Resection of skin lesions from the facial region is typically a straightforward procedure, yet the challenge arises in effectively closing the resulting deformity [1]. Surgeons frequently face hurdles, especially when the lesion occupies a restricted anatomical region with limited skin elasticity, or if the lesion is sizable [2].
Primary closure may be unachievable, local flaps might experience excessive tension with unsatisfactory scarring. Skin grafting is one option but typically results in poor cosmetic outcomes due to differences in skin colour and texture [2]. Moreover, there is a secondary morbidity at the donor site.
The paradigm of thought on the reconstructive ladder is as follows: (a) primary closure, (b) local flap closure, (c) skin grafting, (d) regional flap closure, (e) free flap closure in cases of extensive surgical defects [3]. While tissue expanders can provide additional stretched tissues allowing a primary tension-free closure after extirpation of the lesion, they do carry additional costs and time which make them quite impractical in various clinical settings where funding is limited. Healing by secondary intention is not a viable option for large defects.
It is prudent to ideally utilise adjacent tissue for the reconstruction with local flaps being utilised when primary closure is not feasible to have a contiguous match in skin colour and texture. Because the face is a critical area for reconstruction, we need to also consider how the final appearance of the surgical reconstruction will affect the patient’s appearance and self-esteem post-surgery.
The principle of skin closure without tension is of paramount importance for the healing process and the final cosmetic outcome. Can a tension-free primary closure of a significant defect of the face be achieved without distorting the facial features?
Case report
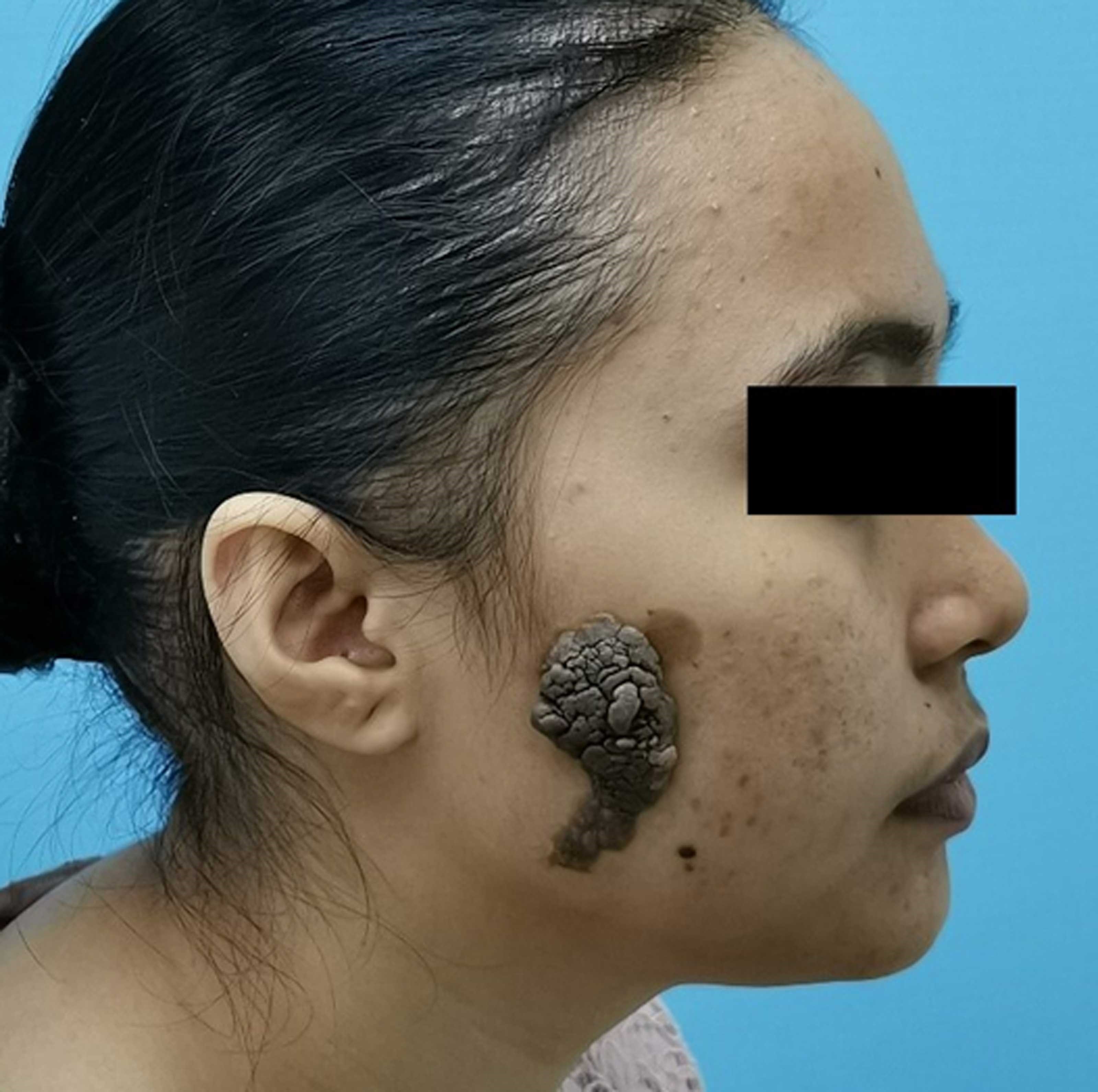
Figure 1: Large verrucous lesion overlying the right side of lateral cheek measuring 10 X 6cm.
