The author interviews Dr Shobha Chamania, Chief of Choithram Hospital Burn Unit, to obtain an insight into the unique challenges burns care practitioners face in India.
Choithram Hospital Burn Unit is an Interburns accredited training centre located in Indore City, Madhya Pradesh State in Central India. The Chief of the Burn Unit is Dr Shobha Chamania, who initially started the burns services in 1985 from a humble makeshift ward of a single bed; gradually expanding the services today to a busy 14-bed Burn Unit admitting more than 220 acute burns and treating 1000 outpatients per year at Choithram Hospital. The unit also comprises a multidisciplinary team including three other burns surgeons (all plastic surgeons), a psychologist and a psychiatrist, a dietitian, physiotherapists and occupational therapists, nurses and dressing assistants.
Interburns was founded in 2006 by three surgeons – Tom Potokar (Wales, UK), Shobha Chamania (Indore, India) and Shariq Ali (Karachi, Pakistan) to balance the disparity of burns care provision in the developed countries with that of the lower-income countries by facilitating transfer of knowledge and expertise. Interburns is hence an organisation that leverages huge amounts of volunteer time from experienced medical personnel – including plastic surgeons, therapists, nurses and other specialists – to deliver high quality burns care training, education, research and capacity-building cost-effectively to middle to low-income countries. In 2008, Interburns was incorporated as a UK based charity leading to an active partnership between the Welsh Centre for Burns & Plastic Surgery and the Choithram Surgical Research Burns Centre in Indore, India which continues to this day.
In high income countries, great strides have been made in the field of burns care. To illustrate a point, one in 100,000 people die of burns injuries in high-income countries. In India and Africa, the rates are 6.4 and 6.1 deaths in 100,000 burns respectively (Source: A WHO plan for burns prevention and care. Geneva: World Health Organization; 2008). Successful burns prevention programs in high-income countries in the West have also decreased the incidence of burns significantly. We speak to Dr Shobha Chamania to obtain an insight about the unique challenges burns care practitioners face in India – how burns care in a low-income country differs from that in an advanced country and about the role of the Interburns organisation.

The author (middle) with Interburns co-founders Dr Shobha Chamania and Mr Tom Potokar
at the National Academy of Burns India Conference (NABICON) 2018.
Can you tell us about your background and what drew you to burns care as a specialty practice?
After medical school, I completed my postgraduate training in General Surgery obtaining the Master of General Surgery in 1978 at the Gandhi Medical College in Bhopal. Back then, burns were treated traditionally by conservative methods and little was known about modern treatment options. We used amniotic membranes to cover superficial burn wounds and got reasonably acceptable results.
After working for several years, I realised that burn patients were still being neglected in the country. We had no special burns care facility in the newly started Choithram hospital where I was based. Choithram Hospital was a multispeciality referral centre for the whole of central India in those days.
I initiated burns care in a room, or rather a makeshift ward, outside the main hospital building in 1985 which had no extra facilities for burns patients. In 1988, the burn unit was finally launched in the main building with just six beds, which expanded to 12 beds and now 14 beds.
How long have you been involved in the practice of burns care and can you tell us about the Interburns organisation?
I have been working in burns since 1985, never exclusively, but it remains a large focus of my practice. Initially, I was also practising paediatric and general surgery. In the latter years, I gave up paediatric surgery and continued with burns care and general surgery.
In the early days, the burn unit functioned like an isolation ward outside the main building and we had minimal staff. But surprisingly, we had some very good results salvaging patients with 60-73% Total Burns Surface Area (TBSA), even with that compromised setting and infrastructure. That motivated me and my team to focus on improving burns care further. The late Dr MH Keswani from Mumbai, pioneering burns surgeon of India, gave me guidance in setting up a proper burn unit. I later became a member of the Burns Association of India and also the International Society of Burns through his recommendations. Through these associations, many senior visiting professors came to periodically update and train us in the intricacies of total burns care and surgery. I also visited several burns centres abroad in the United States and China, taking ideas and modifying and implementing them as I went along.
Our burn unit in Choithram Hospital began a formal collaboration with Interburns UK from 2006. Interburns Director Mr Tom Potokar, a British trained plastic surgeon with subspecialty interest in burns, and myself initiated the development of a worldwide networking community committed to training burns care practitioners in low-income countries and developing strategies that are adaptable and cost-effective for burns care provision in those parts of the world. Being part of Interburns allowed us to develop a wider perspective of burns care as we travelled across several low-income countries and sought to improve burns care via formal education, research and training programs. We work in close collaboration with local partners to deliver long-term, sustainable improvements in burns care and prevention. Since 2006, we have trained over 1800 burns care professionals in Bangladesh, Ghana, India, Malawi, Nepal, Pakistan, Tanzania and Uganda to provide a good standard of burns care.
