This article has been verified for CPD. Click the button below to answer a few
short questions and download a form to be included in your CPD folder.
In this feature article, we discuss our experience in masculinising chest wall surgery (aka ‘top surgery’) in transgender and gender diverse adults requesting gender affirming surgery with the aim of better aligning their body with their gender identity.
Transgender persons account for 0.4-1.3% of the population, and gender affirming treatments and surgical options are constantly evolving in approach and technique [1].
International guidance exists for delivering best possible care with regards to various aspects of transgender health, including the decision-making and holistic care surrounding masculinising chest wall surgery. This guidance is the World Professional Association for Transgender Health (WPATH) Standards of Care, currently in its eighth edition [2].
We are closely guided by WPATH as well as the Gender Reassignment Protocol outlined by the Scottish Government when delivering care [3]. National Health Service options exist within Scotland, but our experience as set out in this feature is in the private sector.
Transsexualism and gender dysphoria are complex presentations which require careful evaluation, a holistic approach, multidisciplinary care, and patient-centred shared decision-making over a prolonged period of time. This article focuses on female to male transition, which is multifactorial and often involves hormone therapy, speech therapy and psychotherapy as well as surgical interventions.
Assessment for suitability for surgical intervention
Decision-making concerning surgical management requires careful evaluation and ongoing discussion with the patient over a period of time. Surgical intervention is irreversible; therefore, guidance concludes that the patients’ gender diversity must be sustained over time, with the patient living in their chosen gender role for at least 12 months before surgery. This allows time to truly experience living in their chosen gender and allows social adjustment, with multiple reviews and check in opportunities with the Gender Identity Clinic. This allows the patient to postpone or alter the decision for surgery.
The patient also needs to meet the diagnostic criteria for gender incongruity and needs to have the ability to provide informed consent. Any mental health concerns that have not previously been addressed or may interfere with the ability to understand or consent to treatment must be addressed.
In our practice, we ensure that our patients have two confirmations of gender dysphoria diagnosis before offering surgery. One of these is from a gender specialist doctor and the other either from a psychologist or psychiatrist with expertise in this area.
It is important to ensure that the patient journey is as supported as possible, with flexibility and options to delay surgical intervention or make changes to their pathway.
Regular psychotherapy and counselling are encouraged throughout the patient journey, and every attempt is made to facilitate inclusion of families, partners and carers. It is acknowledged that patients with gender dysphoria often have concomitant psychiatric diagnoses [4]. In our patient cohort, retrospective study found that 65.6% of patients had at least one psychiatric diagnosis noted at their preoperative consultation, and 27.9% of patients reported previous self-harm. It is essential that this cohort receives ongoing psychological support throughout their patient journey.
Surgical options
Masculinising chest wall surgery in the form of bilateral mastectomy is often carried out early in the gender reassignment pathway due to the risk of morbidity from breast binding such as pain, shortness of breath and detrimental impact on exercise tolerance. Studies have shown abnormal baseline lung function in individuals wearing chest binders [5]. It is also acknowledged that testosterone therapy can make breast binding more uncomfortable [3].
Surgical techniques offered in our unit include bilateral mastectomy with free nipple grafts (most common), bilateral mastectomy via peri-areolar incision, bilateral mastectomy with no nipple, and bilateral mastectomy with pedicle nipple flap. Choice depends on patient preference and breast tissue volume and ptosis [6,7].
Our most popular option is the bilateral mastectomy with free nipple grafts, whereby we harvest nipple grafts which are 25mm in diameter and adjust them to reduce nipple volume and projection. These are kept for repositioning once the bilateral mastectomy is complete.
Symmetrical incisions are made at the intramammary fold, and the breast is lifted from the pre-pectoral fascia. Symmetrical superior incisions are also made and a superior dissection carried out to the upper glandular limit in the breast fat plane.
We quilt the flap with a running STRATIFIX™ suture to the prepectoral fascia to reduce risk of seroma. We do not routinely use drains. STRATIFIX is a barbed suture which self-locks without need for knotting and also has antibacterial technology (coated with triclosan) to reduce risk of infection, in particular MRSA and MRSE [8]. Wound closure is with an absorbable suture (MONOCRYL®).
We use a triangulation technique to confirm accurate nipple positioning at a level that equates to the fourth intercostal space on preoperative and intraoperative markings, and also to maximise scar symmetry.
