The incidence of skin cancer is rising exponentially in the UK; in particular non-melanoma skin cancer, yet the current statistical data surrounding exact figures is thought to be underestimated.
Topical photodynamic therapy (PDT) provides a non-invasive, safe and efficacious modality to treat certain non-melanoma skin cancers: actinic keratosis (AK), superficial and thin nodular basal cell carcinoma and squamous cell in situ (Bowen’s Disease). Prior to treatment the patient should have a clinical and histological diagnosis of the skin lesion, and this should be discussed within the skin multidisciplinary team to ensure that the treatment is appropriate for the particular lesion.
Several topical photosensitising drugs, light sources and treatment protocols are currently in use in the UK and Europe. A licensed treatment protocol, which involves narrowband red LED light at 37 J ⁄cm2 (approximately 630-nm) in conjunction with topical photosensitising pro drug Methyl aminolevulinate (MAL), which can be performed on the majority of anatomical areas and repeated as frequently as required is described. MAL is contraindicated in individuals with a peanut allergy due to the arachis oil component, those with morpheaform basal cell carcinoma, as well as porphyria.
Preparation of the lesion is pivotal in relation to the level of clearance and potential recurrence. Hyperkeratotic lesions benefit from pre-treatment with an enhanced emollient or Vaseline. Tape stripping, microdermabrasion and laser ablation are also reported methods in the literature to assist with debridement. Thin / non hyperkeratotic lesions are subjected to a gentle scrape, using either a ring curette or a 15 blade to ensure that the surface of the lesion is receptive to the application of MAL.
Once the lesion has been cleaned, a 10mm border is measured and marked around the visible margins using a skin marker pen and the MAL is applied to a thickness of 1mm, extending to the marked border. An occlusive dressing is placed over the lesion, followed by a photo protective dressing, for three hours. During this time, the pro drug MAL is preferentially taken up by neoplastic cells and converted into protoporphyrin IX (PpIX).
Three hours later, the patient returns to clinic and is placed in a comfortable position. Prior to illumination, the dressings are removed and the area is cleaned with normal saline. The lesion is assessed to establish the presence of photofluorescence using a Woods lamp, to delineate tumour margins as well as the extent of MAL uptake as porphyrins abundant in neoplastic and dysplastic cells will fluoresce pink.
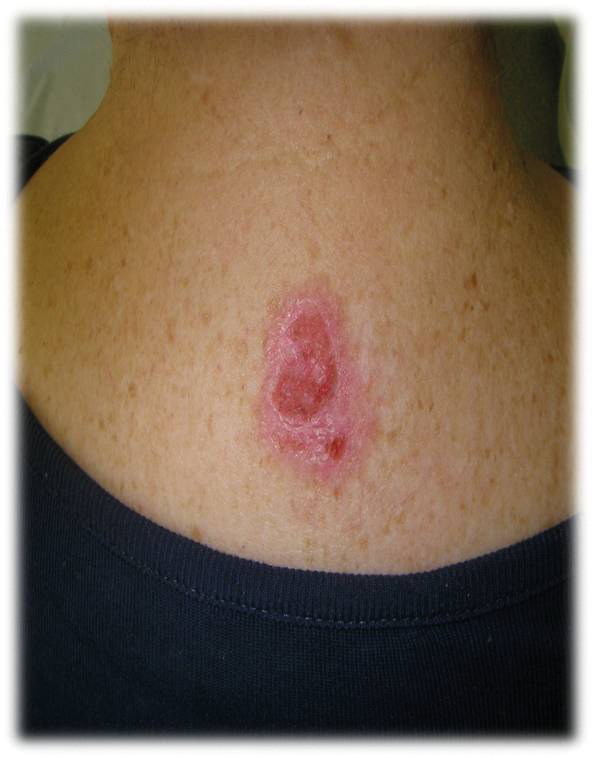
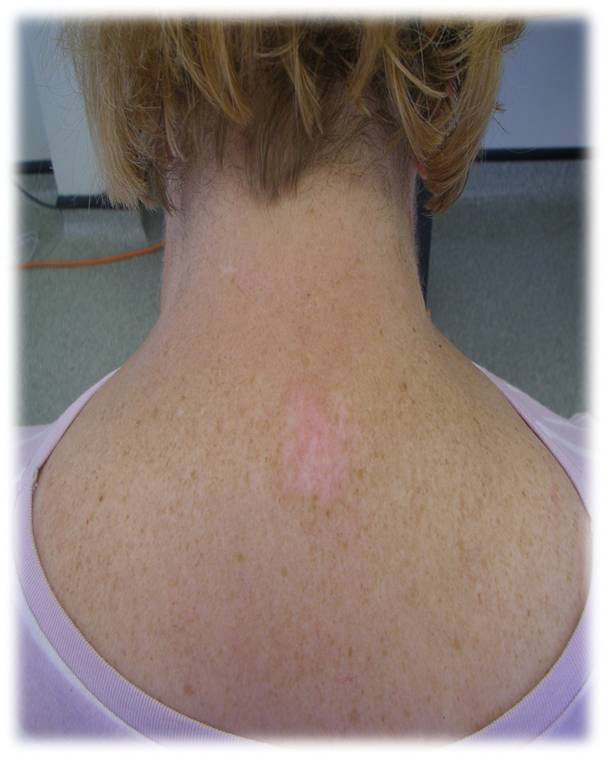
Figures show patients before and after PDT therapy for a superficial basal
cell carcinoma. Used with permission from Galderma UK Ltd.