In February 2011, Choithram Hospital Burns Unit became an accredited training centre for clinical fellowship in burns care. Our aim is to offer burns care fellowships in the typical working environment and the resource level of a burn unit in a low or middle-income country. This enables us to deliver fellowships in the real life context of an operational burns unit in India and ensure that what is learnt is relevant to a practitioner who will be working in similar conditions in their own country. This fellowship is also endorsed by World Health Organization (WHO) and International Society for Burn Injuries (ISBI). Our unit started a skin bank service in February 2011 and to date, we have harvested 395 cadaver skins. We have had visiting fellows from India, Bangladesh, Nepal, Uganda, Brazil, West Bank Palestine, Afghanistan, Sri Lanka and also the UK. These fellowships are provided for surgeons, physiotherapists / occupational therapists, nurses, medical students and nutritionists. While the primary focus of the fellowship is on clinical care, our aim is for all Fellows to leave the training centre with the ability to provide a comprehensive burns care service and achieve the best outcomes for patients. In order to achieve this, burns care practitioners need to have an understanding of all aspects of burns, from primary prevention through to rehabilitation, as well as administration, fundraising and advocacy.
Staff members of the Burn Unit, Choithram Hospital headed by
Dr Shobha Chamania with visiting fellows from Uganda.
What are the particular challenges you face in burns treatment in a low-income country like India? A multitude of challenges are unique to India.
They range from poverty, ignorance, illiteracy or very low education, to oppression and exploitation of women, who are generally uneducated and economically dependent on their husbands.
Common burns are scald burns in children as cooking is often done at floor level in India in the lower income group. Kerosene flame burns are mainly in adult females. Women wearing loose flowing saris, a traditional Indian clothing, while cooking on kerosene stoves often suffer accidental burns as these saris are prone to catching fire. A more sinister cause of kerosene burns would be what we term ‘dowry burns’ which is intentional and often fatal. Bride-burning or ‘dowry burns’, accounts for the death of at least one woman every hour in India, more than 8000 women a year. In most cases, the husband’s family decide after the marriage has taken place that the original dowry was not sufficient. A dowry is paid in the form of cash and valuables to the bridegroom or his parents by the bride’s family for marriage. Dowries have been a tradition in Indian marriages as the bride’s family is expected to compensate the bridegroom and his family for the financial support the groom will have to provide throughout his wife’s life. Due to the subjugated role of women in our society, the bride’s family are often vulnerable. Demands for more money escalate into threats of violence, and when the family can’t pay any more, the harassment may rise to the extent of killing her or creating such intolerable circumstances that she decides to take her own life. Traditionally, dowry deaths (homicidal and suicidal) occur through immolation, hence the term “bride burning”. This is a very real and serious problem that often goes unreported and perpetrators go unpunished.
Burns injuries among the men are often high-tension line electrical burns. High voltage electrical accidents are common, as transmission cables and feeder cables are placed close to roof tops. People get electrical burns when they intentionally or unintentionally touch these cables. Sometimes, these transmission cables can snap and dangle, and unwary children may get pulled into the arc and suffer horrible burns. Theoretically, placing all high-tension electrical lines underground can effectively eradicate this problem but implementing it is another issue.
How does the practice of burns care in your set-up differ to that in an developed country like the UK or USA?
We don’t have an emergency room attending for burns patients in our setup. Patients come directly to the burns unit and are stabilised and treated here. There is commonly a delay between the burns incident and presentation at our unit. Pre-hospital care or on-site management of burns are often non-existent or poorly executed. We do not have specialised primary or secondary transport to an medical facility or burns centre like we see in developed countries that may even employ helicopter evacuation and transport of burns victims. Patients’ relatives have to locate a burns care provider and bring the burns victims there themselves.
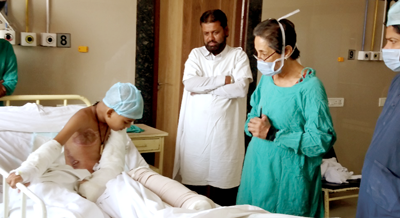
Dr Shobha Chamania during a ward round at the Burns Unit, Choithram Hospital.
