Balanitis xerotica obliterans (BXO) was initially described by Hallopeau in 1887 [1], when it was known as lichen sclerosis et atrophicus, the designation BXO, first being used by Stuhmer in 1928 [2]. It is a chronic, persistent and unrelenting inflammatory process mainly affecting the male external genitalia, though lichen sclerosis et atrophicus can affect females [1].
The disease principally affects the foreskin, the urethral meatus, the distal urethra, the penile skin and even the scrotum [3]. There are a myriad of clinical symptoms which include itching, phimosis, white plaques on the glans, meatal stenosis, urethral strictures, pain and discomfort, sexual dysfunction and even penile carcinoma [3].
The aetiology of BXO remains an enigma, with both genetic and autoimmune theories being postulated. The disease has been reported in young boys, although it mainly affects males aged between 30 to 60 years of age. It is more common in African-Americans and Hispanics, males who are uncircumcised and those suffering from BXO are thought to have a higher prevalence of other autoimmune disorders [4].
The choice of treatment can be either medical [5] or surgical [6] and we wish to report on four cases of BXO, who had failed to respond to previous medical and surgical treatment and presented with progressive and extensive disease of the penile skin, necessitating appropriate reconstructive procedures.
Patients and methods
Four male patients, who had failed with prior treatment for BXO and presented with extensive recurrent disease affecting the penile skin, were reviewed at a combined urology/plastic surgery clinic and a plan formulated for excision of the diseased tissue and appropriate reconstruction.
Results
Four male patients with a mean age of 53.5 years (range 39–63) presented with progressive BXO, the mean duration of symptoms being 35 years (range 20–50). All were obese [7], with a mean BMI of 40.1 (range 31.5–44.6) and all of the group suffered from pain, phimosis, recurrent balanitis, urinary leak or spray, and sexual dysfunction. All had previously been treated with topical steroids, six circumcisions had been performed (from age 6–36), one patient having previously undergone multiple circumcisions elsewhere, all had undergone meatal dilatations and two were self-dilating at the time of referral.
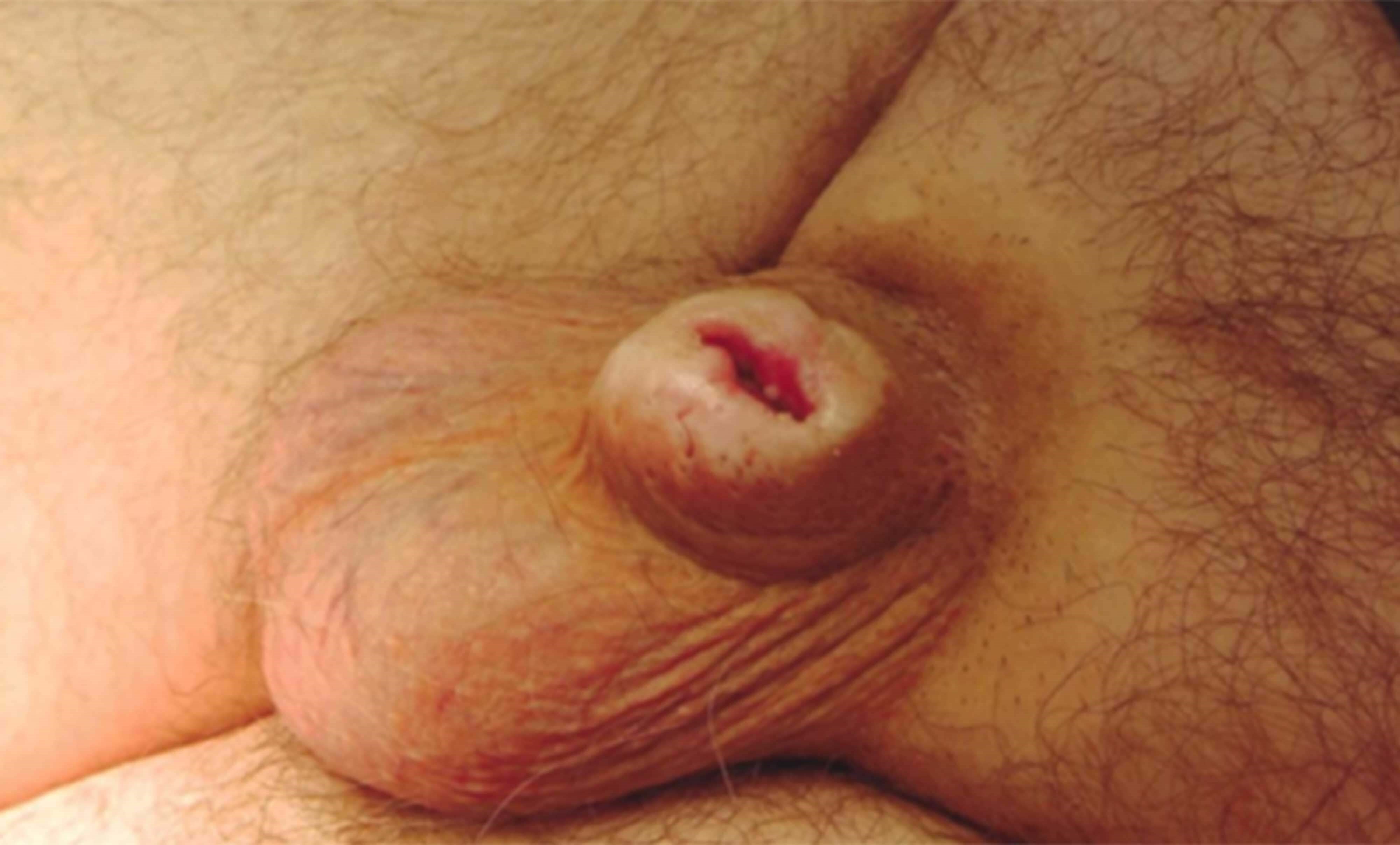
Figure 1: Severe penile scarring and deformity resulting from long-standing BXO.
