For thousands of years chemical peels have been used for ameliorating the signs of photoageing, reducing scarring and skin lightening. The term ‘chemical peel’ is both loose and frightening to consumers. Some patients only think of the images they see on TV portraying full face phenol peels performed under general anaesthetic, others will think of the peels available on the high street which are really merely gentle exfoliation. In this article I will outline the types of peel available, and touch on practical applications of peeling.
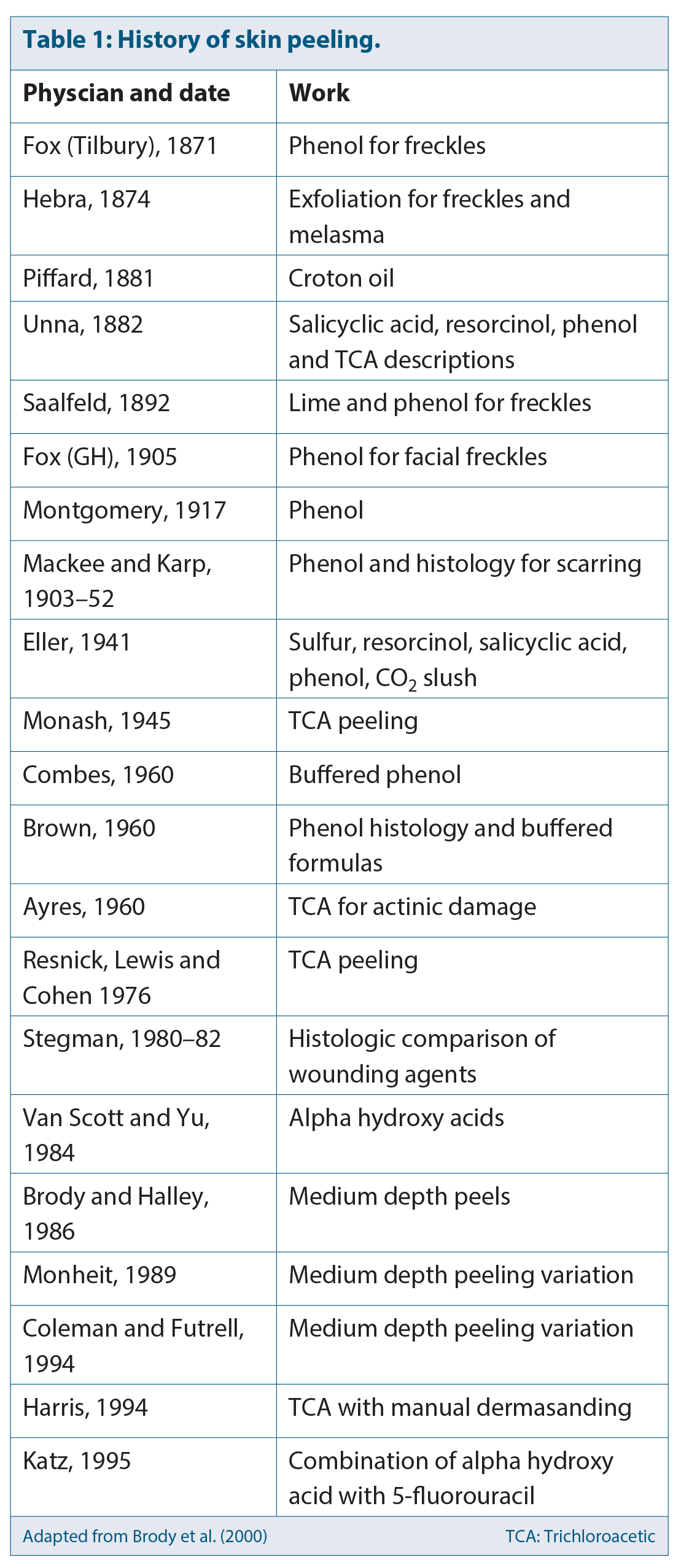
There was a flurry of clinical research and interest in phenol in the late 1940s, and trichloroacetic acid (TCA) in the 1960s, but it was not until the late 1970s and 1980s that chemical peeling regained popularity. During this time, Resnik et al. [1] published articles on the benefits of TCA and Van Scott and Yu published papers on alpha hydroxy acids (AHAs) (Table 1 [2]).
We currently have multiple options of both single ingredient and combined peels to choose from: superficial epidermal peels remove layers of the skin through keratocoagulation or keratolysis leading to desquamation and enhanced epidermal renewal; medium depth (papillary dermis) and deep (reticular dermis) cause second degree burns.