A 19-year-old woman presented with a large verrucous lesion overlying the right side of her face. Clinical history revealed that the lesion was present at birth but gradually grew larger, thicker and became darkened during her teens. On examination, the lesion was non-tender but fixed to the underlying skin measuring 9 X 6cm (Figure 1). How would, or how should, you reconstruct this defect?
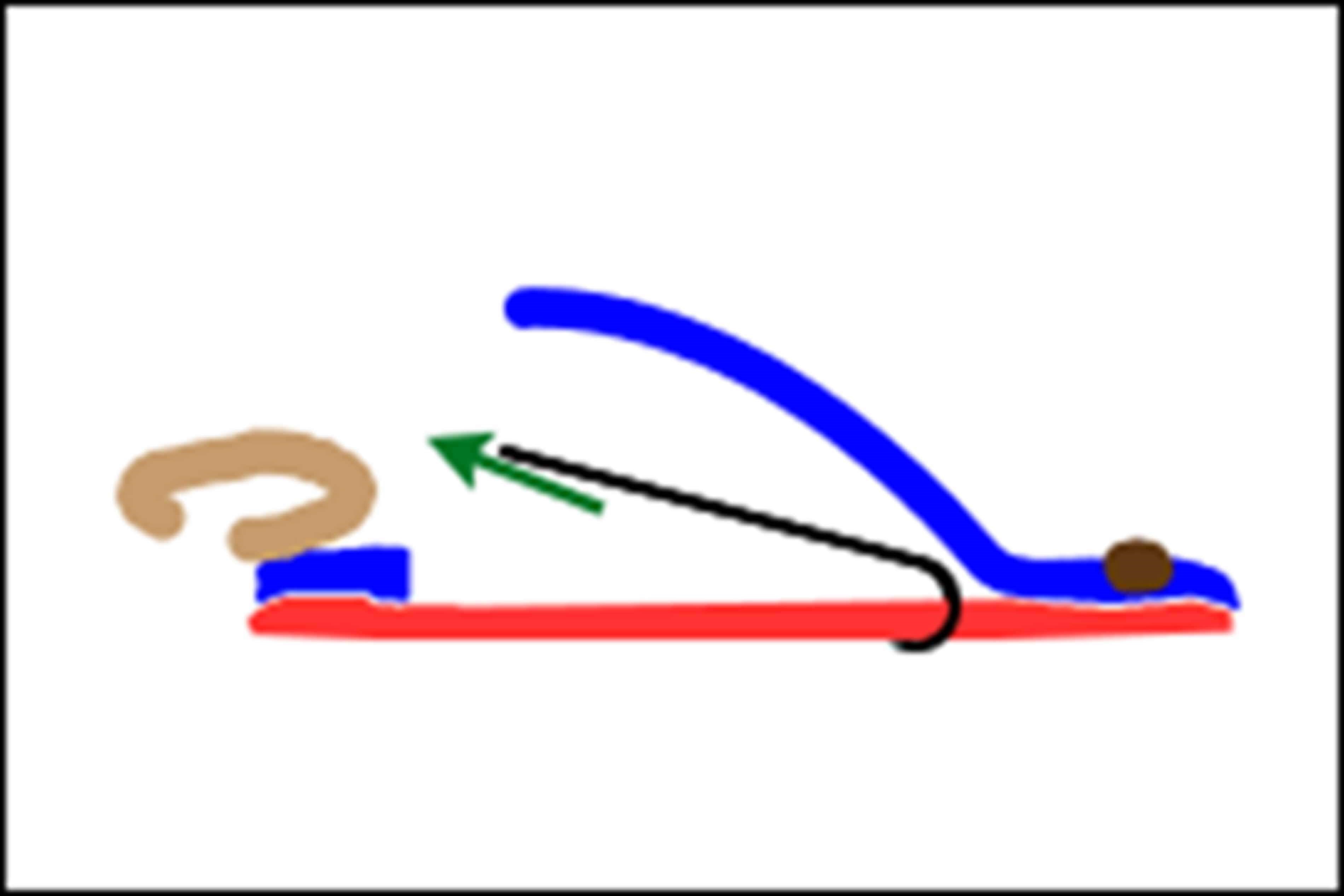
Figure 2: SMAS is represented in red; skin represented in blue.
The superficial musculoaponeurotic system (SMAS) is commonly described as an organised fibrous network consisting of the platysma muscle, parotid fascia, and a fibromuscular layer covering the cheek skin (Figure 2). This system separates the face’s deep and superficial adipose tissue and exhibits region-specific morphology.