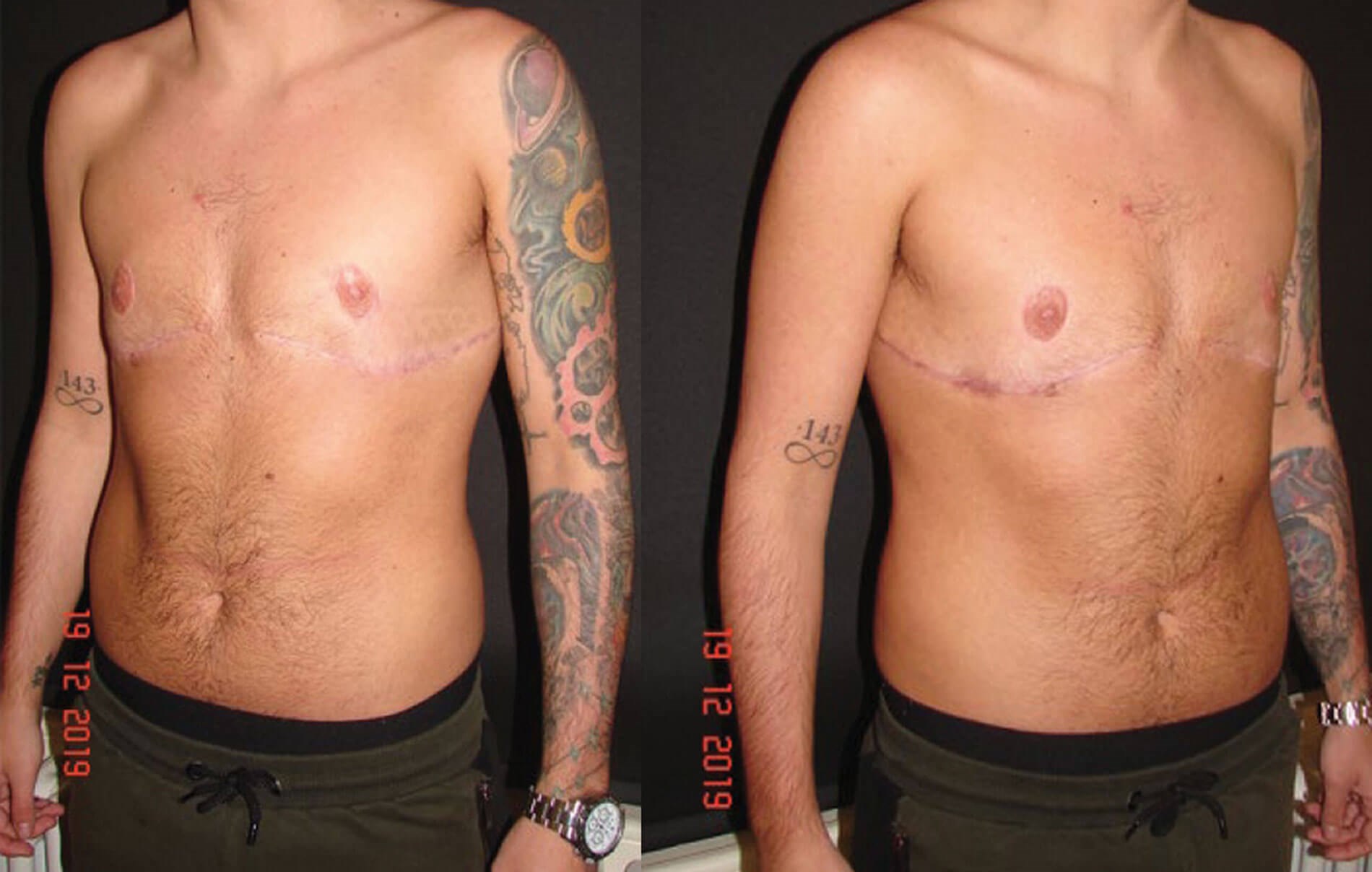
Figure 1: Bilateral mastectomy with free nipple grafting.
The majority of our patients undergo this surgery as a day-case procedure, and the remainder have a one-night hospital stay. This difference is usually accounted for by the time of surgery. We have evaluated our complication rates which are low and comparable with published literature, and our revision rates are lower than those reported in a recent systematic review [9].
The peri-areolar technique avoids skin resection and is best suited to patients with low volume of breast tissue. It avoids scars in the inframammary fold region in suitable patients.
