Many patients who survive major burns, suffer a traumatic injury or undergo reconstructive surgery following cancer are left with both physical but also psychological sequelae. Sometimes early psychological difficulties improve with the passage of time with support from friends and family, however, professional psychological help is sometimes required.
The link between the physical, psychological and in particular psychosocial needs of the patient is not always integrated into the patient’s journey from the acute phase into the subsequent rehabilitative process. To integrate some of the treatment modalities, which can improve the psychosocial wellbeing of the patients, we introduced a micropigmentation and camouflage service. This is also a requirement within the medical aesthetic component of the British National Burn Care Standards [1].These Standards were devised by an expert multidisciplinary group and ensure services are working within nationally agreed service specifications and are fundamental to the provision of specialised burn care in the UK.
A micropigmentation service has been provided by our department for nine years now. It was initially set up as a combined service delivered by a senior nurse specialist and a clinical prosthetist as part of the breast reconstruction pathway. The micropigmentation was applied in the final stages of creating the new nipple areola complex.
Case study 1
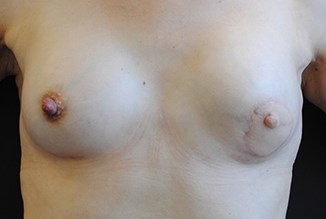
A 45-year-old lady underwent a mastectomy to the left breast with immediate lattissimus dorsi reconstruction, followed by nipple reconstruction and micropigmentation to the nipple and areola.
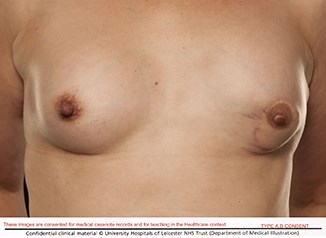
Figures 1 & 2: Pre and post nipple micropigmentation post breast reconstruction.
Case study 2
Burn scar on the face treated with skin camouflage.


Figure 5 & 6: Pre and post skin camouflage post burn injury.
With advances in techniques and experience of the practitioners, this service has evolved, incorporating a wider variety of scar management treatments, such as scar softening with micro-needling; hair simulation [2], e.g. eyebrow, beard area; separation of desired facial zones, e.g. vermillion border; and scar camouflage using semi-permanent pigments.
Micropigmentation involves implanting semi-permanent pigments into the dermal layer of the skin. It is performed using a Finishing Touches-Precision Plus, Class 2A Medical Device. Pigments are selected during the colour matching process and implanted into the skin with the hand-held device, adopting the aseptic non touch technique (ANTT). Products and pigments are sourced from Finishing Touches and Dermace. Local anaesthetic cream is only needed if there is any significant sensation in the area. This is not present when the breast reconstruction is achieved with a free tissue transfer but may be associated with tissue expanded skin and some local flaps.
A full consultation with the patient, including scar / skin assessment and medical photography is undertaken. Colours may be matched to the contralateral nipple / areola if creating the illusion of a natural appearing nipple areola following breast reconstruction, or matched to simulate the appearance of hair for the eyebrow / beard area following hair loss due to burns, for example. On average two to three treatments are required to implant the pigment and achieve the desired outcome.
To measure the value and quality of this service we sent a satisfaction survey to patients who had received nipple tattooing following breast reconstruction. We sent questionnaires to 150 patients. Of these patients, 91% underwent nipple reconstruction, while 9% opted for micropigmentation only using just colour and shading to create the 3D illusion.
All patients felt that micropigmentation following breast reconstruction was a valuable part of the treatment process, with over 90% reporting that it improved the overall appearance of their reconstructed breast. None of the patients reported having had any complications or problems with the healing process, which enabled us to reassure them that it is a safe procedure.
When asked to write comments on the procedure several common themes were apparent, with over 60% of women using one or more of the four following words: ‘Complete / Normal / Confident / Woman’.