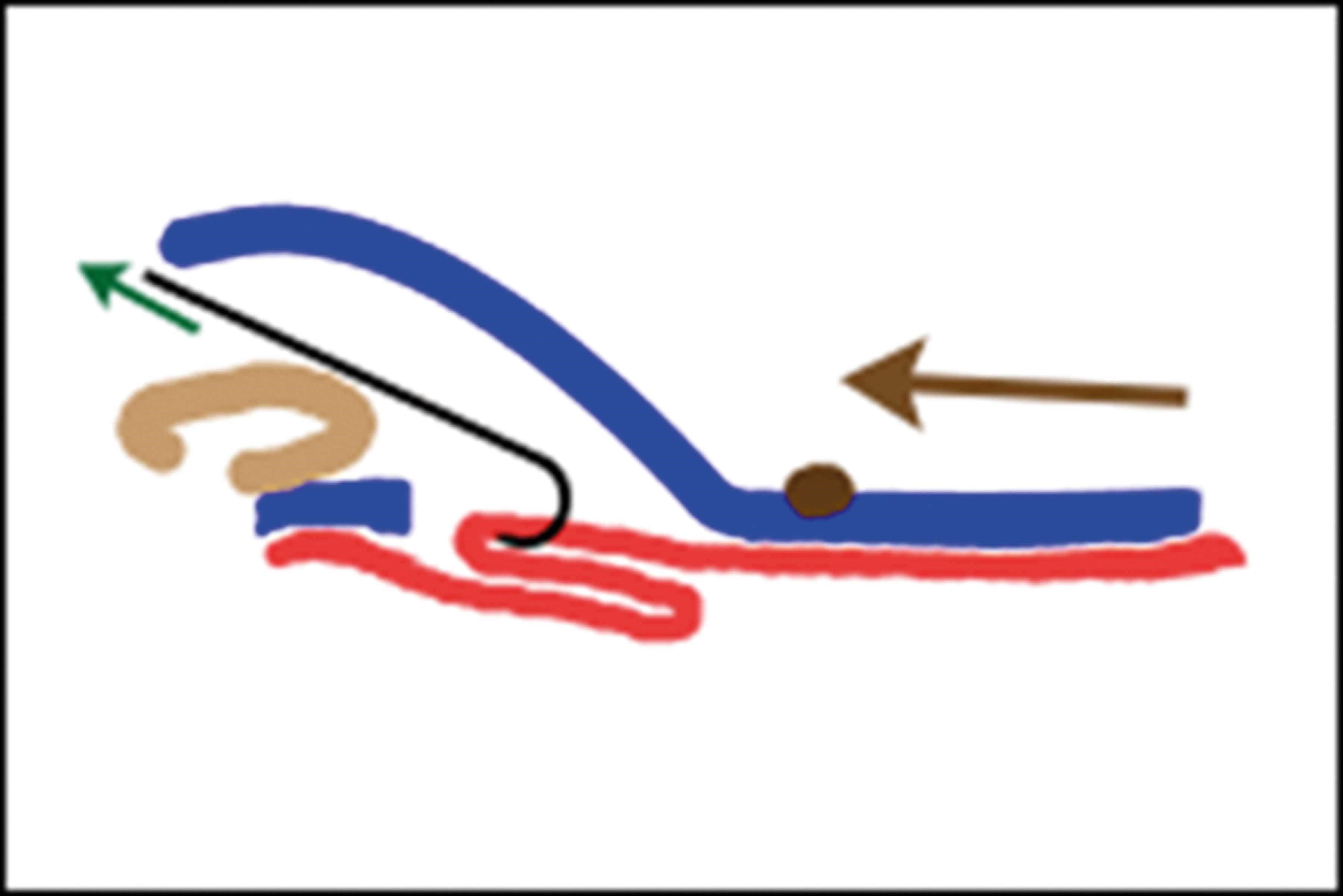
Figure 3: SMAS (red) is plicated while skin is re-draped and pulled.
The SMAS plication face-lifting technique, first described by Skoog in the 1970s [4] remains an effective method for suspending the soft tissues of the face, going beyond merely tightening the skin (Figure 3), and various adaptations of the technique have been described.
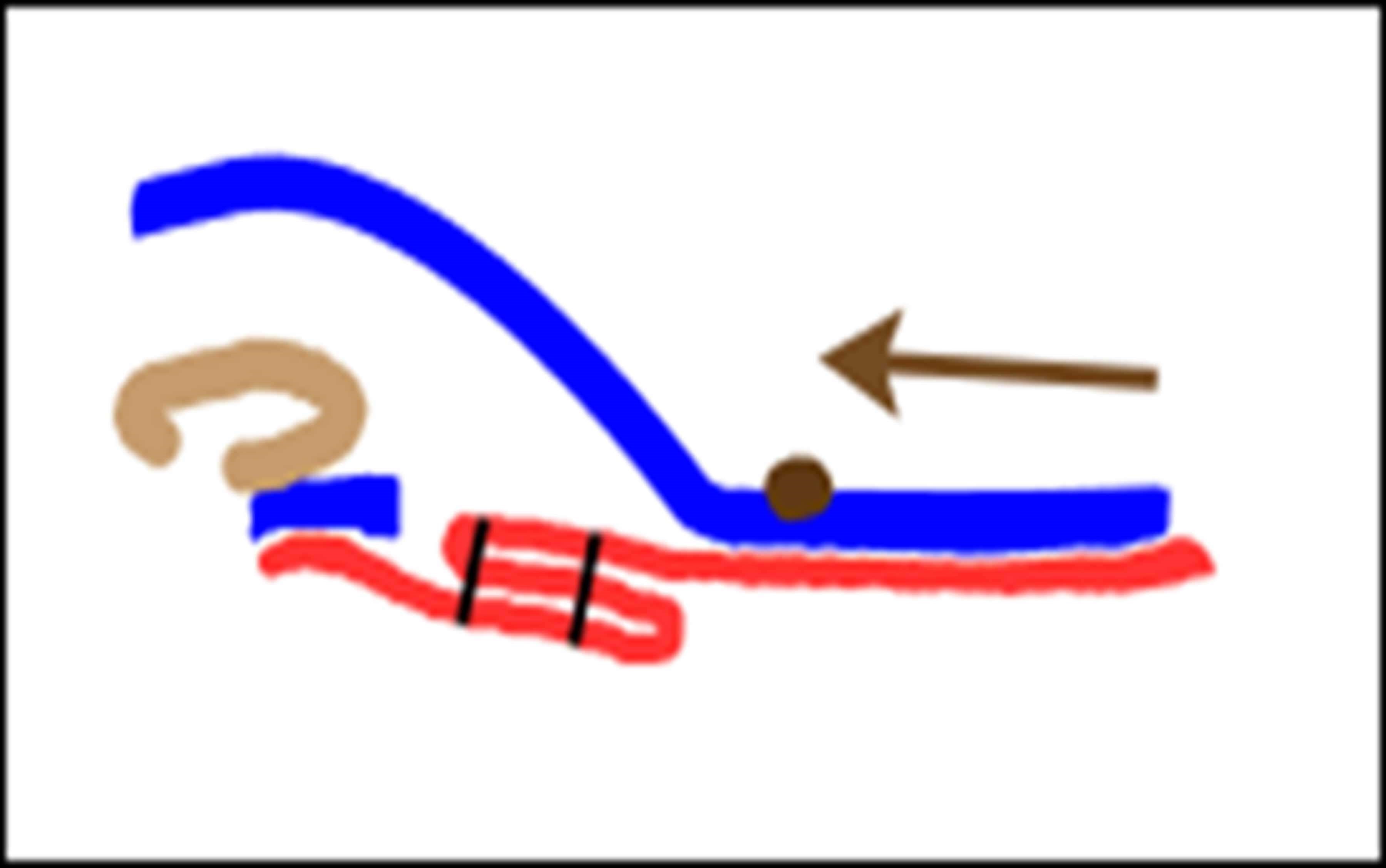