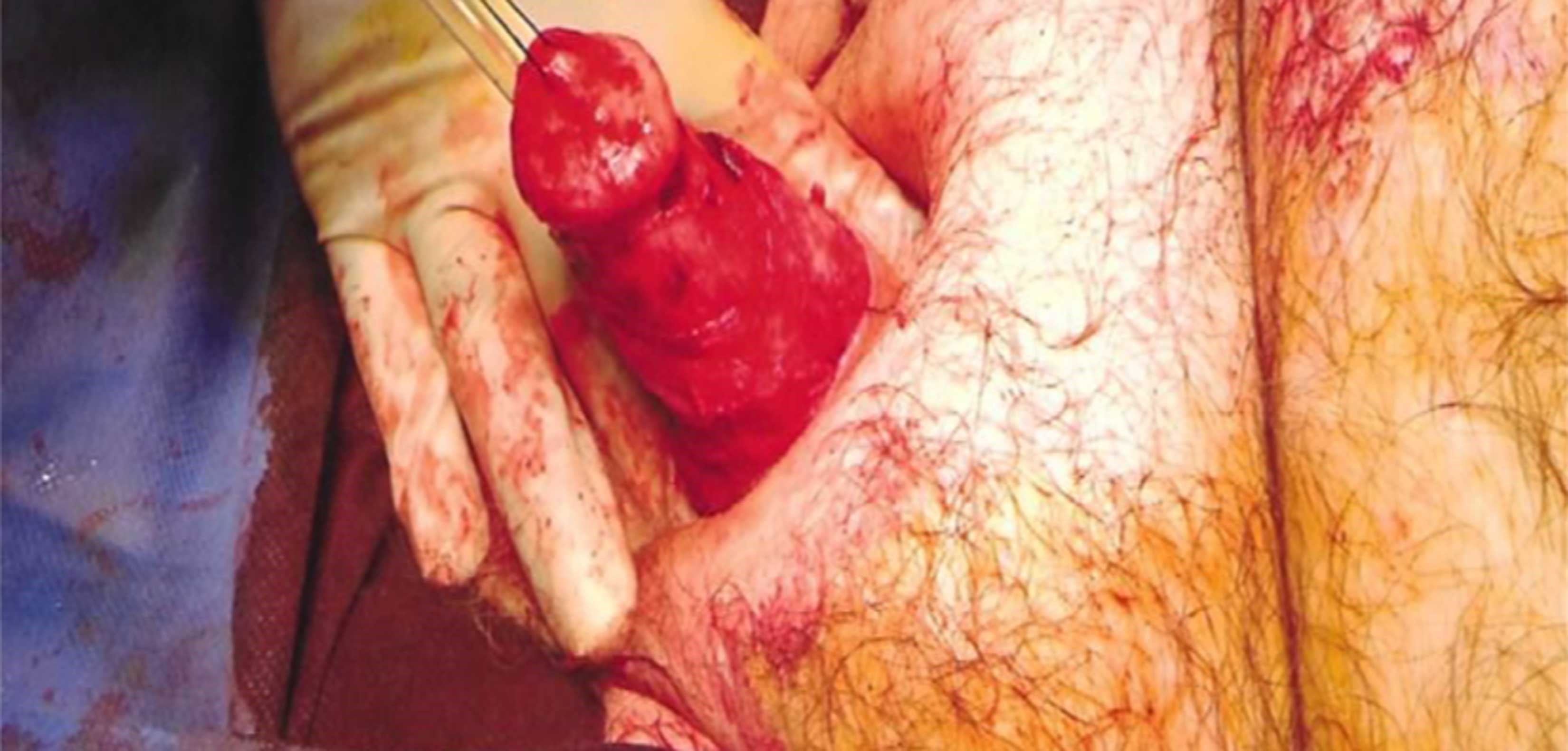
Figure 2: The excised diseased penile shaft skin.
