Wound healing takes place by two distinct mechanisms. The first involves cellular proliferation and migration resulting in regeneration. This occurs in the epidermis and leaves no scarring. The dermis is a collagen-rich connective tissue and when this is damaged the process of healing follows a distinct pattern with initial inflammation and removal of contaminated or damaged material and then a rapid deposition of new collagen.
This new collagen is not placed in the orderly manner of the uninjured dermis, and it is this lack of organisation which determines a scar. A normal scar will go through an initial phase of hypervascularisation and proliferation followed by a period of stabilisation and then progressive remodelling. The original tissue architecture is however never achieved, and scarring can be permanent. Scarring can be both aesthetically and functionally limiting. As such scars have long been a focus of treatment with many different modalities explored. In this paper we describe our clinical experience of a new form of laser treatment.
Ablative fractional lasers have proven effective after a variable number of sessions. Micro-epidermal wounding also offers the ability to increase trans-epidermal delivery of selected drugs. Lighter photo-genetic skin types can be addressed more safely than darker skin. Repetitive, controlled micro-wounding actions on scar tissues induce a sort of biological ‘rewind’ of wound healing, leading to an optimisation of tissue repair processes.
The latest generation of 1064nm Q-S nano- and pico-second pulse lasers can operate in full or fractional beam mode. Here we introduce the Fotona Starwalker MaQX. Due to its high energy, hybrid pico / nano pulse, it can drill precise micro-holes through skin tissues. The hybrid delivery involves a train of 580ps bursts operating within 4ns intervals. This action relies on extremely confined micro-pressure waves generating minimal collateral photo-thermal damage. The device is able to produce short 1.6ms pulses that can be used to reduce the vascular component associated with active proliferation of fibrotic tissue in hypertrophic and keloid scars. It also appears to photo-thermally prime dermal fibroblasts in hypotrophic scars subject to modulating fluence and number of passes. This innovative form of ablative fractional remodelling is showing extremely promising clinical results.
Treatment protocol
Frac-scar consists of a sequential combination of short 1.6ms 6mm-spot photo-thermal tissue priming followed by 5mm x 5mm QS hybrid nano / pico pulse micro-fractional photo-acoustic ablation MaQx 5-10 followed by 20% triamcinolone acetonide under occlusion.
Patient selection
Treatment can be safely performed on all Fitzpatrick skin types. Darker skin requires gentler parameters and fewer passes. Contraindications include active skin infection, malignant skin tumours, auto-immune skin disorders, skin allergy to triamcinolone acetonide and, most importantly, unrealistic expectations.
Preparation
After photographic documentation, skin antisepsis is performed with 10% sodium hypochlorite and topical anaesthesia (Benzocaine 20% / Lidocaine 10% / Tetracaine 10% liposome gel) applied under occlusion for 30-45 minutes.
Laser procedure
Step 1
Starwalker MaQX 1064nm – collimated R28d full beam handpiece – 1.6ms Frac-3 mode with 6mm spot size 10J/cm2 3Hz three passes (keloid and hypertrophic scars) – four-five passes (hypotrophic scars) delivered with slow painting technique. Clinical endpoint: mild erythema with minimal tissue swelling.
Step 2
Starwalker MaQX 1064nm – fractional 5mm x 5mm FS20Bd handpiece – MaQX 5 144mJ/px 1.5Hz (hypotrophic scars) – fractional 5mm x 5mm FS20Bd handpiece – MaQX10 267mJ/px 1 Hz (hypertrophic and keloid scars). One to two passes are performed on all scar tissues. Clinical endpoint: pinpoint capillary bleeding.
Step 3
0.9% N/S soaked sterile chilled (4°C) surgical gauze (contact time five minutes) to stop capillary bleeding. Gentle tissue cleansing with sterile gauze followed by application of sterile alginate compresses. Twenty percent triamcinolone solution gently and uniformly distributed on alginate compresses. Polyurethane film occlusive dressing.
Post-treatment skincare
Occlusive dressing is removed after three hours. Treated area is cleansed with 1.5% H2O2 solution and sterile surgical gauze. Topical moisturiser is applied twice a day for 21-30 days. 0.05% clobetasol ointment is applied twice a day for two / three consecutive days per week for 21-30 days. Patients are advised on possible cutaneous reactions such as erythema, moderate swelling, minimal burning and itching, usually more evident on the second post-treatment day. Minute pinpoint brown scabbing will be noted. They progressively fade in seven to ten days.