Figure 4: Plication of the SMAS results in excess skin (blue) that can be trimmed.
Suture plication creates an infolding of the SMAS (Figure 4), drawing SMAS from the lower part of the face up to the point where the sutures are placed [4]. Multiple sutures with customised vectors can be used, allowing the surgeon to tighten and reshape the facial SMAS to a more youthful appearance.
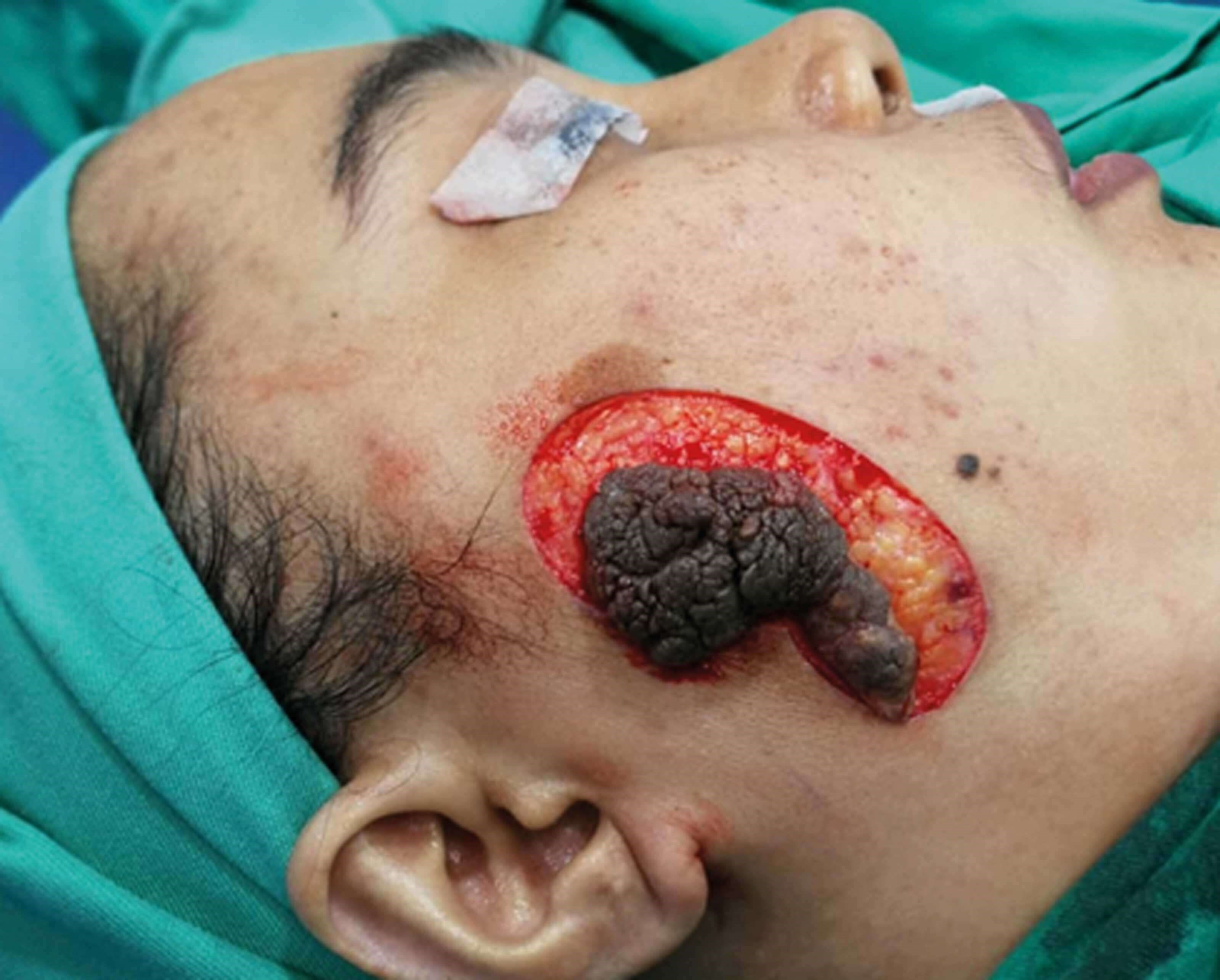
Figure 5: Excision of verrucous lesion.
