Vascular anomalies are the most common lesions that can often lead to disfigurement of a child's appearance. Due to the complexity of diagnosis and individual specialists’ understanding of their pathological process, these young patients often undergo many unnecessary tests and waste precious time searching for the right doctor before receiving treatment.
The choice of treatment tactics depends on the child's age, the area of the haemangioma and the shape of the latter according to the International Society for the Study of Vascular Anomalies (ISSVA) classification, originally published in 2014 and updated in 2018 [1]. The total number of vascular anomalies in the world reaches 4.5%. Often these diseases are accompanied by pain, bleeding, infection, and the development of physical and mental disorders.
One of the reasons for the development of complications and ineffective treatment is the situation caused by misdiagnosis. Thus, according to Greene et al. (2011), only 53% of cases of various vascular anomalies went under the correct primary diagnosis [2]. More often than not, most of the pathology is defined by the term ‘haemangioma’ erroneously. At the same time, among infantile hemangiomas (IH), the latter was misidentified in about 17%. Although they are the most common vascular tumours of childhood.
The ISSVA classification was confirmed at the meetings of the society in 2018 and 2023 as the only and most advanced one. In recent years, there has been a clear trend towards a decrease in the frequency of surgical treatment of infantile haemangiomas of skin and mucous membranes in children. This can also be attributed to the wider use of ISSVA 2014, at least by the majority of paediatric surgeons, dermatologists, and paediatricians. A recent development is the increased use of selective laser photothermolysis for treatment of vascular tumours.
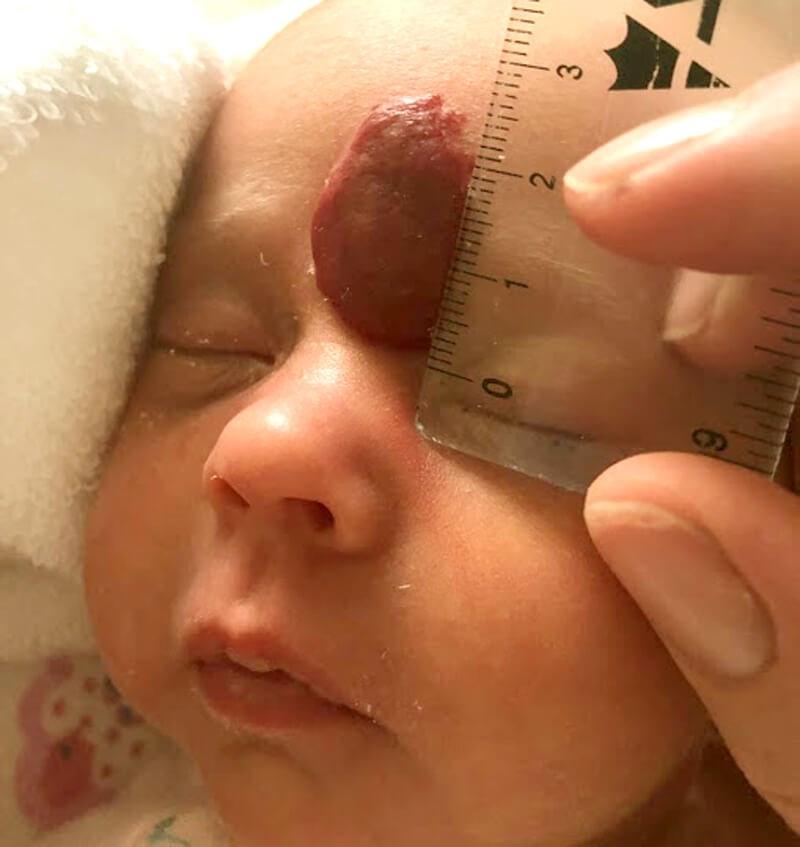
Figure 1: Haemangioma on forehead before any treatment.
