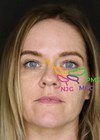
It is very helpful to use the patient’s old photographs as a guide to addressing the bothersome changes that have occurred in order to plan an approach that maintains an individual’s natural appearance. Periorbital rejuvenation should be considered in the context of: 1) bony and soft tissue volume loss, (2) tissue descent and laxity of skin, muscle, orbital septum and canthal tendons, and (3) skin ageing.
Lower eyelid blepharoplasty has a role in three types of patient. First, a patient with lower eyelid fat pad prominence from childhood, where my preferred technique is a transconjunctival-approach arcus-marginalis and orbito-malar ligament release with fat-repositioning.
The second, perhaps more common, is the slightly older patient with a combination of prominent fat pads accentuated by periobital rim hollowing, in addition to ageing features of tissue descent with laxity of skin, muscle and orbital septum. Typically, such patients request a single eyelid procedure and are usually realistic that this will not address generalised facial ageing that would require a more holistic facial aesthetic approach. For such cases, my preference is a transcutaneous-approach with orbito-malar ligament and arcus-marginalis release, Hamra-type septal-reset with composite fat-repositioning, orbicularis suspension and canthopexy.
The third represents the patient with medical preclusion to prolonged surgery, individuals on anticoagulation and those with a predominant treatable feature of skin laxity only. This may include a localised festoon (beware of risk factors for this that may cause festoon-persistence postoperatively). In such a patient, I often recommend a simple skin-pinch blepharoplasty, either sub-ciliary or direct-festoon excision, usually combined with canthopexy in view of age. A sub-ciliary skin-pinch can then be combined with hyaluronic acid filler as an office procedure to treat co-existing hollows. In some of these patients, skin laser treatment may well be an equally good alternative for skin laxity.
Transconjunctival-approach
- As the patient is usually young, recommend general anaesthesia.
- Infiltrate long-acting local with adrenaline extending to the cheek region. I usually inject 10cc to each eyelid for intumescence.
- Eye-shield is essential.
- Use a lower eyelid margin traction suture and Desmarres retractor.
- During arcus-marginalis release, be mindful of the inferior oblique muscle insertion immediately posterior to the inferior orbital rim, medially.
- Release the orbito-malar ligament from the medial tear-trough hollow, extending laterally to the lateral canthal region along the inferior orbital rim. Once the malar fat-pad is visible centro-laterally, no further dissection or release inferiorly beyond this is necessary.
- To maintain fat pads repositioned into this pre-periosteal space in the early postoperative period, I place vicryl-rapide fat-pad sutures brought through to the skin.
Transcutaneous-approach
- Stepped skin incision to preserve as much pre-tarsal orbicularis muscle (remember, undermining orbicularis oculi will partly denervate it due to its innervation from its posterior surface).
- A lower eyelid margin traction suture maintaining lower eyelid stretch allows neater pre-septal sub-orbicularis dissection as the septum is stretched to its insertion just posterior to the orbital rim. This effectively provides a runway to dissect along (“traction is the key”).
- Orbito-malar ligament release is performed in the same way as above.
- Avoid contact or incarceration of the inferior oblique muscle near its insertion immediately posterior to the inferior orbital rim, both during arcus-marginalis release but also when advancing the omentum of orbital septum and fat pad over the inferior rim.
- During a Hamra-type septal-reset, place the lower eyelid on upward stretch in order to ensure under-correction of septal tightening and repositioning that may cause eyelid retraction. The inferior septum where fat is prolapsing is usually thinned. Immediately above this is a white-line confluence or thickening of septum. This is a useful landmark to place and suture to the anterior surface of the orbital rim. Avoid suturing the orbital septum above this expansion to avoid eyelid retraction.
Skin-pinch blepharoplasty
- There are many publications describing this technique.
- In individuals who do not have hyaluronic filler present and with no history of allergy, hyaluronidase in the local anaesthetic helps skin-pinching in order to create a ‘wall’ of redundant skin to excise.
- Suture skin using a 6/0 prolene sub-cuticular continuous suture. Cover by steristrips. Patient removes steristrip and pulls out suture at home at approximately day six; In fact, I would recommend this suture technique for all blepharoplasty skin closure.
Lateral canthopexy
- This is an adjunct procedure to minimise postoperative ectropion and reduce the need for excessive skin excision (by correcting canthal-descent before planning skin excision).
- My preference is a standard trans-canthal approach using a double-armed 5/0 prolene.
- A separate exit-site skin-incision is required so that the knot may be buried sub-orbicularis at the inner rim.
- Simple steristrips to skin avoid suture-related skin-complications.
Declaration of competing interests: None declared.
COMMENTS ARE WELCOME