and enhancement of all facial areas. For the purpose of biorevitalisation it has to act without much volume induction.
Given the high density of the ECM, it is paramount that the HA gel presents a low viscosity, respecting the histological structures of the dermis, causing little trauma with a strong tendency to spread out.
Being injected in such a superficial layer, the gel should not have too much elasticity, promoting little pressure between tissues and avoiding over-correction and / or long-lasting irregularities [Denis Couchourel, PhD, Scientific & Medical Director of Vivacy Paris, email communication, January 2022]. This is an important observation to prevent undesirable results and complications.
Non cross-linked (NCL) and cross-linked (CL) HA products are available on the market, with HA concentrations ranging from 8mg/ml HA to 20mg/ml HA. The lower concentrations are suitable for younger patients and / or delicate areas with thin skin, while the higher concentrations are particularly suitable for counteracting the main signs of skin ageing such as roughness and deep wrinkles [13].
HA may be accompanied by other ingredients such as vitamins, antioxidants, minerals and amino acids; these are biological components developed to support the HA and its effects on the skin [14].
As soon as an injection is performed, with needle or cannula, an inflammatory response is triggered, eliciting the release of free radicals that promote degradation of the HA; mannitol, for example, has been incorporated into some products due to its scavenging properties against free radicals therefore increasing durability by slowing down degradation [15].
Both NCL and CL HA have been shown to be effective on skin quality, however NCL HA has a short half-life making it less stable than the CL products [14,16]. The cross-linking allows for a slower degradation of the HA by the endogenous hyaluronidases, consequently prolonging the interaction in the ECM and stimulating fibroblasts, leading to a sustained skin improvement [17].
