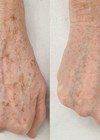
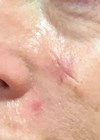
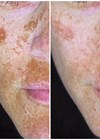
The development of laser-based aesthetic devices has provided patients with an appealing non-surgical treatment alternative to address clinical aspects of photoageing skin [1]. Many treatments include skin resurfacing of the uppermost skin layers to initiate a skin regeneration process with fewer risks and complications and with a faster recovery time than conventional invasive procedures [1].
The Frax 1940 non-ablative solid-state diode laser handpiece, developed for the Nordlys™ and the Frax Pro™ multi-application systems, is intended to be used for coagulation of soft tissue.
Treatment of the skin using the Frax 1940 handpiece leads to skin resurfacing via ablation and coagulation of soft tissue. The handpiece is equipped with a replaceable roller tip and motion sensor, controlling the rate at which the laser delivers the microscopic treatment zones (MTZ) arrays to the skin, as determined by the speed at which the user advances the roller across the targeted area. The treating operator has control over the scan width, energy per MTZ, and percent of coverage, while the system independently calculates the number of MTZs / scan width and the number of passes. As a safety feature to prevent multiple MTZ arrays being overlaid, the laser can only deliver energy while the roller is in motion. A low power <1mW red aiming beam at 650nm helps to show the user where the treatment laser pulses will be delivered. An integrated cold air delivery system provides patient comfort.
During the second phase of an IRB-approved clinical trial, 18 female patients underwent a series of two to three skin resurfacing treatments to photoaged skin with the Frax 1940 handpiece at the Candela clinic.
Procedure
Prior to full resurfacing treatment, several test spots were performed on other anatomical locations. Test spots were monitored for up to 28±7 days to evaluate treatment parameters for patient safety.
Topical anaesthetic cream was generally applied prior to treatment using a lidocaine 23% / tetracaine 7% compound, EMLA™ (lidocaine / prilocaine) or benzocaine / lidocaine / tetracaine (BLT). Full treatment parameters were set according to physician discretion taking into consideration: test spot outcome, location of treatment, skin type and clinical indication. In general, the scan width was decreased, and the coverage increased to 30-40% when focusing on areas with discrete lesions. Treatment complications were minimal, and discomfort associated with the treatment was generally mild to moderate.
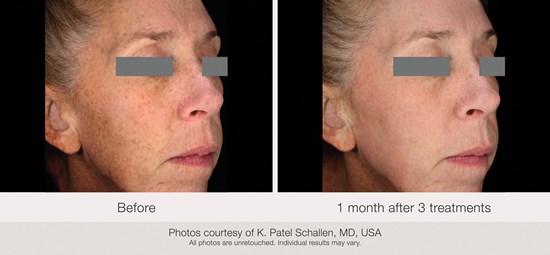
Figure 1: (L-R) Before and one month after three treatments.
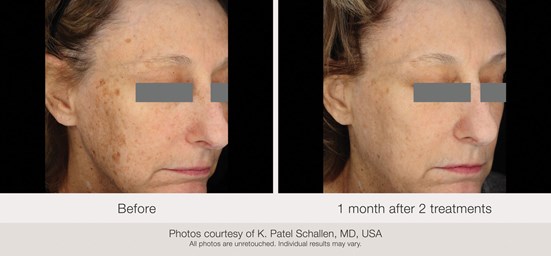
Figure 2: (L-R) Before and one month after two treatments.
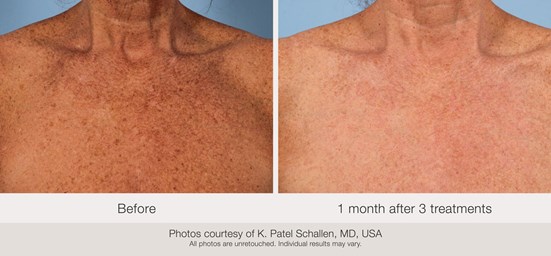
Figure 3: (L-R) Before and one month after three treatments.
Results
Clinical photography was performed for a blinded assessment evaluation at the final follow-up. Subjects were to report on satisfaction and Global Aesthetic Improvement Score (GAIS) at the one-month and three-month follow-up visits. Two subjects dropped from the study prior to the third treatment. At the one-month follow-up, a total of 20 assessments (15 for full face, four for chest and one for hands) were reported for the 16 subjects. All subjects reported satisfaction with their treatment outcome with 50% (10/20) of assessments reported as ‘Very satisfied’. Most assessments (90%, 18/20) indicated improvement with 65% (13/20) of the GAIS assessments showing marked improvement to optimal cosmetic result (‘Very much improved’). Due to clinic closure during the COVID-19 pandemic, three-month follow-up data is available for only four of the treated subjects.
Visible reduction in pigmentation associated with photoaged skin was observed at the one-month follow-up (Figures 1-3), but varied by severity at baseline and treatment location. For example, some subjects showed better clinical outcomes after treatments to the face than to the chest.
Discussion
In this study, clinical photography demonstrated visible improvement following two or three treatments with the Frax 1940 handpiece. In clinical practice, if patients presenting with photoaged skin have visible linear telangiectasias or diffuse redness at baseline, then the vascular dyschromia can be addressed after a series of skin resurfacing treatments.
Intense pulsed light (IPL) treatment, using the SWT® handpieces available with the Nordlys system, demonstrated significant improvement in diffuse redness and linear telangiectasias in a previous clinical study [2]. The IPL treatment should be performed after the micro-epidermal necrotic debris from the skin resurfacing procedure has cleared (two to three weeks).
References
1. Angelo-Khattar M. Non-ablative lasers for photorejuvenation. In: Issa M, Tamura B (Eds). Lasers, Lights and Other Technologies. Clinical Approaches and Procedures in Cosmetic Dermatology. Cham, Switzerland; Springer; 2018.
2. Schallen KP, Murphy M. Treatment of photodamaged skin with a combined dual-filter intense pulsed light and fractional 1550-nm laser system. Lasers Surg Med Suppl (ASLMS 2020 40th Annual Conference).
Declaration of competing interests: Konika Patel Schallen is Medical Director of Candela Corporation. Meghan Murphy is an independent consultant at the Candela Institute for Excellence. Nicolle Dest and Raylene Piretti are employed at the Candela Institute for Excellence.
Acknowledgement: All photos courtesy of Konika Patel Schallen. All photos are unretouched. Individual results may vary.
COMMENTS ARE WELCOME