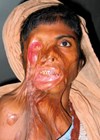
Burn injuries can affect any of us or our families at any time. A momentary lapse in attention can lead to a lifetime of scarring. Whilst any individual member of a family group can be physically scarred, all the family members will experience some form of psychological scarring. Causation is a complex problem and unfortunately there are a proportion of injuries related to mental health, alcohol, drugs, self-harm and malicious behaviour.
What is particularly distressing, for all involved in burns care, is the innocence of children with burn injuries and the devastating impact even such small injuries can have. My first exposure to such a patient was in 1984. In our Burns Unit at St Andrews in Billericay a four-year-old boy died with only a 4% scald three days after injury. Such was my first exposure to toxic shock syndrome. I spent the next few years researching and finding the cause, prevention and an active treatment for toxic shock and then embarked on research involving AlloSkinTM graft, hair follicle and composite flap allo-tissue transfer between humans and other novel ways to resurface burns. In 1989 I had the wonderful opportunity (supported by a Winston Churchill Fellowship), to visit many of the major burns units in the USA. I learned that early aggressive surgery is the way forwards to improve survival in massive burn injury, and young children can accept the results of burn injury better than adults, provided they receive appropriate care and attention. The problem in the USA was not how to keep burn victims alive but how to best rehabilitate and integrate the children into society.
Returning to the UK in 1990 I was one of two consultant plastic surgeons involved with treating paediatric burns at the North East Thames Regional Burns Unit, St Andrews Hospital, Billericay. I had previously been a junior surgeon training under my mentor, Consultant Plastic Surgeon, Mr Michael Hackett. During the 1980s Mr Hackett had contributed greatly to the improvement in the management of children with extensive burn injuries. More children were surviving but not only with physical scarring but also profound psychological injuries.
“How to improve or remove the burn scar appearance was the Holy Grail of the surgeon and was the focus of our research. We made great strides, but without really understanding the long-term psychological needs of the patient”
I have fond memories of the origin of the Burned Children’s Club, from which I became the Patron from 1990. Prior to the club, great support was offered at the Billericay Burns Unit until hospital discharge and thereafter a new medical team in outpatients took over the long-term care of the now scarred children. Before 1980 there was an adult Billericay Burn Club (BBC) but children were not members. There was not a purpose designed burns unit at this stage and those adults lucky to survive had been managed in isolation in single rooms on the general ward over many months, often in pain and forced to live in offensively smelling environments to avoid cross infection to general plastic surgery patients. The BBC was funded by charity donations and these contributed half of the original £10 million needed, the rest of the funding was matched by the NHS.
The Burns Unit catered for children and adults in separate rooms but with specialist nurse care. Sadly, 50% of admissions were young children often with avoidable accidental injury to face, trunk and limbs. After discharge from the Burns Unit, children, parents and families were confused and scared, arriving in hope of magical cures for the scars each time they visited the clinic at three monthly intervals. Often children would need frequent surgeries and scar releases to improve contracture, deformity and disability as they grew, but essentially once a burn scar had developed it was permanently there. Our procedures were mitigation. We operated on them frequently throughout the whole year without realising that if we operated on them during their school term-time we had withdrawn them from their formative days where they met their schoolfriends and formed relationships. We also removed them from education. Their wounds often needed time to heal, meaning more time off school. Without realising it we were denying them a future. Simple to understand now but it wasn’t even considered then.
How to improve or remove the burn scar appearance was the Holy Grail of the surgeon and was the focus of our research. We made great strides, but without really understanding the long-term psychological needs of the patient. We saw distress and pain in the years towards adulthood with often an inability to succeed at school, an inability to make friends and relative exclusion from a normal life. Burn injured children need to be converted from feeling that they are the unlucky victim of injury and blame, to feeling they are a fortunate survivor with special qualities and experiences, leading to a lifetime of future success. The child who survives a burn injury needs friends and family and a sense of support and respect. They don’t want sympathy. The holistic care of burn injured children needed to be rethought.
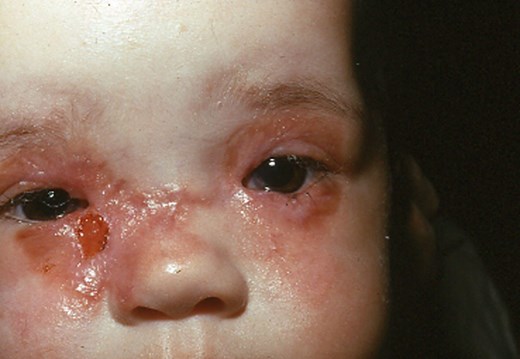
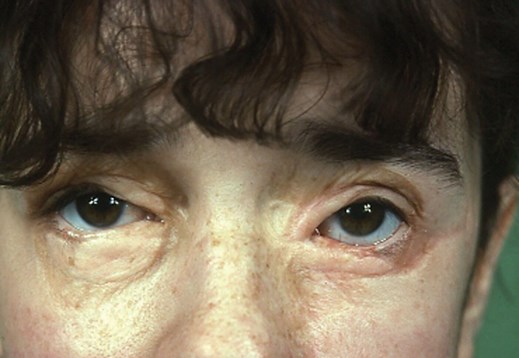
Photos of burns patient as a toddler following injury and as an adult after years of treatment.
In the early 1990s, Graham Locke, Pat Wade, her daughter Jane, and I met with the Burn Camp groups at the American Burns Association in New York and we realised what was actually needed in the UK. Thus, ‘The Burned Children’s Club’ was formed. There was no financial support from the NHS; the club was down to the hard work and total year-round dedication of Pat and those magical few who supported her. Their holidays were always with the Burn Camp Children and this selfless sacrifice and determination was the reason that Pat was awarded an MBE in 2002. Of course, many others also deserved recognition for their contribution, too many to mention but we know who they are and they are not forgotten. Donations came in and the first UK Burned Children’s camp at Graffham Water happened and was thereafter the annual focus of activity that supported survivors and their families constantly throughout the year. These burned children made lifelong friends with everyone involved with their burn care and especially with other survivors.
The helpers were volunteers with compassion and empathy wanting to give back to society and where better to contribute? These good people were not just workers on the Burns Unit, they also came from other walks of life and included survivor adult burn victims who could relate to the children themselves, firefighters, physiotherapists and many friends and family members of those connected with the Burns Unit, all of whom contributed their time unselfishly. Many of the burn injured children came from within the East London community with poor social housing and with financial need. Although scalds are the commonest injury in children, sari flame burns, acid burns, house fire burns and electrical burns were more prevalent in this community. Many were from ethnic minority groups. With inhalation injury and full thickness skin burns the children needed many painful operations to keep them alive. We worked hard to restore appearance and function and this was my job, but 20 plus major painful procedures would often be needed in these children and they needed long-term support and encouragement.