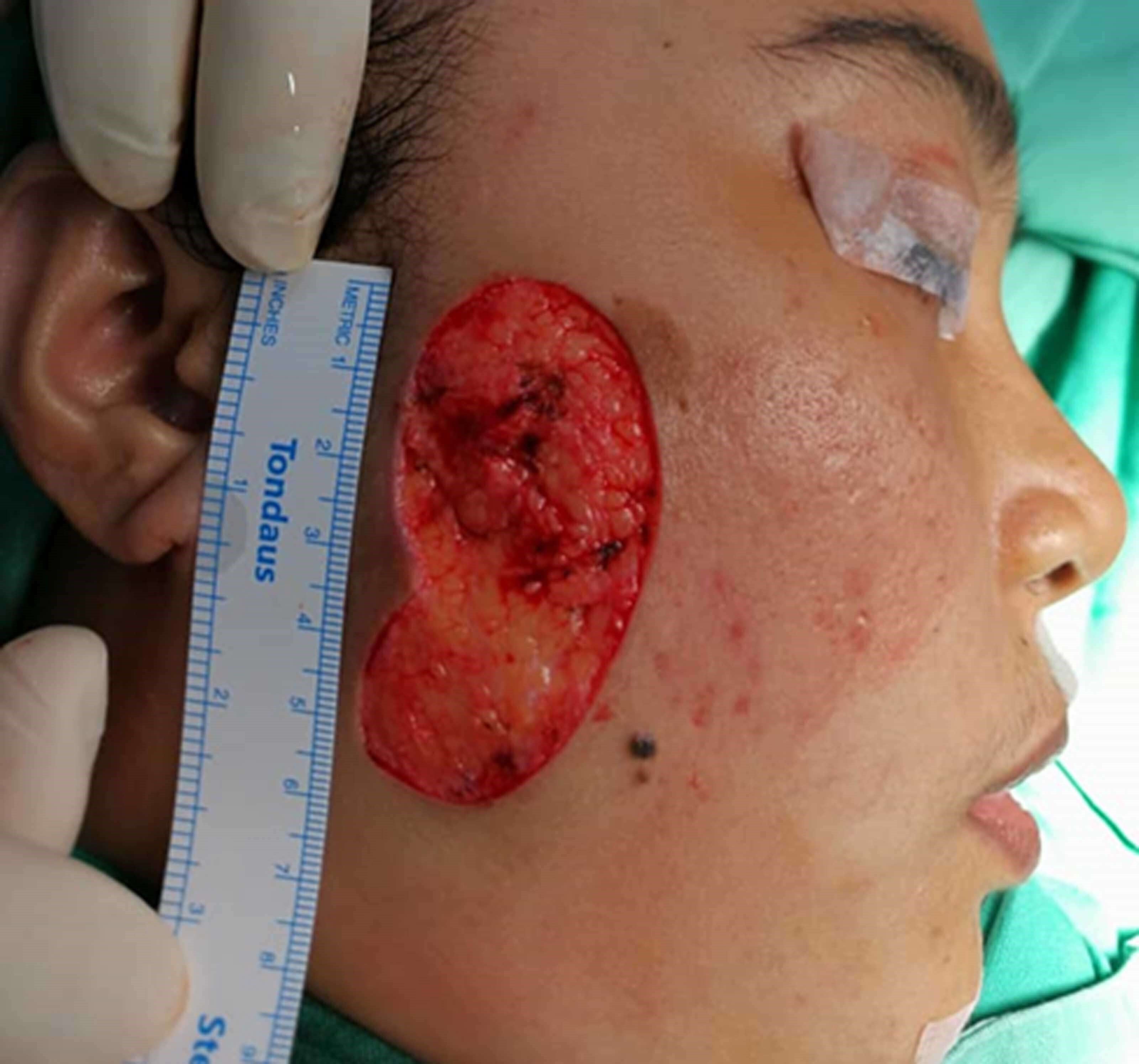
Figure 6: Defect left after excision of lesion.
Wide excision of the verrucous skin lesion resulted in a considerable soft tissue defect which was not possible to close primarily even after undermining of the subcutaneous tissues (Figure 5, Figure 6).