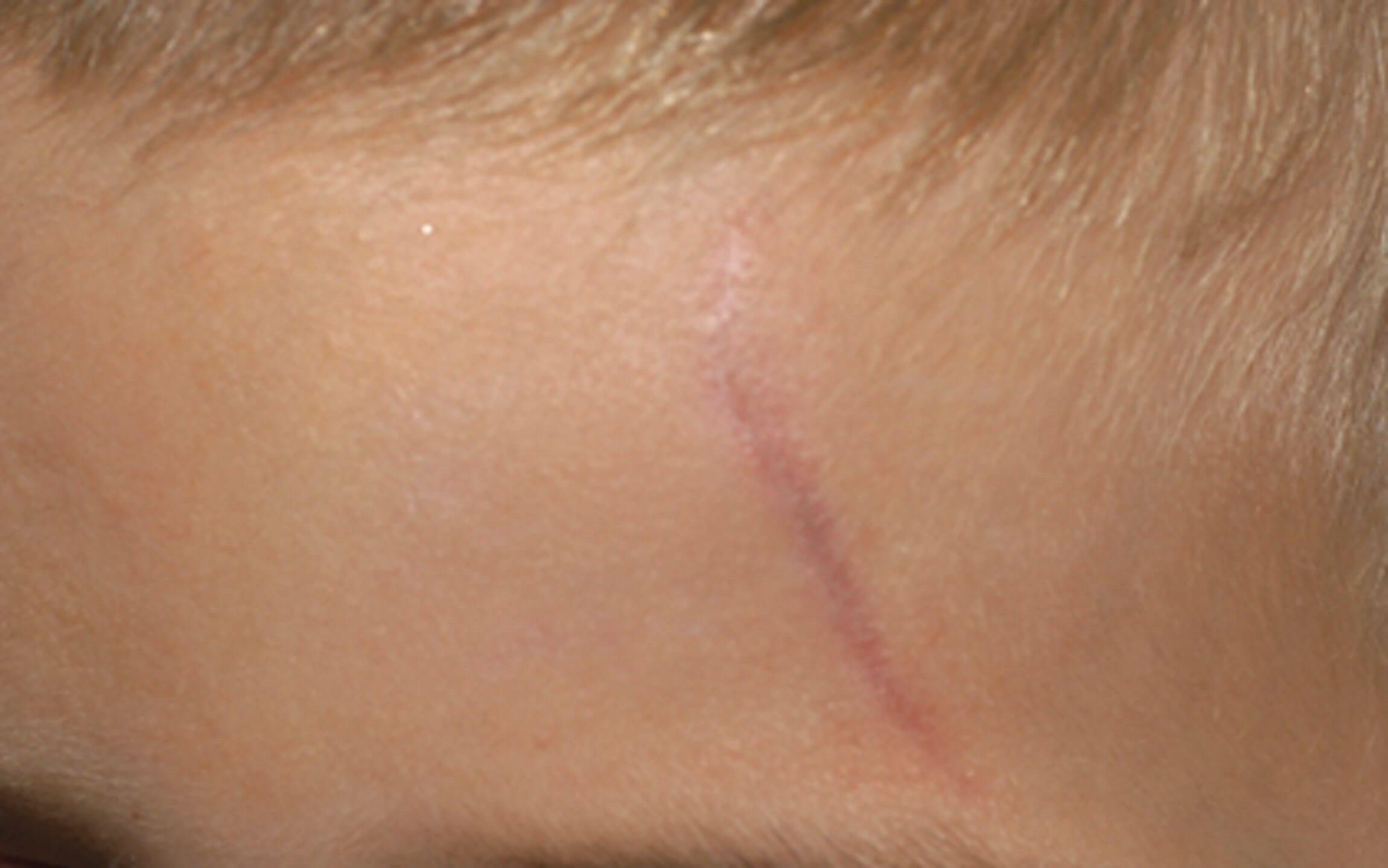
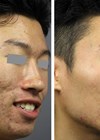
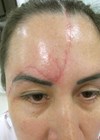
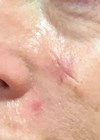
Figure 1a.
