A smooth convexity from the lower eyelid to the upper cheek with flawless skin is considered a desirable feature and a sign of youth. The opposite leads to ‘shadows’ around the eyes and a tired appearance or sunken eyes.
Patient selection
Lipp et al. suggested the acronym OCULAR to denote the following: Osseous, Colour, Underlying anatomy, Laxity, Adipose, Rhytides [1]. To this I would add maxillary projection assessment from the convexity of the eye (closed) to the maximum projection of the maxilla. A positive vector would imply a pure treatment of the periocular area. A negative vector in my experience implies poor aesthetic results unless the maxillary area is augmented. Blueish tinged skin in Fitzpatrick skin types 1-3 rarely improves with treatment.
Prominent fat pads can be visualised with ultrasound. Fillers should not be injected into the pad as these would worsen the appearance. These should be assessed on a case-by-case basis and filler placed around the fat pad in a camouflaging pattern.
Rhytides can be softened with botulinum toxin and skin boosters. I would recommend starting with those prior to attempting to treat the tear trough with fillers themselves. Such treatment can take up to three months to be effective and the patient needs to be informed at the outset.
Choice of product
A very low G prime reticulated hyaluronic acid (HA) filler is used. Some experts use calcium hydroxylapatite (CaHA). The advantage of the latter is its being minimally hygroscopic. In my experience of trying almost every major brand of filler available, I would say all low G prime fillers perform equally well.
Dosage of product
It is common consensus to start with 0.5ml per side. However, in my experience the dose is dependent on the assessment of the tear trough and a dogmatic approach is to be avoided. I find it wise to avoid more than 1ml per side.
Requirements
- HA or CaHA filler
- Cannula 38mm 25 G
- Disinfectant (my preference is to use NatraSan Skin as some other disinfectants are not suitable for this delicate area)
- Sterile gloves
- Good lighting
Assessment
The patient is assessed sitting upright looking up. Good photographic documentation at 45, 90 and 180 degrees are obtained. A thorough medical history is obtained to assess suitability.
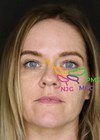
The cheeks are assessed for convexity by drawing a line from the most anterior part of the cornea perpendicular downwards. A negative vector to the maxilla implies that optimal results will only be achieved if the maxilla is treated.
The skin is tested for laxity using the ‘snap test‘ where the skin recoil is observed. Poor candidates are those with very loose skin. Pigmentation is also assessed.
The presence of malar oedema is noted (this is a predictor of poor cosmetic results).

Before and after images from the author’s practice.
Technique
These techniques are suitable for both HA and CaHA.
A line is drawn from the lateral canthus perpendicularly downwards. Another line is drawn from the medial canthus along the nasojugal groove. The entry point of the cannula will be at the intersection. The product needs to be deposited supraperiosteally. The cannula is advanced to the medial canthus. Placement and depth can be checked by lifting the cannula and checking its outline. Ultrasound can also be used for this purpose. The filler is then deposited in small aliquots while moving the cannula back and forth along the tear trough. The same entry port can be used for treating the palpebromalar groove.
Deeper tear troughs class II and III, might benefit more from a ‘sandwich technique’, whereby small 0.05 aliquots of filler are deposited along the margins of the nasojugal groove, supraperiosteally, by serial puncture at 90 degrees to the skin with a 30G needle. Prior ultrasonic vascular mapping is essential. This is followed by the above technique.
The patient is then reviewed after three weeks. Class I and II (Hirmand classification of the nasojugal sulcus [2]) would most likely be treated by a single intervention. In my experience, class III tear troughs often need further treatment by repeating the above or depending on personal judgement, the use of blended HA or CaHA more superficially. I normally blend with 0.9% saline in a 1:1 solution. Placement of product is ideally assessed via ultrasound.
References
1. Lipp M, Weiss E. Nonsurgical treatments for infraorbital rejuvenation: a review. Dermatol Surg 2019;45(5):700-10.
2. Hirmand H. Anatomy and nonsurgical correction of the tear trough deformity. Plast Reconstr Surg 2010;125:699-708.
Further reading
1. D’Amato S, Fragola R, Bove P, et al. Is the treatment of the tear trough deformity with hyaluronic acid injections a safe procedure? A systematic review. Appl Sci 2021;11(23):11489.
2. Sharad J. Treatment of the tear trough and infraorbital hollow with hyaluronic acid fillers using both needle and cannula. Dermatologic Therapy 2020;33(3):e13353.
3. Hassan G. Treating tear troughs: soft tissue augmentation. Practical Dermatology 2013;43-6.
4. Funt DK. Avoiding malar edema during midface/cheek augmentation with dermal fillers. The Journal of Clinical and Aesthetic Dermatology 2011;4(12):32-6.
Declaration of competing interests: None declared.
COMMENTS ARE WELCOME