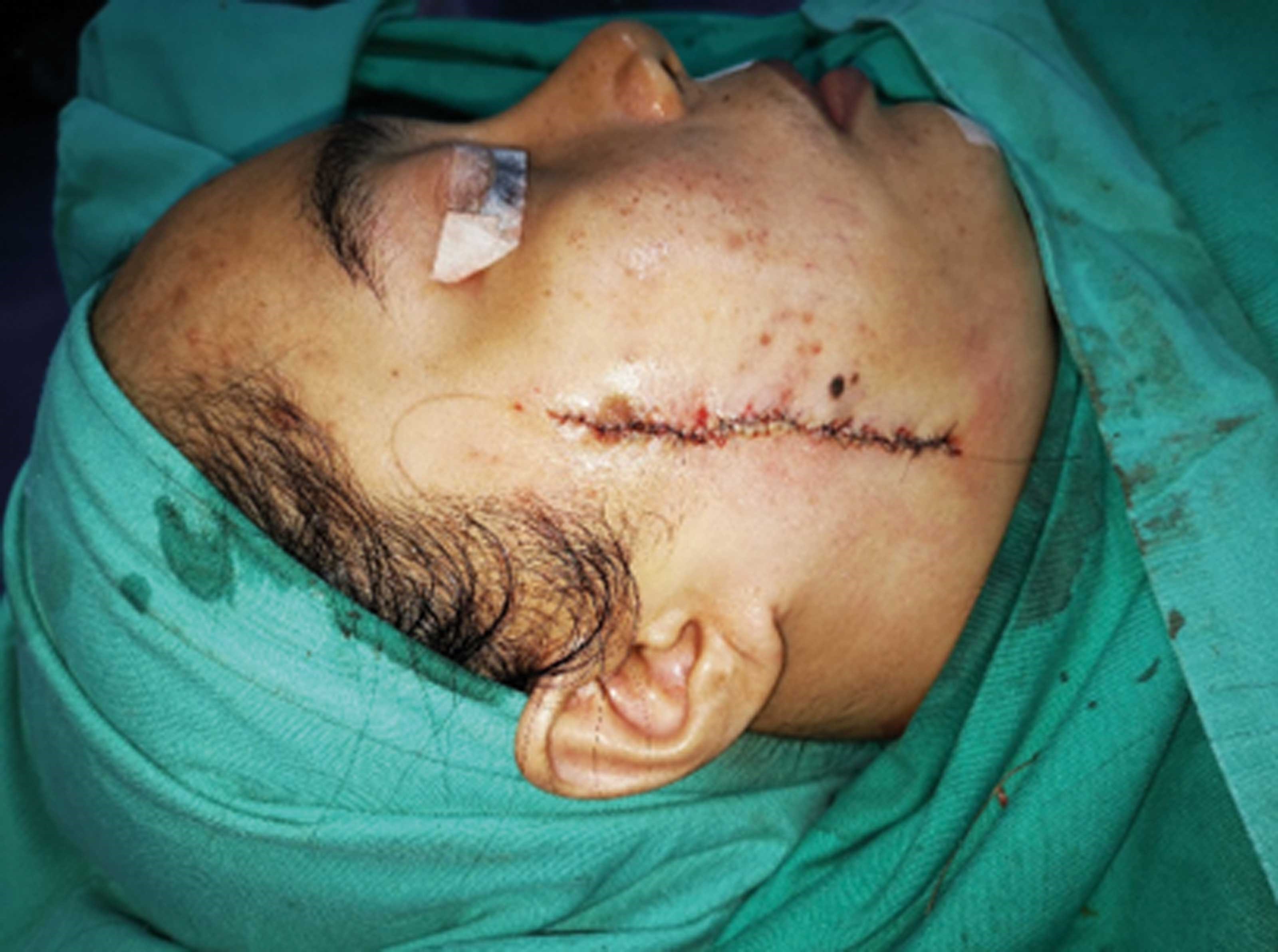
Figure 7: On table appearance of tension-free primary closure after excision of lesion.
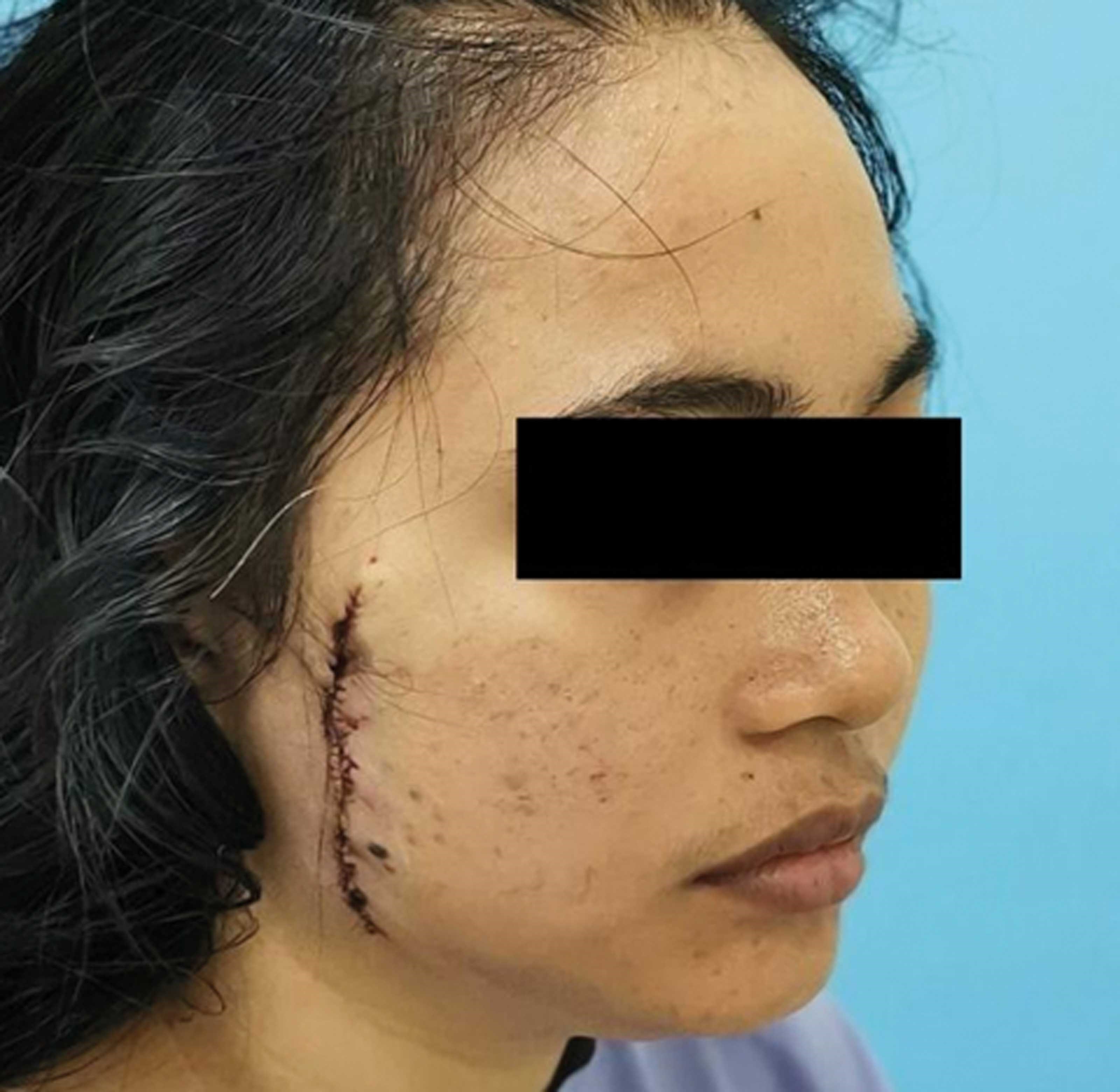
Figure 8: Immediate post-surgery appearance.
Plication of the SMAS with multiple 2-0 Vicryl sutures was carried out in a 45 degrees vector allowing the skin edges to approximate each other with virtually no tension (Figure 7). The SMAS plication shortens the distance between the skin defect and relieves the tension to allow a primary closure that does not distort the facial features (Figure 8). This also prevents the need to resort to more extensive local type flaps such as the cervicofacial flap that result in longer unsightly scars. D’Arpa described a method of using a facelift incision and SMAS plication