From left to right: David Gault, Michael Hackett and James Frame in 1988 celebrating a successful
Saturday training day for junior surgeons – the start of a change in approach to burn injury management.
The interface was the Burned Children’s Club and those dedicated people who supported it. Many serious burn injured children have gone on to become parents themselves, including our original massive burn injury survivor. You cannot imagine the immense emotional pride felt by those involved in the care of the children in these circumstances. It must be remembered though that not all burned children will survive injury and support is always needed for the bereaved parents and family members. The staff themselves also need support.
Our first major burn survivor at St Andrews was a 15-year-old boy with 95% body surface full thickness skin burns from flame injury. This was probably the largest burn size to survive in the UK at that time. Despite septic episodes and the ‘give up emotions’ within the patient himself and some staff members, we asked Penny Stephens, owner of Inflight at Stansted Airport for help. She liaised with Continental Airlines to arrange a complimentary medical transfer and we flew this boy over to Galveston in Texas for final rehabilitation. In a truly serendipitous moment my friend and colleague Peter Dziewulski was a fellow at the Shriners Children’s Hospital in Galveston at that time and helped look after our boy. Peter was to become my successor in the Burns Unit. We learned so much from this one episode and realised that we needed to offer this same resource in the UK. A whole host of other children survived burn injury, some with even small burns, but all needed the rehabilitation and support that the Burn Children’s club offered. Parents were integral to the success of the management. The Club started sending children and families abroad and engaging with other units keen to learn our model. These were the golden days of burns care in the UK.

Children line up for activities at one of the annual summer camps run by the Children’s Burns Club.
The Billericay Burns Unit transferred from Billericay to the Mid Essex Hospital in Chelmsford in 1996 and kept its St Andrews name and much deserved reputation as a world leader in burns care. It is a state of the art 20-bed facility with intensive care and a major research facility. We continued to develop cutting edge research with the Department of Experimental Dermatology at The Royal London Hospital, now known as The Blizzard Institute. More recently St Andrews has also become involved with research at the School of Medicine, Anglia Ruskin University, Chelmsford.

Pat Wade, whose determination and dedication helped so many families,
enjoying herself at one of the camps she helped to set up.
Suffice to say, Pat and the committee worked tirelessly all through the years from Billericay to date to get charity funding and continue to help burn injured children and their families. During the mid-1990s a group of investor angels from Price Waterhouse Cooper freely donated their time to help organise the Burned Children –‘Victims to Survivors’ Conference in Essex, which helped our understanding of how to better deal with the psychology of burn injury in children and also better understand the effects that the injury has on the parents and family. A professionalism developed within the charity to the benefit of the patients and their families.
With Pat retiring, the Burned Children’s Club changed its name to The Children’s Burns Club (not a name that I would have chosen but it satisfies the needs of burn victims and families) and is continuing to develop the ambitions of the founding members of the club. It is professionally led and is now a permanent feature within the world of burns care in the UK. It is now an integral part of the NHS. I was immensely proud to have supported Pat and her many friends and families who unselfishly spent a considerable part of their lives all day and every day for many years to help people in need; God Bless them all.
COMMENTS ARE WELCOME