Removing breast implants has a profound effect on the patient’s appearance; in this article the authors, both expert breast surgeons, discuss how to optimise the cosmetic result.
Removing breast implants has a profound effect on the patient’s appearance and we should aim to do so in a way that optimises the cosmetic result.
Breast implant augmentation remains the most commonly performed cosmetic breast procedure in the UK [1]. Whereas in the past, patients were informed that breast implants should always be routinely changed after a certain length of time, nowadays modern implants have long-term durability and satisfaction.
However, this does not completely avoid the situation where patients wish their implants to be removed, revised or exchanged, and whilst when removal is chosen, a simple breast implant explantation might leave a satisfactory result, discerning patients often ask for additional procedures to improve final aesthetic outcomes. The longer the interval since breast implantation, the more likely patients are to experience local complications and adverse outcomes, which may be cosmetically undesirable and irreversible.
In this article we will discuss the reasons for breast implant removal and the options for surgical remodelling to enhance the postoperative appearance, specifically in the case where the patient does not wish implants to be used again.
Reasons for breast implant removal
Breast implants do not always last an entire lifetime and patients should be informed at their index implant procedure that implants may need replacement and further surgery may be required. With time and natural ageing processes, breasts become ptotic (droopy) and lose volume. Changes in weight can have a profound effect on the appearance of the breasts and both pregnancy and breastfeeding might exacerbate this, with hormones leading to a cycle of breast engorgement and then later atrophy. Breast implants themselves are also subject to the effects of gravity and ‘wear and tear’ although this may be at a different rate to native tissue change. Overall, this might lead to changes such as a ‘waterfall deformity’, where remaining breast tissue droops over the front of an implant, or a ‘double-bubble’ where the implant drops down and sits below the inframammary crease, forming a separate bulge below the lower pole of the breast.
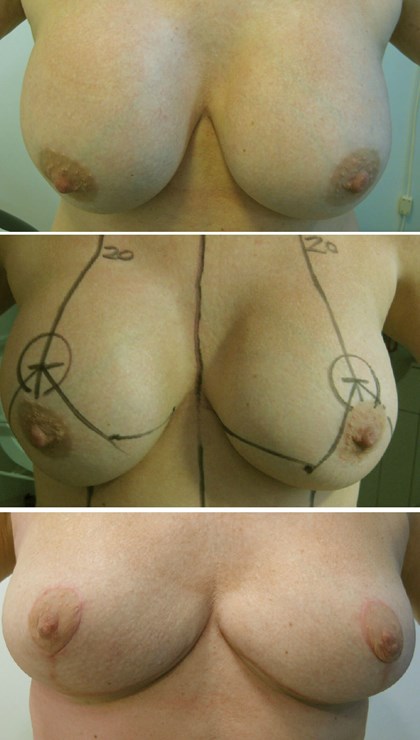
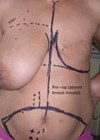
Patient underwent bilateral removal of 350cc round implants.
Second photo shows Wise-pattern markings prior to auto-augmentation at the time of implant removal.
Despite the strict quality standards that must be met by modern implants, there are well-described complications related to the prostheses themselves. Capsular contracture is the most frequent complication in breast augmentation or reconstruction with breast implants [2]. At 10 years postoperatively, between 10 and 20% of patients are found to have a degree of capsular contracture which may require further surgery [3]. Other complications include implant deflation or rupture and rotation of anatomical (teardrop) implants. In the United States, implant rupture rates range from 1.1% to 17.7% at 6 to 10 years after primary augmentation, 2.9% to 14.7% after revision augmentation, 1.5% to 35.4% after primary breast reconstruction, and 0% to 19.6% after revision reconstruction [4]. Whilst these diagnoses do not always necessitate further surgery, many patients will opt for a procedure to exchange or remove the implants.
“Auto-augmentation is using the patient’s own breast tissue to re-shape and uplift the breast”
Of recent interest, the rare diagnosis of breast implant associated adult large cell lymphoma (BIA-ALCL) always requires removal of the implant and surrounding capsule. This is most commonly diagnosed during investigation of a ‘late’ seroma, where fluid collects around the implant, after original implant placement, although other presentations do exist. BIA-ALCL is uncommon and in the UK the risk reported by the Medicines and Healthcare products Regulatory Authority (MHRA) is approximately 1:15,000 implants sold [5]. As of December 2020, the MHRA had received 83 reports of BIA-ALCL in patients with breast implants.
The most recent guidance from the MHRA states that based on the current information, people with implants do not need to have them removed in the absence of symptoms of ALCL. BIA-ALCL is not a cancer of the breast tissue itself and if caught early can be readily curable [6]. If the disease is advanced, chemotherapy or radiotherapy may be required. There has been substantial media coverage regarding this phenomenon, including BBC’s Panorama ‘The Great Implant Scandal’ in December 2018 and women are taking legal action [7].
Breast implant illness (BII) is a term used by patients who have breast implants and who may describe a variety of symptoms including (but not limited to) fatigue, chest pain, hair loss, headaches, chills, photosensitivity, chronic pain, rash, body odour, anxiety, brain fog, sleep disturbance, depression, neurologic issues and hormonal issues that they feel are directly connected to their saline or silicone, textured or smooth breast implants. The rapid surge in interest across online forums, social media and the news may be at least partially accountable for the high numbers of referrals and patients reporting of BII. BII is not a World Health Organization (WHO) recognised medical disease [8]. But a lack of a direct, proven scientific link does not mean that the symptoms experienced by these patients are not real. Some patients have legitimate concerns about a potential link between breast implants and symptoms, so it deserves our attention and further scientific research to better determine what symptoms may improve with explanation of implants [9].