Possible complications of top surgery include systemic complications (such as complications of general anaesthetic, venous thromboembolism (VTE) and pneumonia), general complications relating to breast surgery (including bleeding, infection, pain, haematoma, seroma) and complications specific to top surgery for masculinisation including dog ears, nipple distortion, abnormal or unsightly scarring, fat excess, nipple graft failure and need for revision surgery.
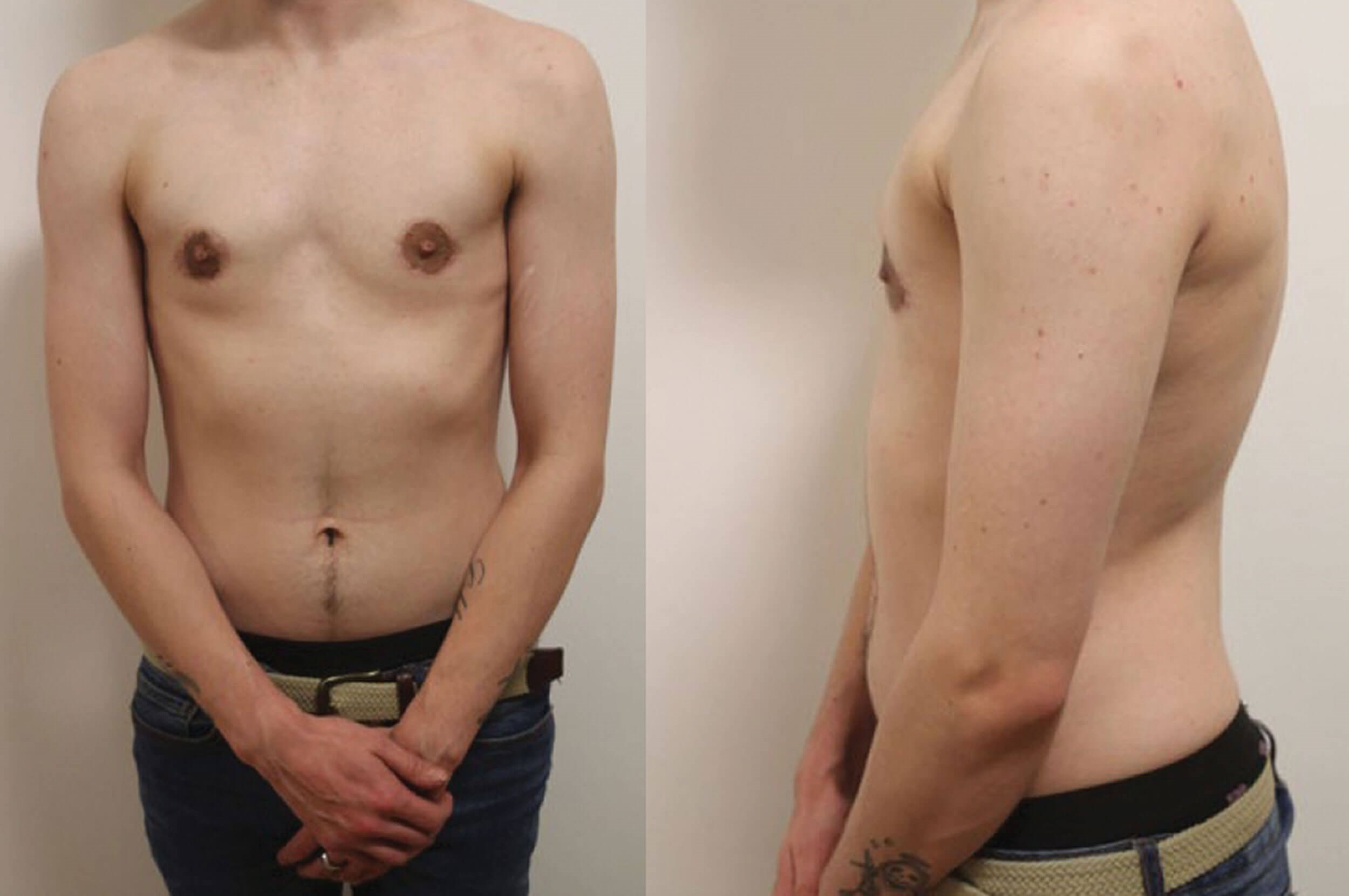
Figure 2: Bilateral mastectomy via peri-areolar incision.