technique to reconstruct temporofrontal defects post extirpation surgery [5]. In our technique, there is no need for a facelift incision as the skin undermining is done through the defect and plication done directly through the defect to approximate the edges.
Our technique also differs from the ingenious ‘flicklift’ technique which uses an inverted L- shaped SMAS flap which is suspended using a ‘figure of eight suture’ to the deep temporal fascia [6]. Our technique does not require any undermining of the SMAS and has no requirement for anchoring to the deep temporal fascia thus allowing novice surgeons to easily learn and perform this procedure.
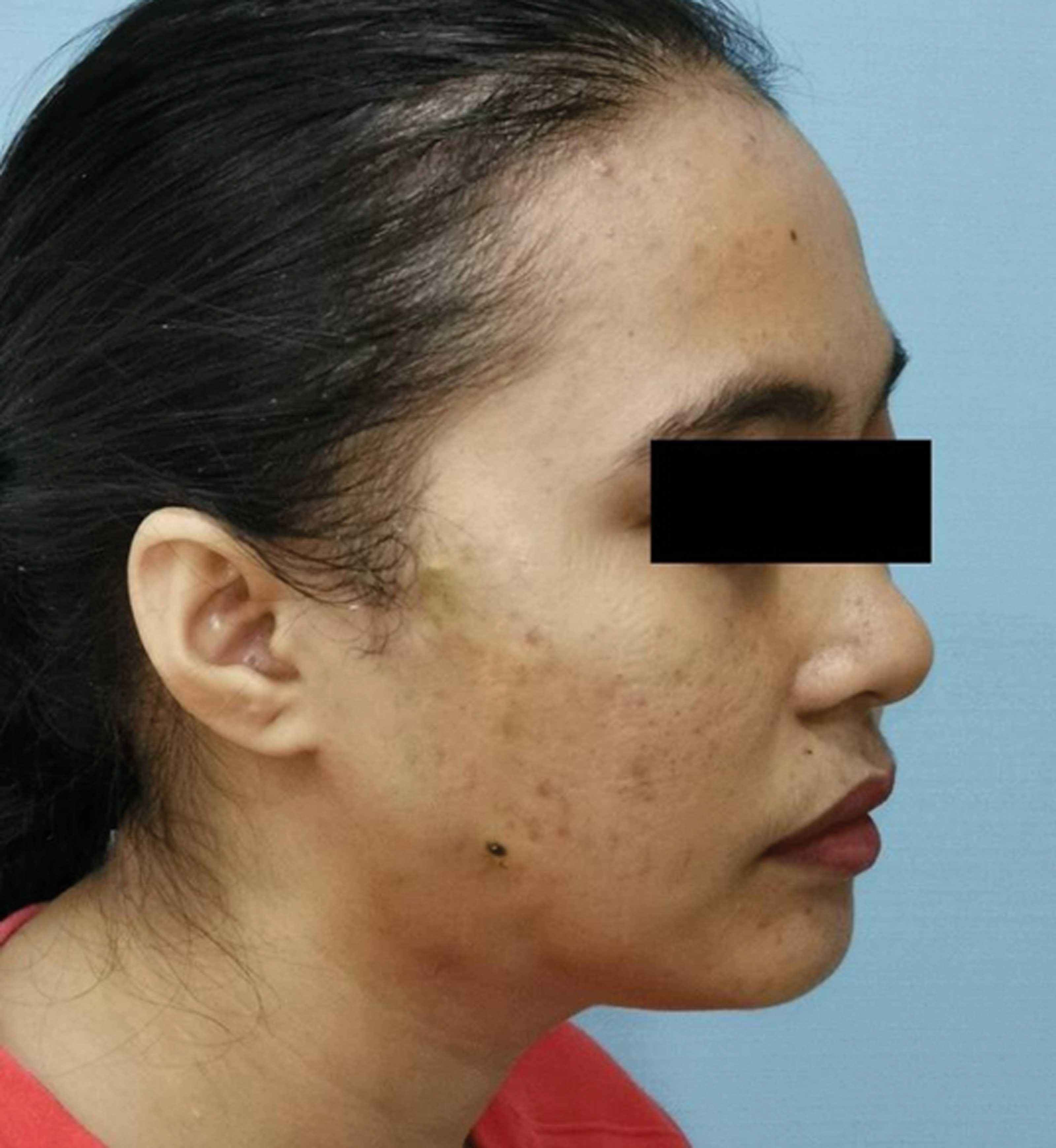
Figure 9: Patient review at eight-months post surgery showing excellent cosmetic results.