Whilst we acknowledge the concerns about the risk of developing BIA-ALCL and BII (or autoimmune syndrome induced by adjuvants – ASIA) do exist, it is important to highlight that the worldwide consensus from the available evidence so far is that these potential possibilities do not justify the routine removal of breast implants at present.
Techniques to improve cosmesis after breast implant removal
When removing breast implants and not replacing them, there are several techniques that can help to address the desired cosmetic outcome. Broadly, these are a simple mastopexy with skin tightening, auto-augmentation mastopexy with relocation of breast tissue and fat transfer (lipofilling).
Breast ptosis is characterised by sagging, with the breast parenchyma drooping to the bottom of the skin envelope and thus leaving an empty upper pole, with the nipple-areolar complex shifting downwards to varying degrees. When implants are removed, a mastopexy approach can often relocate and lift the nipple position. Mastopexy scarring can be varied and tailored to the patient’s needs with circum-areolar, vertical (lollipop) or inverted-T scars.
Auto-augmentation is using the patient’s own breast tissue to re-shape and uplift the breast. Internal breast sculpturing and fixation can usually give long-lasting good outcomes. Using the Wise-pattern (keyhole) approach, this maintains the nipple on a pedicle including the superior, medial and lateral tissue around the areola but with an associated uplift. At the same time, the inferior pedicle tissue is de-epithelialised and maintained within the breast, secured and folded into the upper portion of the breast behind the nipple and in the previous location of the implant. Whilst the volume of the implant is lost from the breast, the overall shape and appearance of the breast is enhanced by relocating droopy tissue to a more youthful upper-pole position. The mastopexy, implant removal and reconstruction (MIRAR) procedure has been described by Richards [10].
Auto-augmentation combining both mastopexy and simultaneous lipofilling, as shown in a recent study of 26 patients with a mean follow-up of 18 months using a mean volume of 258cc fat, has provided a real alternative option to women who need to have their breast implants removed or desire not to continue with breast implants in secondary procedures, yet wish a more aesthetic and youthful appearance [11]. Patient satisfaction and quality of life parameters using the validated BREAST-Q questionnaire have also recently been demonstrated to show substantial improvements in patients who undergo combined auto-augmentation mastopexy and lipofilling [12]. Certainly, repeated lipofilling procedures can be carried out as part of a planned approach to breast implant removal surgery with mastopexy, giving us further options to continue to achieve a lasting result.
Conclusion
In today’s world, patients are well-informed and have high expectations for the results of aesthetic surgery. Recent media coverage of breast implant-related concerns and complications have increased public interest in the options available for breast implant removal. By using the latest available techniques, we have been able to provide patients with several options and the authors have found a high rate of patient satisfaction with the end result.
TAKE HOME MESSAGE
-
Modern breast implants are durable and do not always require replacement.
-
Concerns over breast implant related cancer and breast implant illness have driven media interest in implant removal procedures.
-
Bespoke surgery can use the patient’s own tissue to improve cosmesis.
References
1. BAAPS. Cosmetic surgery stats: number of surgeries remains stable amid calls for greater regulation of quick fix solutions. 2019
https://baaps.org.uk/about/news/1708/
cosmetic_surgery_stats_number_of_surgeries
_remains_stable_amid_calls_for_greater_regulation
_of_quick_fix_solutions/
[accessed 9 December 2021].
2. Bachour Y, Bargon CA, de Blok CJM, et al. Risk factors for developing capsular contracture in women after breast implant surgery: a systematic review of the literature. J Plast Reconstr Aesthet Surg 2018;71(9):e29-e48.
3. Lista F, Ahmad J. Evidence-based medicine: augmentation mammaplasty. Plast Reconstr Surg 2013;132(6):1684-96.
4. Hillard C, Fowler JD, Barta R, Cunningham B. Silicone breast implant rupture: a review. Gland Surg 2017;6(2):163-8.
5. Medicines and Healthcare products Regulatory Agency. Breast implants and anaplastic large cell lymphoma (ALCL) [Internet]. 2020.
https://www.gov.uk/guidance/breast-implants
-and-anaplastic-large-cell-lymphoma-alcl
[accessed 9 December 2021].
6. Marra A, Viale G, Pileri SA, et al. Breast implant-associated anaplastic large cell lymphoma: A comprehensive review. Cancer Treat Rev 2020;84:101963.
7. BBC. Women take legal action over breast implant cancer link. August 2019.
https://www.bbc.co.uk/news/health-49322370
[accessed 9 December 2021].
8. UK Government. Symptoms sometimes referred to as Breast Implant Illness [Internet]. 2020.
https://www.gov.uk/guidance/
symptoms-sometimes-referred
-to-as-breast-implant-illness
[accessed 9 December 2021].
9. Newby JM, Tang S, Faasse K, et al. Understanding breast implant illness. Aesthet Surg J 2020 [Epub ahead of print].
10. Richards A. Updates to breast augmentation. Aesthetics Journal 2019.
https://aestheticsjournal.com/feature/
updates-to-breast-augmentation
[accessed 9 December 2021].
11. Graf RM, Closs Ono MC, Pace D, et al. Breast auto-augmentation (mastopexy and lipofilling): an option for quitting breast implants. Aesthetic Plast Surg 2019;43(5):1133-41.
12. Papadopoulos S, Colpaert SDM, Goulis DG, et al. Fat grafting and auto-augmentation mastopexy after breast implant removal: technique and evaluation of outcomes using BREAST-Q. Aesthet Surg J 2021;41(6):NP388-NP401.
COMMENTS ARE WELCOME