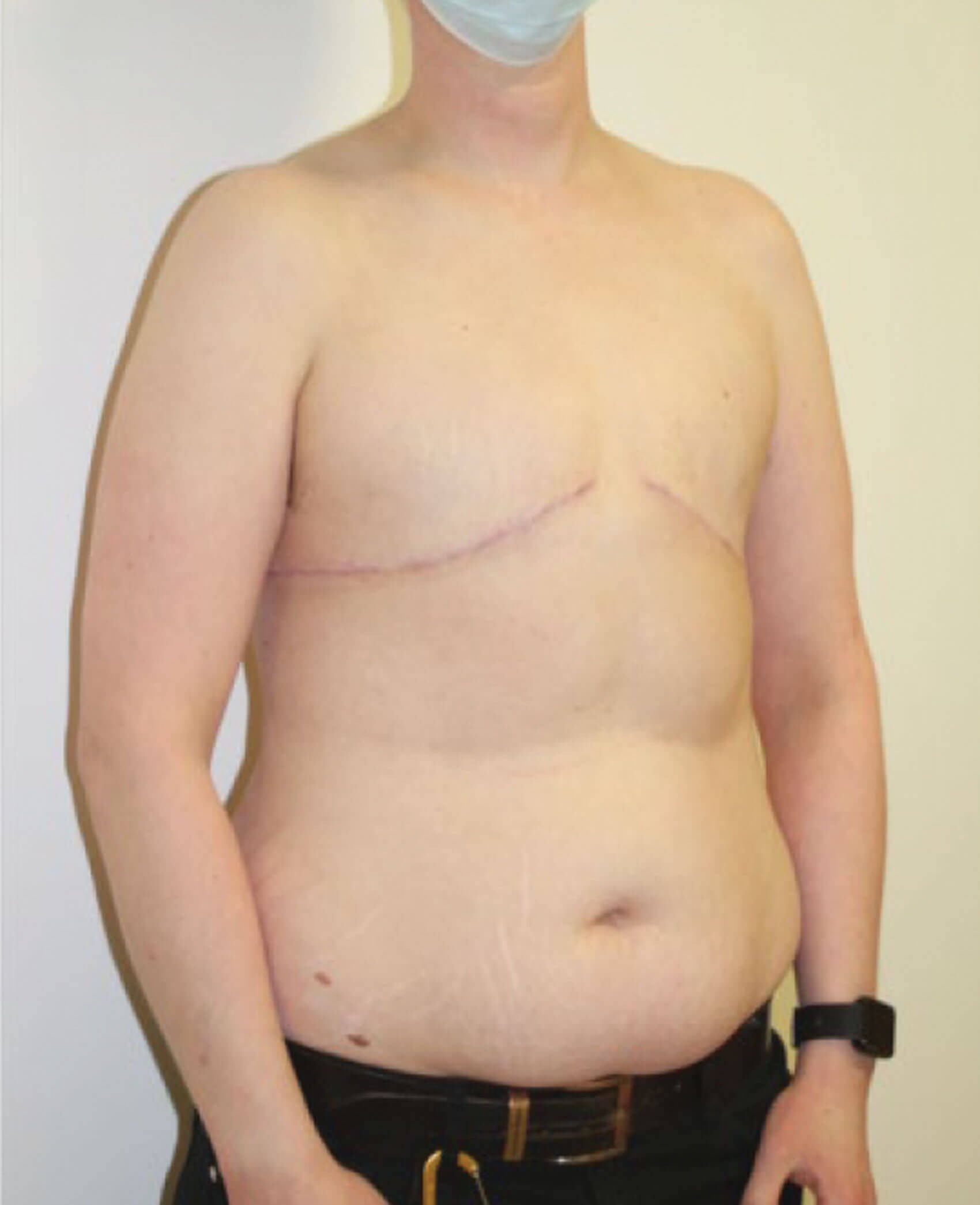
Figure 3: Bilateral mastectomy with no nipple placement in a non-binary patient who
prefers to neither have a feminine or masculine appearance of chest wall.
All patients are risk-assessed for deep vein thrombosis using the Caprini Score system, and those with a score of greater than five receive low molecular weight heparin (prophylactic dose) for 10 days [10]. We follow our patients up in the dressings clinic one week after surgery, with subsequent visits over the following three weeks. For free nipple graft patients this will include a graft check. The final outcome is assessed in the clinic three months post operation.