In the words of one patient “micropigmentation has finished my cancer journey and given me a great deal of closure.”
Similarly, another patient described micropigmentation as “being the final icing on the cake on a long journey back to normality,” and finally: “my chest now feels part of me.”
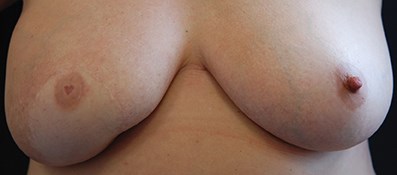
Figure 3: Areola micropigmentation different from norm.
This study confirms that areola micropigmentation is a safe and valuable part of the patient care pathway, restoring their body image, self-confidence and well-being. Interestingly, the authors received requests for alternative designs within the nipple / areola border, i.e. heart shape nipple (Figure 3). So far patients have been happy with their choice, but to be cautious these are all done with the correct pigment colour, so that should the patient change their mind at a later date the nipple areola can be completed as normal.
It has long been reported anecdotally that micropigmentation improves the aesthetic appearance of the surgically created breast [3] and our study upholds these views and additionally has an impact on the patient’s psychosocial wellbeing in terms of improved self-confidence and body image. This qualitative and quantitative data empowers us as clinicians to give patients an informed consent.
Another technique that is used to help restore colour, minimise the visual appearance of scars following trauma, burns or reconstructive surgery is with the use of skin camouflage creams or powders (Figure 4) such as Dermacolor, Veil and Kerromask. In order to use these products with success, specialist training in skin camouflage was provided by the British Red Cross. This can also play an important role in the patient’s journey in conjunction with other scar therapy interventions, such as pressure garments and topical silicone gels / sheets. Using these interventions can improve a patient’s quality of life and their ability to feel confident with social interaction.
For those with permanent or chronic disfigurement, the use of skin camouflage and micropigmentation can help a patient to adjust to an altered image and regain their self-esteem by creating a sense of personal wellbeing [4].
Tattooing is an ancient procedure, practised by humans from all parts of the world for a variety of reasons. In modern medicine it is often the valuable finishing step for a number of patients in their psychosocial rehabilitation following a long journey.
Micropigmentation and camouflage services should be integral to the patient care pathway. We have started providing these services to our local burns and plastic surgery community in the Midlands area of the UK for the last few years with positive patient outcomes.
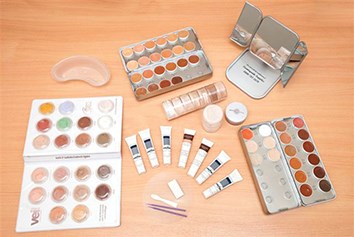
Figure 4: Colour palette for skin camouflage.
References
1. National Burn Care Standards. National Network for Burn Care.
http://www.britishburnassociation.org/
downloads/National_Burn_Care_Standards_2013.pdf
Last accessed October 2014.
2. Rassman WR, Pak JP, Kim J. Scalp micropigmentation: a useful treatment for hair loss. Facial Plast Surg Clin North Am 2013;21(3):497-503.
3. Collingridge K, Calcluth J. Micro-pigmentation: implications for patients and professionals. Br J Nurs 2005;14(15);818-22.
4. Levy LL, Emer JJ. Emotional benefit of cosmetic camouflage in the treatment of facial skin conditions: personal experience and review. Clin Cosmet Investig Dermatol 2012;5:173-82.
Declaration of competing interests: None declared.
TAKE HOME MESSAGE
-
Micropigmentation and skin camouflage should be incorporated into the patient’s rehabilitation following plastic, head and neck reconstructive surgery or following burn injuries.
-
Traditional practices such as tattooing can be adopted within the field of medicine.
-
Women feel that having their nipple / areola tattooed following breast reconstruction improves the overall appearance of their reconstruction.
-
We can improve the patient’s psychosocial wellbeing with the use of micropigmentatin and skin camouflage.
COMMENTS ARE WELCOME