Indications
This modality of treatment has also been aimed at the younger patient with the goals of prevention of ageing and maintenance of youthful and healthy skin.
The main indications are areas such as the face, neck and decolletage, which are more adversely affected by photoageing; concurrently the literature has also positively explored the use of skinboosters in other body regions such as hands and arms [18,19].
Treatment considerations
There is a paucity in standardisation regarding protocols, therefore attendance at training provided by the manufacturers is recommended. Biorevitalisation with HA is a progressive treatment therefore multiple sessions may be required to achieve the desired effect.
A recent prospective study evaluating a NCL HA product showed statistically significant improvement in skin firmness and elasticity after eight weeks from baseline; although not with statistical significance, skin hydration improved after eight weeks and there was positive patient satisfaction at week eight, 12 and 16. Injections were performed at baseline, after three and six weeks [20].
A retrospective review from 2018 supports that a regimen consisting of three injections, one month apart, is efficient, safe and well-tolerated by subjects. Face treatments may show significant results after only one of the planned three sessions [21].
An expert panel consensus agreed that a standard initial protocol treatment of up to three sessions followed by maintenance at four to six-month intervals, would improve and preserve skin quality over time [13].
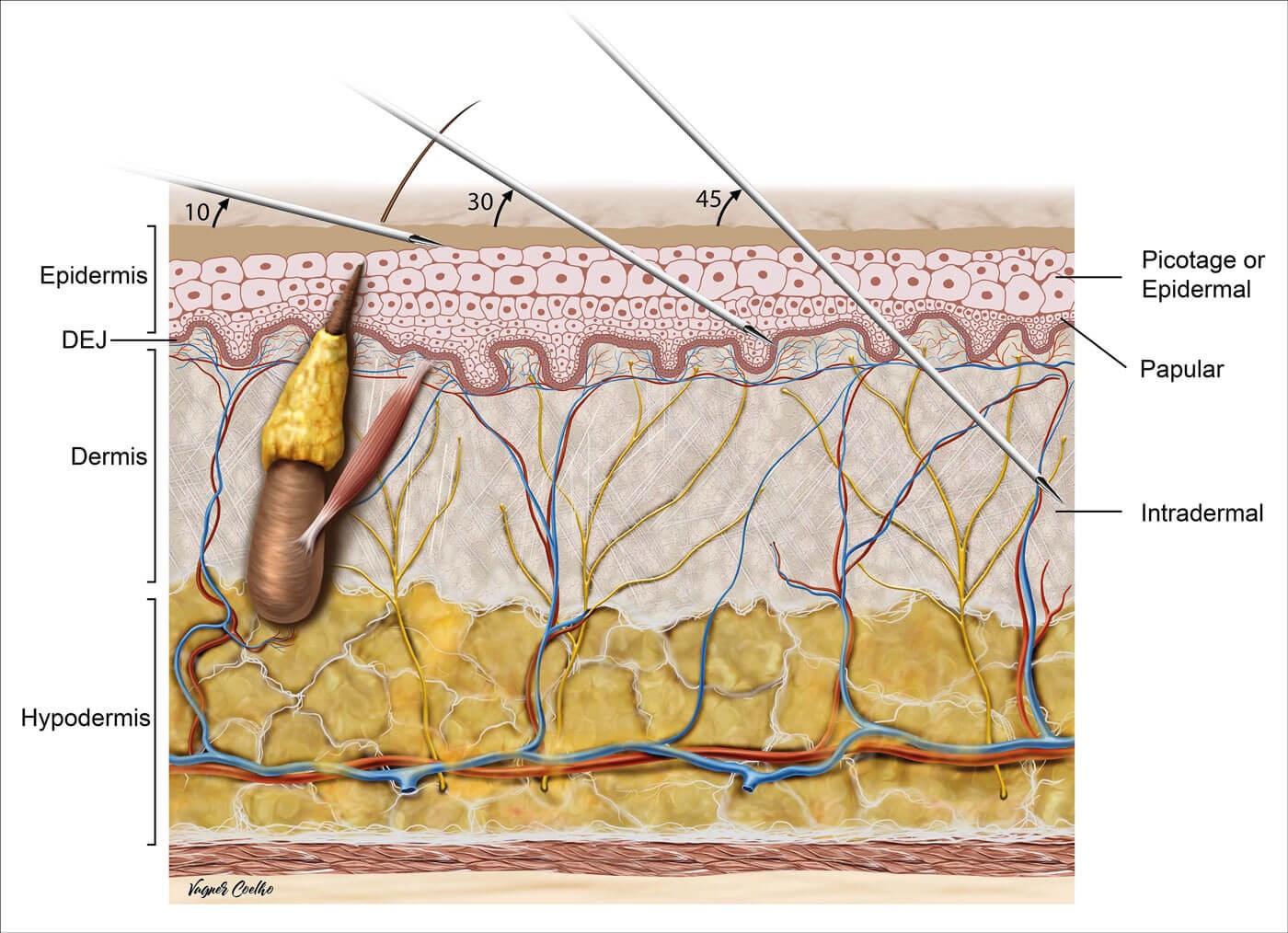
Figure 1: Schematic representation of skin layers and injection techniques.
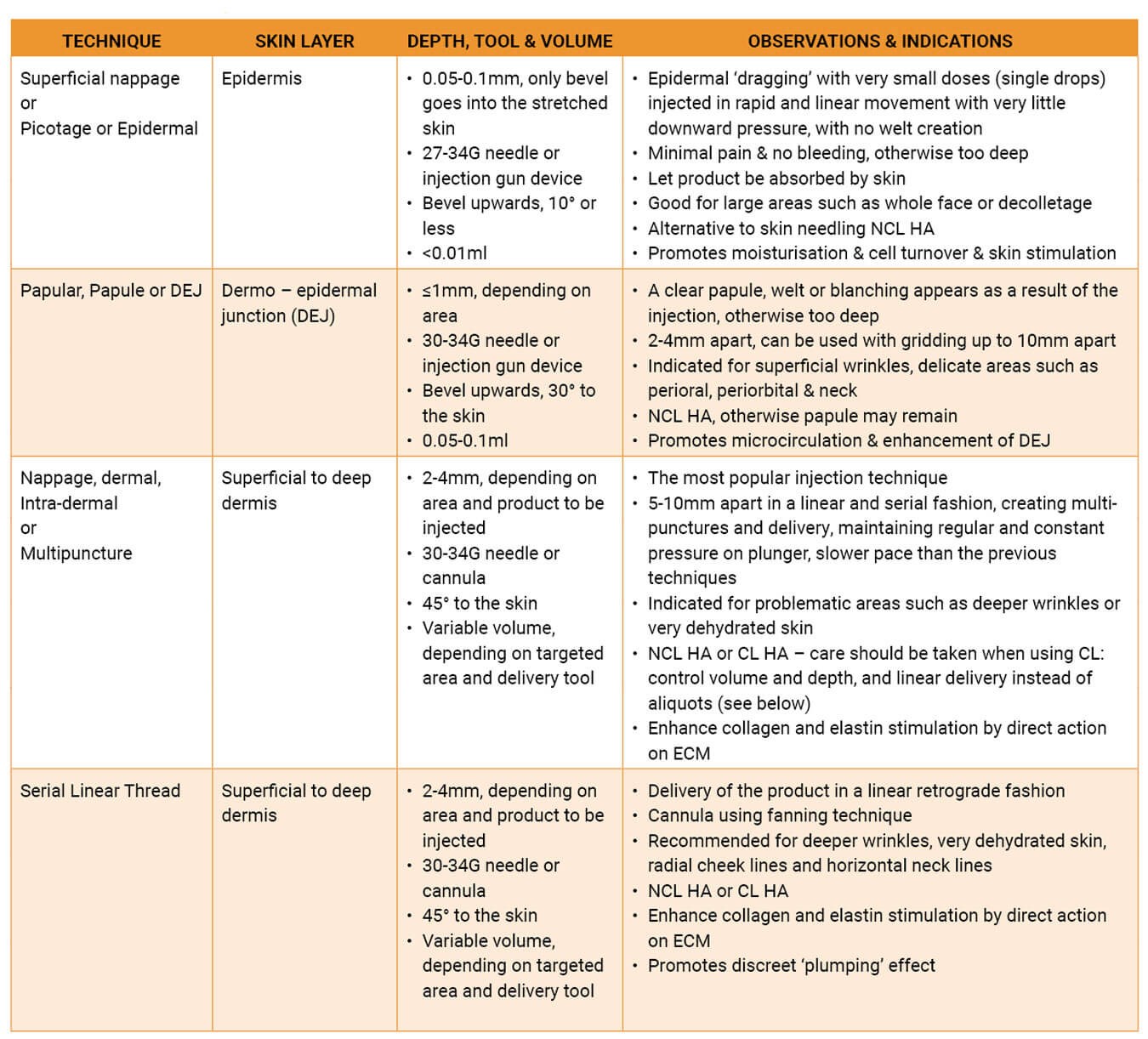
Table 1: Injection techniques and indications.