Postoperative outcome examples from our patient cohort
Our outcomes review showed low complication and revision rates. On this page and the following there are some clinical photographs showing outcomes through various approaches.
Holistic care and other health considerations
It is important to consider breast cancer risk in this population. WPATH guidelines emphasise that surgeons should assess patients for risk factors for breast cancer preoperatively, and screening guidelines must be followed.
There is currently no provision for those who are reassigned from female to male gender to remain in the breast screening programme following gender affirming surgery. This is a complex area as some breast tissue will remain in the superior aspect, left deliberately to create a pectoral ridge.
The majority of patients undergoing top surgery are also receiving hormone therapy in the form of androgens (intramuscular (IM) testosterone enanthate, topical Testogel® or oral / IM testosterone undecanoate).
Testosterone is continued for life if there are no medical contraindications, but regular liver function tests are required as there is a risk of liver dysfunction with testosterone therapy. There is documented evidence that testosterone therapy improves bone density and reduces osteoporosis risk, in short-term follow-up [11].
Some surgeons advocate stopping testosterone therapy for four weeks prior to surgery, and restarting one week postoperative due to possible increased VTE risk. However, Scottish guidance suggests continuing testosterone therapy throughout surgical management, and that is also our practice. We have had no incidence of VTE in our cohort, and there is recent evidence to suggest that testosterone is not procoagulant, compared to oestrogens given to transwomen [12].
Conclusion
Masculinising chest wall surgery allows for significant improvement of quality of life by contributing to better alignment of the patients’ body with their gender identity.
As well as considering best surgical technique for the patient and their presenting breast shape, it is essential to take a holistic multidisciplinary approach and ensure certainty of diagnosis of gender dysphoria, ability to consent, and stability of mental health leading up to surgery.
The senior author has carried out over 60 masculinising chest wall surgeries in recent years in our unit, with good outcomes comparable with published literature, and we recommend adaptive techniques as described for improved outcomes including triangulation for accuracy of nipple placement and to maximise scar symmetry and quilting for reduction of seroma placement.
In the near future, we look to carry out a formal Patient Reported Outcome Measure (PROM) for our patients to assess impact on quality of life.
References
1. Zucker KJ. Epidemiology of gender dysphoria and transgender identity. Sex Health 2017;14(5):404-11.
2. Standards of Care for the Health of Transgender and Gender Diverse People, Version 8 (WPATH 8th Edition 2022). International Journal of Transgender Health 2022;23(S1):S1-S258.
3. Gender Reassignment Protocol, The Scottish Government, CEL 26(2012)
www.sehd.scot.nhs.uk/mels/
CEL2012_26.pdf
4. Paz-Otero M, Becerra-Fernández A, Pérez-López G, Ly-Pen D. A 2020 review of mental health comorbidity in gender dysphoric and gender non-conforming people. Journal of Psychiatry Treatment and Research 2021;3(1):44-55.
5. Cumming RJM, Sylvester K, Fuld J. Understanding the effects on lung function of chest binder use in the transgender population. Thorax 2016;71:A227.
6. Ammari T, Sluiter EC, Gast K, Kuzon WM Jr. Female-to-male gender-affirming chest reconstruction surgery. Aesthetic Surgery Journal 2019;29(2):150-63.
7. Etemad SA, Furuyama WM, Winocour JS. Double incision mastectomy with free nipple graft for masculinizing chest wall surgery (Video). PRS Global Open 2020;8(11):e3184.
8. www.jnjmedtech.com/en-US/product/
stratafix-spiral-knotless-tissue
-control-device/barbed-suture
9. Wilson SC, Morrison SD, Anzai L, et al. Masculinising top surgery: a systematic review of techniques and outcomes. Annals of Plastic Surgery 2018;80(6):679-83.
10. Cronin M, Dengler N, Krauss ES, et al. Completion of the updated Caprini risk assessment model. Clin Appl Thromb Hemost 2019;25:1076029619838052.
11. Stevenson MO, Tangpricha V. Osteoporosis and bone health in transgender persons. Endocrinol Metab Clin North Am 2019;48(2):421-7.
12. Scheres LJJ, Selier NLD, Nota NM, et al. Effect of gender affirming hormone use on coagulation profiles in transmen and transwomen. J Throm Haemost 2021;19(4):1029-37.
[All links last accessed February 2023].
Declaration of competing interests: None declared.
COMMENTS ARE WELCOME