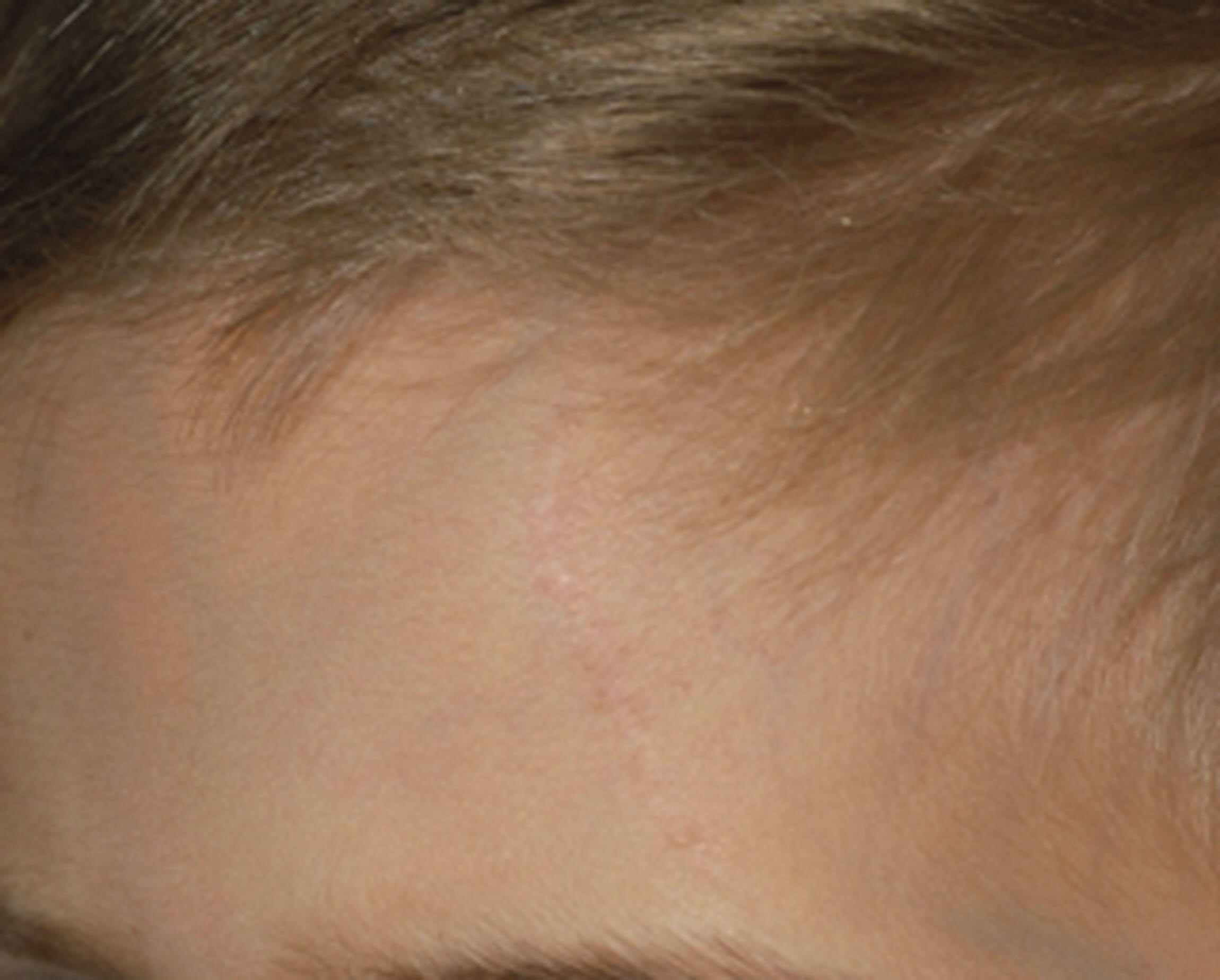
Figure 1b.
Clinical outcome
Structural improvement will be observed after 21-30 days (Figure 1a and b). Significant variations will be evident according to anatomical location, age of scars, and if the scar has been previously treated. Lower body areas will heal slower and clinical improvement will take longer. Treatment should be repeated four to six times at four to six-week intervals.
Declaration of competing interests: Leonardo Marini is an Expert Clinical Lecturer for LAHA Laser and Health Academy. He has received honoraria to speak at LAHA events as well as for conducting online and on-site Fotona clinical workshops worldwide.
COMMENTS ARE WELCOME