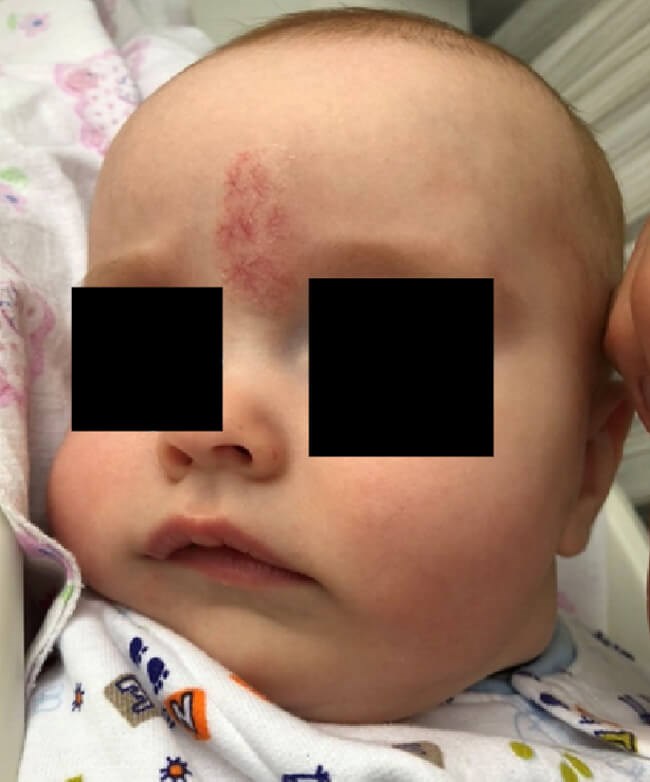
Figure 2: Haemangioma on forehead following treatment with propranolol;
it still requires aesthetic modification with a laser.
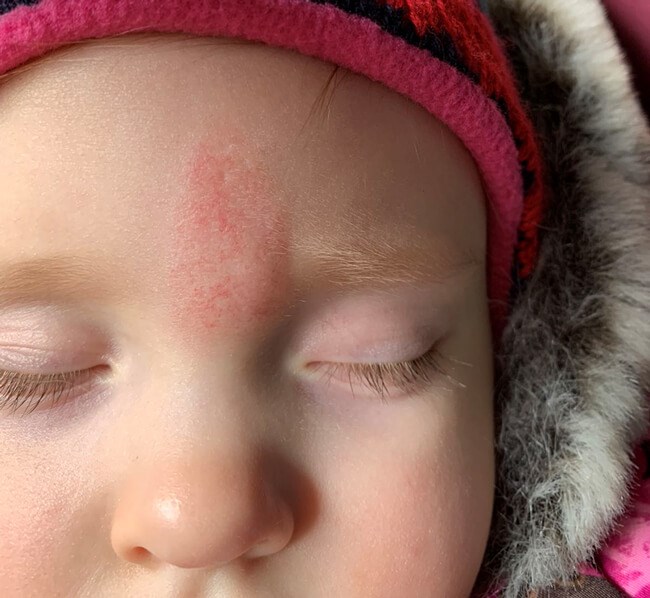
Haemangioma on forehead following completion of treatment with laser.
The use of laser technology should be the method of choice in cases of small lesions in functionally important areas or as a means of eliminating residual changes. The choice of wavelength and radiation power should be clearly defined by a specialist in each individual situation.
I conducted a retrospective analysis, which included 173 children with 213 neoplasms who were under observation and treated with a vascular laser. The main criterion for prescribing laser therapy was the location of the neoplasm in aesthetically and functionally significant areas and the small size of the vascular neoplasm. The above therapy was used as part of a comprehensive multimodal therapy in cases of treatment of residual skin phenomena in the form of telangiectasias after the use of beta-blockers or in cases of refractory haemangiomas to medical treatment. I also used the Fotona neodymium laser for preventive treatment, considering the potential risk of neoplasm spreading at the stages of evolution and recurrence after surgery.
The group of children treated with Fotona's SP Dynamis laser included 213 children with haemangiomas, two of which were segmental, and eight children had multifocal tumours. In more than half of the cases, 112 out of 213, the haemangiomas were of the so-called critical localisation. The treatment period averaged three to four procedures with an interval of five to six weeks.
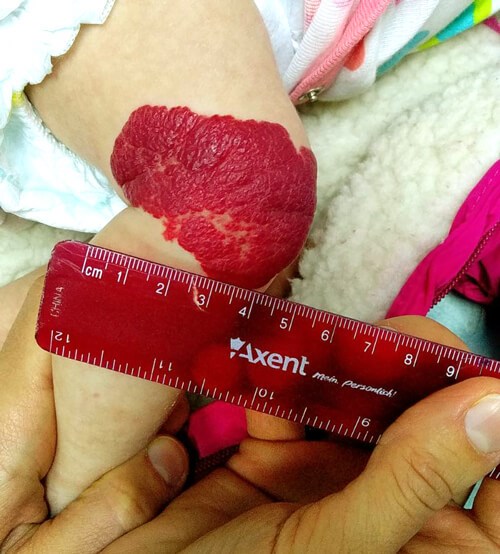
Haemangioma on knee before any treatment.