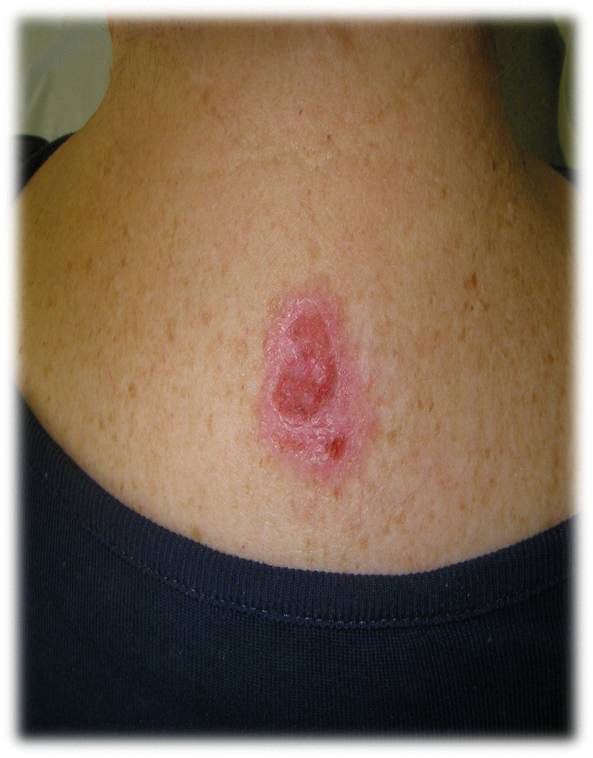
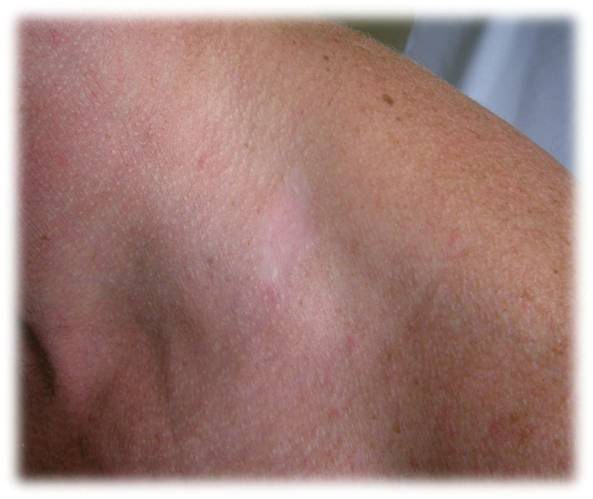
Figures show patients before and after PDT therapy for a superficial basal
cell carcinoma. Used with permission from Galderma UK Ltd.
Prior to commencing illumination, the lamp is placed at a distance of between 5-8cm from the lesion. The patient is provided with dark eye protection and the clinician wears green eye protection. When irradiated with red light, PpIX is excited to a high energy triplet state, generating reactive oxygen species free radicals which in turn can bring about cellular apoptosis and necrosis.
The extent of photofluorescence has been associated with the degree of discomfort during illumination, which generally improves with chilled sterile water sprayed on or around the treated area. Once the total light dose is delivered, a Wood’s lamp is used to check for photobleaching, which can be predictive of the extent of lesion clearance. A non-adherent dressing is placed over the lesion for 24-48 hours and the patient reviewed in three months following treatment.
In general actinic keratosis require a single treatment and superficial / nodular basal cell and Bowen’s Disease require two cycles at seven-day intervals, with the treatment protocol as above.
Where available, topical photodynamic therapy with MAL is recommended as first line therapy for Bowen’s Disease and may be favoured as a preferred treatment option when treating larger areas such as field cancerisation, as it may prevent new AKs and the transformation of AKs into invasive SCC. Photodynamic therapy can decrease expression of p53 (a marker of early skin cancer), reinforcing a preventative indication in carcinogenesis.
Declaration of competing interests: Anna Baker runs nurse-led photodynamic therapy clinics in conjunction with Ashfield Healthcare and Galderma UK.
COMMENTS ARE WELCOME