A thorough pre-treatment assessment including full medical and aesthetic history will help in setting goals and expectations. Patients should be cautioned that any immediate volumisation or ‘plumping’ will subside after a few days and visible results of skin improvement including glowing and tightening may be noticeable five to10 days after treatment and effects will last around four to six months [22]. It is crucial to keep a good record and documentation including skin analysis, standardised photos and objective assessment if available.
The main contraindications do not differ from other types of injectables: pregnancy or breastfeeding, allergy or intolerance to any of the substances used, history or predisposition to hypertrophic scars, acute viral or bacterial infections, acute inflammatory skin conditions, bleeding disorders, blood-thinning medications and compromised immunity.
Studies have shown minimal side-effects such as bleeding, ecchymosis, oedema, discomfort or pain. These are usually local reactions, reversible and short-lived. Severe complications are rare and usually a result of inadequate product administration and / or inappropriate injection technique with poor assessment [23]. Post-treatment instructions include the use of sunblock and no make-up for 12 hours, downtime is very limited.
Techniques
The many injection techniques described in the literature can be delivered either manually (needle or cannula) or by injection devices (mesotherapy gun). The angle of entry, volume, depth and spacing of the injections must be individualised to the targeted area, skin condition and type of HA; injudicious technique may lead to unwanted side-effects such as haematomas or skin surface irregularities [23,24] (Table 1 and Figure 1).
A previously mentioned study using NCL HA demonstrated patient satisfaction with improved skin appearance including hydration and texture when intradermal multipuncture was performed compared to epidermal, which showed very little skin improvement. This may support that injection technique can be significant in obtaining a positive outcome [14].

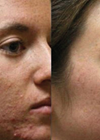
Figure 2: Images showing improvements in skin quality and texture. Face and neck treated with combined techniques: NCL HA 14mg/1g (Stylage Hydro®, Vivacy) with papular injections using 30G 4mm needle for whole face and neck & CL HA 12.5 mg/1g (Stylage Hydromax®, Vivacy) with intradermal fanning technique delivered by blunt cannula 25G 38mm in the radial cheek and marionette lines and linear threads with 30G 13mm needle for horizontal neck lines. Treatment plan: Initial three sessions, three weeks apart, then maintenance twice a year.
A. Before treatment; B. Twenty-four months after initial treatment.
Note: this patient has also been treated with Botulinum Toxin A for upper face and HA dermal filler for midface within this period.
A mixed technique, combining superficial and deeper injections at the same session, is a good concept to optimise results [24] (Figure 2).
Conclusion
Evidence shows the role of HA-based products in improving overall appearance and functionality of aged skin with a high safety profile and short downtime. Minimally invasive, it can be incorporated with more advanced or invasive treatments and is suitable for all ages.
Understanding of skin anatomy and function, and rheological properties of HA are fundamental for judicious choice of technique to prevent unwanted side-effects and to ensure good outcomes.
Even though versatile and adaptable to all injector levels, the lack of standardised protocol means that strict adherence to manufacturer’s instructions and training is highly recommended.
References
1. Global Industry Analysts. 2022.
https://www.strategyr.com/market
-report-anti-aging-products-forecasts
-global-industry-analysts-inc.asp
[Last accessed 26 October 2022].
2. Sivagnanam G. Mesotherapy - The french connection. J Pharmacol Pharmacother 2010;1(1):4-8.
3. Farage MA, Miller KW, Elsner P, Maibach HI. Characteristics of the Aging Skin. Adv Wound Care (New Rochelle) 2013;2(1):5-10.