Although designated as a burns unit, we do not have an intensive burns care unit. We manage all the burns patients that may require ‘intensive care’ ourselves. We don’t perform prophylactic intubation for every facial burn or in every single inhalational injury as practiced in other burns centres in the West. Patients are infrequently intubated and ventilated. This is controversial but it is our belief that unnecessary intubation may pose a risk or even prolong the clinical evolution of these patients. A large number of patients with no respiratory distress and no co-existing pulmonary pathology have been safely managed with non-invasive supportive measures. Tracheostomy is also very infrequently performed as I have often noticed that even when the burn wounds are healed, complications of the tracheostomies remain.
Early excision and grafting is generally done in one or two stages in our setting depending on the time and extent of the burns injuries.
Insurance is not very popular among the rural low-income population in India who ironically represent the majority of burns victims. Hence, the absence of third party billing and the patients’ relatives have to bear all expenses for the treatment costs of the patient.
I am sure the psychosocial and economic challenges are very different in our setting to those in Europe or the West. We have made our own low-cost substitutes for dressings and splints while not compromising outcome. Admittedly, financial challenges will render us unable to use the most advanced biological bio-engineered dressing materials and equipment.
Could you elaborate regarding the incidence of non-accidental burns in India such as ‘dowry burns’ you mentioned? What can be done to eradicate such practices?
Burns surgeons must have a high index of suspicion when assessing burns injuries to distinguish intentional injuries from unintentional ones. Management should include a psychologist and psychiatrist as part of the burns team. They should be seeing patients from the admission to the last day in the hospital, including follow-ups. Standardised tools for the assessment of psychiatric disorders and risk of abuse is mandatory.
For example, one study in India documented that 9.3% of paediatric burns injuries seen within a 15-year period were secondary to child abuse. This should be in the mind of the attending burns surgeon when assessing atypical burns injuries in the young.
As for homicidal and suicidal burns; a more accurate picture emerges if we include the cases of young married women registered as having committed suicide after dealing with harassment from her husband and relatives. As the victim is barely alive, taking a dying declaration is almost impossible. Women in rural India worry about the family and the social stigma and implications of making a complaint. Cases that occur within the premises of the husband’s house go unreported.
The Indian national burns registry states that approximately 91,000 women succumb to burns injuries annually due to ‘kitchen accidents.’ A study titled ‘Busting the Kitchen Accident Myth: Cases of burn injures in India’ by Padma Bhate Deosthal revealed that out of 22 cases of burn injuries in women examined, 15 were reported as accidental burns to the police. Ironically, when these cases were reexamined, only three of these were really actual accidents. The other cases of burn injuries were spouse inflicted, self-inflicted burns or cases of accidental burns with a history of domestic violence.
Preventing burns must start at grassroots level through active education. Public campaigns and media publicity can enlighten people on the terrible life-long outcomes of burns. We should also encourage couples and particularly women to reach out for help early on when marital discord begins. Social service providers, Non-governmental organisation (NGOs), survivor groups, public health and criminal justice practitioners can actively provide the support needed through an active multidisciplinary approach. We should also look into replacing kerosene as the primary fuel source and perhaps make the availability of kerosene safer in appropriate containers.
When burns have occurred, then timely support by the neighbours and police etc. can be implemented to ensure a quick referral to a designated burns hospital. On admission, there should be good provision of care for acute burns to save the victim and prevent contracture deformities and disabilities. This is where more burns care practitioners should be adequately and appropriately trained.
Burns care does not end with the healing of wounds and the discharge of the patient. They need to be rehabilitated and reintegrated into society. NGO groups act to interact with families and society at large to accept them back at home, include them at social events and offer them job prospects.
Education and empowering women should start with encouraging education and economic independence among female children. Stringent laws should be implemented and punishment carried out for the perpetrators of domestic violence and intentional burns. A multidisciplinary approach is necessary as this is a medical problem interwoven with crime and gender-related issues.
What are your long-term goals for the Burn Unit in Choithram Hospital?
My ultimate wish is to have a successor who has a vision to take this Burn Unit in Choithram Hospital further to achieve greater heights in burns care. If I am able to do a small amount towards the prevention of all kinds of burns, encourage team members and surgeons to do research to find their own solutions to the problems and have a cohesive passionate team dedicated to holistic burns care; then I would be happy to step down as my objective would have been fulfilled.
Lee Seng Khoo completed a fellowship in burns care at the Interburns Training Centre at Choithram Hospital under the direction of Dr Shobha Chamania in 2017.
COMMENTS ARE WELCOME