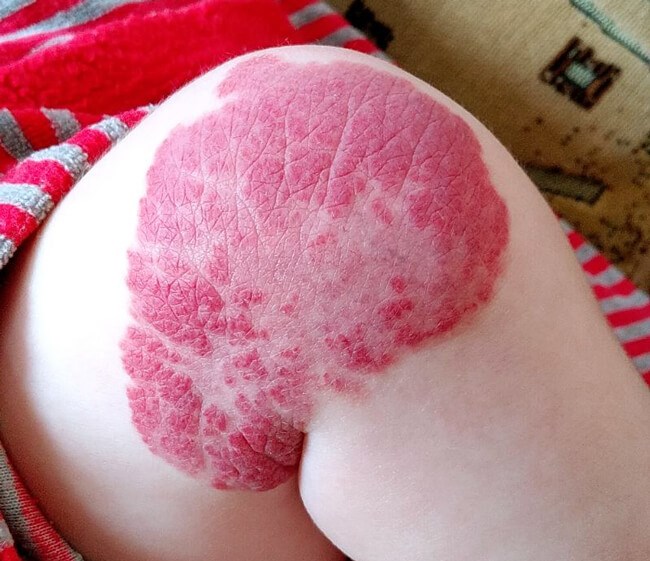
Haemangioma on knee following treatment with beta blockers.
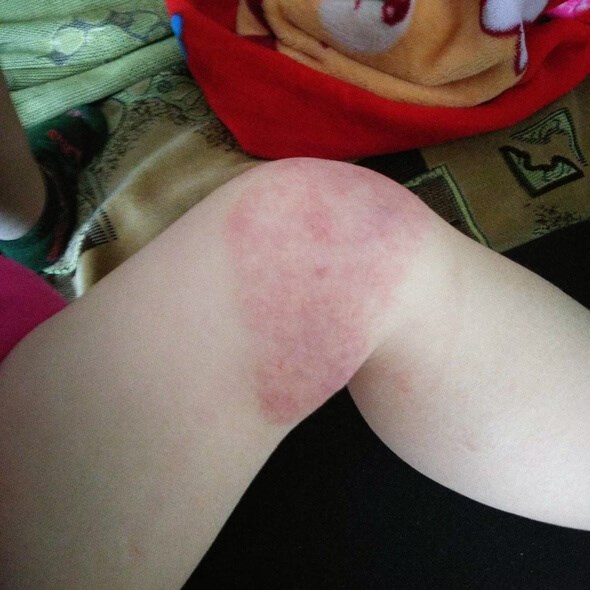
Haemangioma on knee following treatment with laser.
The treatments were performed using the R33 handpiece with an average fluence of 60J/cm2, which is much lower than the generally accepted parameters. However, the use of low power led to a significant reduction in post-laser skin complications in children.
The treatment process was usually accompanied by a slight disturbance of the child, which immediately stopped as soon as the laser irradiation was stopped, which usually lasts 1.5-2.0 minutes per session. For the first time, we used Nd:Yag laser in the microsecond range with an ultra-low fluence of 10 J/cm2. to treat the most complex segmental forms of haemangiomas. The use of such sparing parameters eliminated the formation of post-procedural complications in the form of skin scars. For two children with segmental haemangiomas of the face, a combination of methods was used to achieve the best effect, including beta-blockers and two Nd:Yag laser sessions.
The range of spots, the ability to generate powerful laser irradiation with a given wavelength of 1064nm, allows the effective elimination of a persistent focus of haemangioma proliferation in the depth of tissues up to 1.0cm with just one shot and without damaging the skin surface. This possibility surpasses the capabilities of other short-wavelength vascular lasers and complements the incomplete effectiveness of using beta-blockers as the main treatment in this case. It was the ability to use a power of 80J/cm2 at 1064nm with a working spot of 9mm that made it possible to forget about long-term propranolol intake and the tumour itself. Patients did not require post-procedural wound management or daily dressings.
Thus, the main approach to the treatment of haemangiomas, as the most common representatives of supra-superior vascular manifestations, should be an individualised, unified, customised approach, which is impossible without considering the size of the neoplasm, morphological structure, localisation, potential risk of possible complications, patient's age, concomitant malformations, and the stage of the neoplasm (proliferation or involution). In addition, the potential risks should be carefully compared with the potential benefits of treatment.
Finally, the management of such patients is simply impossible and biased if the team of doctors or the attending physician does not have experience with the Nd:Yag laser. The results with this laser, its ease and simplicity of use are impressive and exceed the expectations of both doctors and patients' relatives.
References
1. ISSVA Classification. 2018.
https://www.issva.org/classification
[accessed 25 October 2023].
2. Greene AK, Liu AS, Mulliken JB, et al. Vascular anomalies in 5,621 patients: guidelines for referral. J Pediatr Surg 2011;46(9):1784-9.
Declaration of competing interests: None declared.
COMMENTS ARE WELCOME