4. Sachs D, Fisher G, Voorhees J. ‘Skin Ageing’ In: Griffiths CEM, Barker J, Bleiker TO, et al. (Eds). Rook’s Textbook of Dermatology 9th Edition UK; Wiley-Blackwell; 2016.
5. El-Domyati M, Attia S, Saleh F, et al. Intrinsic aging vs. photoaging: a comparative histopathological, immunohistochemical, and ultrastructural study of skin. Exp Dermatol 2002;11(5):398-405.
6. Fisher GJ, Kang S, Varani J, et al. Mechanisms of photoaging and chronological skin aging. Arch Dermatol. 2002;138(11):1462-70.
7. Kohl E, Steinbauer J, Landthaler M, Szeimies RM. Skin ageing. J Eur Acad Dermatol Venereol 2011;25(8):873-84.
8. Krieg TAM, Koch M, Chu M, Uitto J. ‘Collagens, elastic fibers, and other extracel- lular matrix proteins of the dermis.’ In: Goldsmith LAKS, Gilchrest BA, Paller AS, et al. (Eds). Fitzpatrick’s Dermatology in General Medicine 8th Edition New York, USA; McGraw-Hill; 2012.
9. Avantaggiato A, Pascali M, Lauritano D, et al. Hyaluronic acid in dermal rejuvenation: an in vitro study. J Biol Regul Homeost Agents 2015;29(3 Suppl 1):149-55.
10. Hascall VC, Laurent TC. Hyaluronan: Structure and Physical Properties. Glyco Forum [online] 1997;1(A2):
https://www.glycoforum.gr.jp/
article/01A2.html
[Last accessed 26 October 2022].
11. Monheit GD, Coleman KM. Hyaluronic acid fillers. Dermatol Ther 2006;19(3):141-50.
12. Streker M, Reuther T, Krueger N, Kerscher M. Stabilized hyaluronic acid-based gel of non-animal origin for skin rejuvenation: face, hand, and décolletage. J Drugs Dermatol 2013;12(9):990-4.
13. Belmontesi M, De Angelis F, Di Gregorio C, et al. Injectable non-animal stabilized hyaluronic acid as a skin quality booster: an expert panel consensus. J Drugs Dermatol 2018;17(1):83-8.
14. Taieb M, Gay C, Sebban S, Secnazi P. Hyaluronic acid plus mannitol treatment for improved skin hydration and elasticity. J Cosmet Dermatol 2012;11(2):87-92.
15. Ramos-E-Silva M, Fonteles LA, Lagalhard CS, Fucci-da-Costa AP. STYLAGE®: a range of hyaluronic acid dermal fillers containing mannitol. Physical properties and review of the literature. Clin Cosmet Investig Dermatol 2013;6:257-61.
16. Ogilvie P, Fink B, Leys C, et al. Improvement of radial cheek lines with hyaluronic acid-based dermal filler VYC-17.5L: results of the BEAM study. Dermatol Surg 2020;46(3):376-85.
17. Turlier V, Delalleau A, Casas C, et al. Association between collagen production and mechanical stretching in dermal extracellular matrix: in vivo effect of cross-linked hyaluronic acid filler. A randomised, placebo-controlled study. J Dermatol Sci 2013;69(3):187-94.
18. Fabi SG, Goldman MP. Hand rejuvenation: a review and our experience. Dermatologic Surgery 2012;38(7 pt2):1112-27.
19. Distante F, Pagani V, Bonfigli A. Stabilized hyaluronic acid of non-animal origin for rejuvenating the skin of the upper arm. Dermatol Surg 2009;35 Suppl 1:389-94.
20. Sulovsky M, Müller D, Prinz V, et al. A prospective open-label, multicentre study evaluating a non-cross-linked hyaluronic acid based soft-tissue filler in the correction of lateral canthal and perioral lines. J Cosmet Dermatol 2022;21(1):191-8.
21. Nikolis A, Enright KM. Evaluating the role of small particle hyaluronic acid fillers using micro-droplet technique in the face, neck and hands: a retrospective chart review. Clin Cosmet Investig Dermatol 2018;11:467-75.
22. Ogilvie P, Thulesen J, Leys C, et al. Expert consensus on injection technique and area-specific recommendations for the hyaluronic acid dermal filler VYC-12L to treat fine cutaneous lines. Clin Cosmet Investig Dermatol 2020;13:267-74.
23. Knoll B (Author), Sattler G (Editor). Illustrated Atlas of Esthetic Mesotherapy: Active Substances, Dosage, Administration. London, UK; Quintessence Publishing; 2013.
24. Smit R. Bio-skin-gineering: a novel method to focus cutaneous aging treatment on each individual layer of the skin specifically and precisely. Aesthetic Medicine 2019;5(1):14-22.
Declaration of competing interests: The author is an International Key Opinion Leader for Vivacy UK; she has not received any honorarium or reimbursement for writing this article.
COMMENTS ARE WELCOME