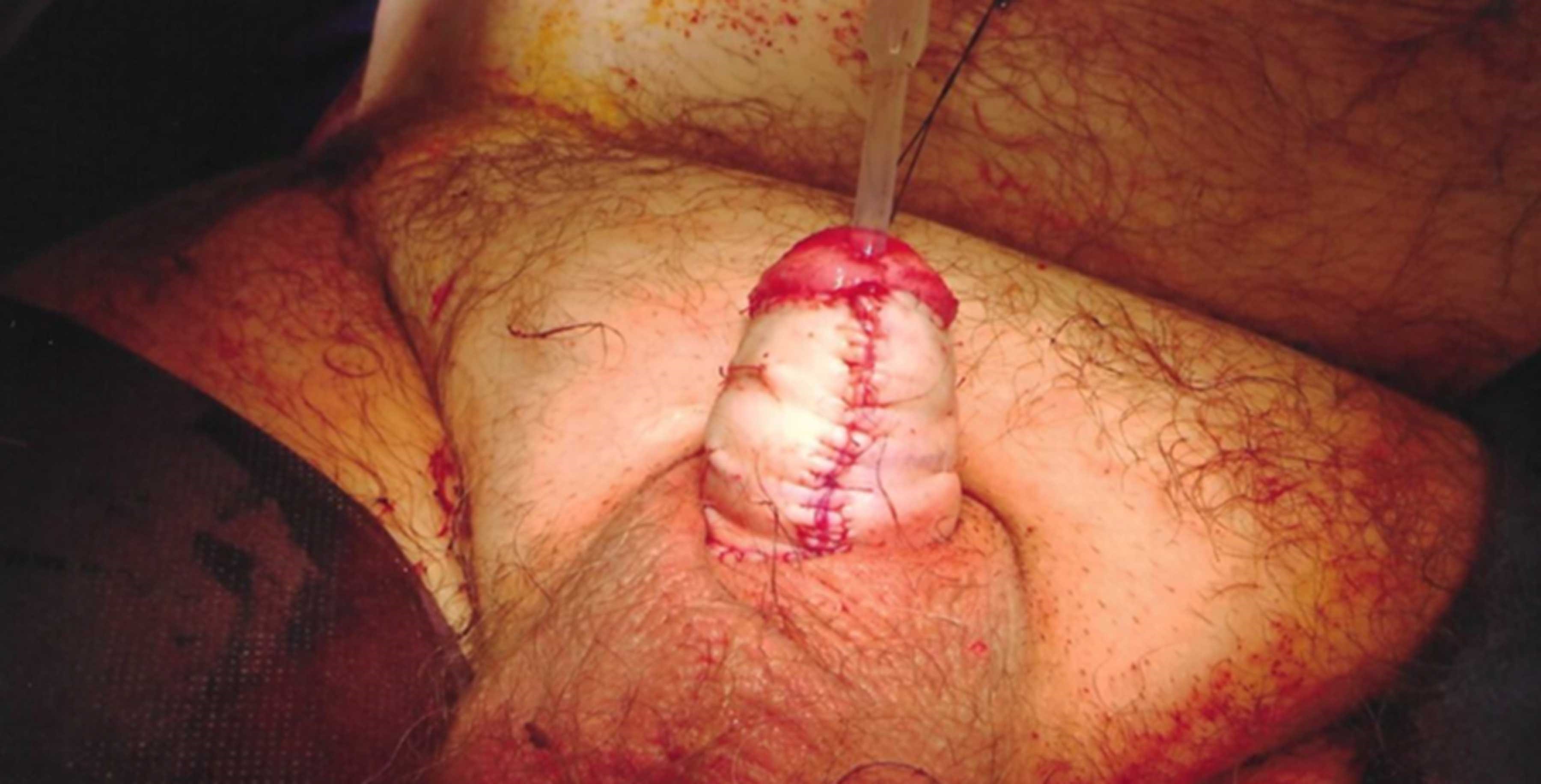
Figure 3: Penile reconstruction with a full thickness skin graft after release of the penis following excision of the diseased tissues.
All underwent a combined surgical procedure in which all the diseased tissue was radically excised and simultaneous appropriate and pertinent reconstruction carried out. In two patients, excision of the whole of the penile skin and full thickness skin grafting were performed (Figures 1–3), one patient had an extended circumcision which included excision of volar penile shaft skin and V-Y dorsal advancement flaps, and the final patient required an extended circumcision with penile shaft skin advancement. Two patients had dilatation of the urethral meatus performed and one other underwent simultaneous supra-pubic liposuction for a buried penis.