Superficial peels
AHAs have two main actions in terms of their peeling effect, reducing corneocyte cohesion and breaking the desmosomal attachments between corneocytes [3]. However, they have also been shown to increase skin thickness. For example, Ditre et al. showed a 25% increase in dermal thickness accompanied by increased hyaluronic acid, enhanced collagen density and improvements to elastin [4]. This is unique to AHAs such as glycolic acid, and may offer significant benefits in terms of improved patient outcomes over peels that simply work by removing the top skin layers [5].
There are many other superficial peel agents such as resorcinol, vitamin A formulations, and frequently these are used in combination peels both with and without one or more AHAs.
Medium peels
TCA is the most widely reported medium depth peel, and can be used for full face peels or locally for hypertrophic actinic keratosis and sebhorreic keratosis. There was a resurgence in popularity of the use of TCA in the 1960s [6] and today it is widely used both as a standalone peel and in combination with other peeling agents and treatment modalities.
Deep peels
Phenol and phenol-based combination peels have been written about over the past 200 years since they were first described by Charles Frederick Gerhardt in 1841 working on carbolic acid [7]. In the 1940s and 1950s, non-medical practitioner use of peels leading to newsworthy horror stories caused them to be rejected by the medical fraternity [8]. More recent work by Deprez in Spain, Vigneron in Fance and Figureido in Portugal, among others, showing inflammatory actions leading to new collagen and ground substance in the dermis, has brought them back to selected use in clinic.
Practical tips for peeling
- Preparation is key. Some peels require preparation at home with the same ingredient such as glycolic acid to ensure no sensitivity. However, preparing the skin is also to ensure an even application – oil will reduce penetration, dry areas will absorb faster; even penetration is critical. This is brand specific.
- Understand the brand. There are significant variations between manufacturers in terms of potency. Understand each manufacturer’s language – for example % and pH can vary widely, it is important to understand the critical parameter for success with the agent you are to use, a glycolic acid 20% with a pH of 1.6 will be significantly more effective than a 50% glycolic peel at pH3.
- Patient selection. Not only choosing the correct peel for the indication, but ensuring the patient is prepared for the post treatment period. A patient wanting a fast result and not minding downtime will not be happy with a course of peels leading to long-term skin health. A patient wanting a slow progression will not be happy with a one-off deep peel.
- Communication. It is vital that the peel patient understands pre and post treatment homecare protocols for the specific peel proposed. Be clear about post treatment downtime, and possible discomfort, peeling, scarring potential, further treatment, etc.
- Protection. Do not peel a patient who cannot demonstrate understanding of SPF. I will not peel a patient unless they either purchase SPF from the clinic or bring their own SPF in at the time of peeling.
Successfully incorporating peels into your practice can increase patient satisfaction with other procedures, combining peels with homecare provides a service to your patients, without which they will seek other ‘skincare professionals’ advice – after all 94% of consumers will buy skincare from somewhere [9].
References
1. Resnik SS, Lewis LA, Cohen BH. TCA peeling. Cutis 1976;17:127-9.
2. Brody HJ, Monheit GD, Resnik SS, Alt TH. A history of chemical peeling. Dermatol Surg 2000;26(5):405-9.
3. Van Scott EJ, Yu RJ. Actions of alpha hydroxy acids on skincompartments. J Geriat Dermatol 1995;3(Suppl A):19-24.
4. Ditre CM, Griffin TD, Murphy GF. Effects of alpha-hydroxy acids on photoaged skin: a pilot clinical histologic and ultrastructural study. J Am Acad Dermatol 1996;34(2Pt1):187-95.
5. Bowes L. The science of hydroxy acids: mechanisms of action, types and cosmetic applications. Journal of Aesthetic Nursing 2013;2(2):77-81.
6. Ayres S 3rd. Superficial chemosurgery in treating ageing skin. Arch Dermatol 1962;85:385-93.
7. Landau M. Advances in deep chemical peels. Dermatol Nurs 2005;17(6):438-41.
8. Landau M. Deep chemical peels (phenol). In: Tosti A, Grimes P, De Padova M. Colour Atlas of Chemical Peels. 2nd Edition. Springer-Verlag. Berlin; 2012.
9. UK salons fight the signs of ageing with high tech facials. MINTEL.
http://www.mintel.com/blog/beauty
-market-news/uk-salons-fight-the
-signs-of-ageing-with-high-tech-facials
Last accessed July 2015.
COMMENTS ARE WELCOME