Excellent long-term scar results eight months postop validate the usefulness of using the technique of plication of the SMAS to allow primary closure of large facial defects without undue tension (Figure 9).
Discussion
Facial skin lesions present unique challenges in terms of reconstruction due to the critical aesthetic and functional considerations involved. While smaller defects can often be managed through primary closure or local flap techniques, larger or more complex defects require innovative approaches to achieve optimal outcomes.
In this case report, we describe a technique utilising facelift-type plication of the SMAS to facilitate tension-free primary closure of a large facial defect resulting from excision of a verrucous lesion.
The SMAS plication technique described herein offers several advantages over traditional approaches. By infolding and tightening the SMAS layer, the distance between the skin defect edges is reduced, thereby allowing for primary closure without undue tension. This technique effectively addresses the primary concern of minimising tension across the wound, which is crucial for optimal wound healing and cosmesis. Furthermore, it obviates the need for skin grafting or more extensive local flaps, which may result in suboptimal cosmetic outcomes and donor site morbidity. Skin grafting should be avoided for facial defect reconstruction because of the difference in skin tone, skin colour and skin thickness. It is imperative we take into consideration how the final appearance of the surgical reconstruction will affect the patient’s facial appearance and self-esteem post surgery when we plan for surgical intervention.
The adaptability of the SMAS plication technique is noteworthy, as it can be customised to address defects of varying sizes and locations on the face. The use of multiple sutures with customised vectors allows for precise control over tissue tension and reshaping, facilitating the achievement of aesthetically pleasing outcomes. SMAS plication can also be done after excision of smaller facial skin lesions to decrease the tension of closure for an improved quality scar.
Comparisons can be drawn between our approach and other techniques described in the literature, such as the flicklift technique, which utilises an inverted L-shaped SMAS flap anchored to the deep temporal fascia. While both techniques aim to address facial defects through SMAS manipulation, our technique offers simplicity and ease of implementation, making it a viable option for surgeons seeking efficient and reliable methods of facial reconstruction.
The long-term cosmetic results observed in this case, as evidenced by the excellent scar outcomes at eight months postoperatively, underscore the effectiveness and durability of the SMAS plication technique. By achieving tension-free primary closure and preserving facial aesthetics, this approach enhances patient satisfaction and quality of life postoperatively.
In conclusion, the utilisation of SMAS plication for facial defect reconstruction represents a valuable addition to the armamentarium of reconstructive techniques available to surgeons. Its simplicity, effectiveness, and reproducibility make it a promising option for addressing challenging facial defects while optimising cosmetic outcomes and patient satisfaction. We have successfully used this technique to close various face defects and for scar revision cases in plastic surgery. Further studies and long-term follow-up are warranted to validate the efficacy and versatility of this technique across a broader range of clinical scenarios.
References
1. Rabbani CC, Hwang MS, Byrne PJ, Desai SC. Management of Large Facial Defects. Facial Plast Surg 2020;36(2):148–57.
2. Heller L, Cole P, Kaufman Y. Cheek reconstruction: current concepts in managing facial soft tissue loss. Semin Plast Surg 2008;22(4):294–305.
3. Meaike JD, Dickey RM, Killion E, et al. Facial Skin Cancer Reconstruction. Semin Plast Surg 2016;30(3):108–21.
4. Skoog T. Plastic Surgery: New Methods and Refinements. Philadelphia, Pa: WB Saunders Co; 1974.
5. D’Arpa S, Cordova A, Pirrello R, et al. The face lift SMAS plication flap for reconstruction of large temporofrontal defects: reconstructive surgery meets cosmetic surgery. Plast Reconstr Surg 2011;127(5):2068–75.
6. Klaassen MF, Frame JD, Levick P. Aesthetica in practice: the flick lift in assisting closure of large cutaneous excisional defects on face. Clin Surg 2017;2:1684.