All were catheterised and all healed uneventfully, with relief of their preoperative symptoms. At a mean follow-up of 47 months (range 13–111), no patient has presented with recurrent disease.
Discussion
BXO is a chronic, progressive, inflammatory, autoimmune condition of unknown aetiology, mainly affecting older, uncircumcised men, its prevalence being present 0.1– 0.3% of males [5]. However, it is also frequently seen in the paediatric age group [4,7], with up to 15% of paediatric circumcision specimens demonstrating histological changes consistent with BXO.
When the condition is asymptomatic, then no treatment is required. However, when there are worsening manifestations of the disease, a variety of both medical and surgical treatment options are currently available.
Topical steroids, such as betamethasone, are the mainstay of the medical options [5] and some have even advocated the injection of intra-lesional hydrocortisone [1]. However, systemic steroids have currently no place in the management of this condition.
Others have advocated the topical application of the immunosuppressive agent tacrolimus to the penile lesions, and this is thought to alter the production of interleukin 2, thus inhibiting the inflammatory response [8]. Other non-surgical treatments include CO2 laser ablation [9] and platelet rich plasma [10].
When medical management is unsuccessful, then a surgical option becomes a necessity. For meatal stenosis and urethral strictures, regular dilatation and even meatotomy or urethral reconstruction may be required.
As the disease frequently involves the foreskin, circumcision has been the cornerstone of surgical procedures, however when this fails, a more radical approach along with appropriate reconstruction is required [11].
The four patients, described above, suffered from longstanding and unremitting BXO and had failed with medical treatments and classical circumcision. Following a multidisciplinary discussion, it was agreed with each patient that an extensive combined urology/plastic surgery procedure would be performed, with no restrictions placed on the extent of the surgical resection, which varied from an extended re-circumcision to complete resection of the penile shaft skin and skin grafting. This can either be split or full thickness skin grafting, the latter being chosen, initially utilising the excised redundant supra-pubic skin following extensive liposuction for an associated buried penis. Patients were catheterised postoperatively until full healing had been obtained.
To date, no patient has re-presented with recurrent symptoms.
Conclusion
When problematic recurrent BXO occurs following failed medical treatment and circumcision, then a more radical combined option with appropriate reconstruction may be required.
TAKE HOME MESSAGE
-
BXO is a chronic, debilitating condition of the male external genitalia.
-
Medical management is often unsuccessful.
-
The disease frequently recurs following circumcision.
-
Radical surgery with appropriate reconstruction may be required.
References
1. Hallopeau H. Du lichen plan et particulierement desa forme atrophique. Ann derm Syph 1887;8:790.
2. Stühmer A. Balanitis xerotica obliterans (post-operationem) und ihre Beziehungen zur 'Kraurosis glandis et praeputii penis'. Archiv für Dermatologie und Syphilis 1928;156:613.
3. Ansari AZ, Hafeez S, Gallagher JJ, et al. Penile carcinoma secondary to balanitis xerotica obliterans and its compounding resultant pathologies: a case report. Cureus [Internet] 2024;16(5):e59555.
4. Cambridge University Hospitals NHS Foundation Trust. Balanitis xerotica obliterans (BXO) in boys – information for parents and carers [Internet].
https://www.cuh.nhs.uk/patient-information/
balanitis-xerotica-obliterans-bxo-in-boys
-information-for-parents-and-carers/
[accessed 12 February 2026].
5. Carocci K, Leslie SW, Hughes EC, McIntosh GV. Balanitis xerotica obliterans (male penile lichen sclerosus). StatPearls [Internet]. 2025.
https://www.ncbi.nlm.nih.gov/
books/NBK567770/
[accessed 12 February 2026].
6. Fox W, McKenna PH. Treatment algorithm for the comprehensive management of severe lichen sclerosus in boys based on the pathophysiology of the disease. J Pediatr Urol 2024;20:suppl 1:S66–S73.
7. Fuchs ME, Beecroft N, Dajusta DG, McLeod DJ. The association between BXO and obesity in boys undergoing circumcision. Glob Pediatr Health 2017;4:1–4.
8. Pandher BS, Rustin MHA, Kaisary AV. Treatment of balanitis xerotica obliterans with topical tacrolimus. J Urol 2003;170(3):923.
9. Rosemberg SK. Carbon dioxide laser treatment of external genital lesions. Urology 1985;25(6):555–8.
10. Navarette J, Echarte L, Sujanov A, et al. Platelet-rich plasma for male genital lichen sclerosus resistant to conventional therapy: first prospective study. Dermatol Ther 2020;33(6):e14032.
11. Hartley A, Ramanathan C, Siddiqui H. The surgical treatment of balanitis xerotica obliterans. Indian J Plast Surg 2011;44(1):91–7.
Declaration of competing interests: None declared.




