How I Do It
How I Do It - A novel method obviating the need to proceed to second stage autologous skin grafting in selected burned patients resurfaced with Integra™
A survivor of large full thickness skin burns will have suffered for months during repeated grafting surgeries to heal, yet real recovery will take years, if at all, because of the inevitable physical and mental challenges. Time spent on the...
How I Do It - Optimising lymphatic recovery following abdominoplasty: The role of advanced postoperative MLD
As abdominoplasty procedures increasingly combine rectus plication and liposuction, patient recovery relies on more than wound care alone. For surgeons and recovery specialists alike, understanding how lymphatic function supports optimal healing is essential. Integrating advanced manual lymphatic drainage (MLD) within...
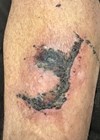
HOW I DO IT - Er:YAG laser ablation for enhanced lesion removal
Ablative lasers, such as CO2 and Er:YAG, may be regarded as superior to traditional surgical techniques – elliptical excision, curettage, cautery and cryotherapy – because they provide greater precision and uniformity in lesion removal. This enhanced accuracy translates into improved...
How I Do It - Hybrid cooperative complexes and monopolar radiofrequency: A combined regenerative approach for skin harmonisation (CRASH technique)
Preventing facial sagging has become a central goal for both aesthetic practitioners and patients. A deeper understanding of the soft tissue ageing process has highlighted the key role of facial subcutaneous white adipose tissue. Properties of the overlying skin –...
How I Do It - Using 3D imaging technology in aesthetic medicine
In recent years, there has been a shift in how patients see themselves. The ‘selfie generation’ are constantly exposed to idealised images, which means that many patients are hyper-aware of subtle facial asymmetries and textural irregularities. They no longer look...
How I Do It - Buried integra in the management of temporal cavernous haemangioma
Cavernous haemangiomas are rare, often distressing, and visually conspicuous vascular abnormalities caused by a mass of aberrant tangles of thin walled, easily distended blood vessels. Fourteen percent will present in the head and neck regions and are histologically characterised by...
How I Do It - Nd:YAG Laser for erasing periocular veins
Periocular veins are superficial blood vessels located around the eyes, often visible beneath the thin skin of the lower eyelids, temples, and sometimes above the eyes. These veins typically begin at the bridge of the nose and extend outward, joining...
How I Do It - Hyperdilute CaHA for the ageing neck
Calcium hydroxylapatite (CaHA) has demonstrated strong biostimulatory effects; increasing collagen and elastin production, while promoting angiogenesis and proteoglycan formation [1]. Consequently, its application as a valuable aesthetic intervention for age-related skin changes is being increasingly adopted. At particular dilutions (when...
How I Do It - Healing difficult wounds non-surgically with focused extracorporeal shockwave therapy
A pre-tibial laceration is a common and serious wound, particularly in the elderly where co-morbidity from smoking, peripheral vascular disease, diabetes, malnutrition and tissue-paper-thin skin are major influencers of outcome. Degloving injuries may be seen as preterminal events in the...
How I Do It - Sebum, science, and the 1726nm laser: Rethinking acne management in a post-antibiotic era
Acne vulgaris remains one of the most prevalent skin conditions worldwide, affecting up to 85% of adolescents and persisting into adulthood for a significant proportion of individuals. Conventional therapies – topical retinoids, oral antibiotics, hormonal agents, and isotretinoin – remain...
How I Do It - 3D imaging in anti-ageing consultations
As aesthetic practitioners, one of the most powerful tools we can employ for effective anti-ageing consultations is clear visual communication. So, I’ve trialled countless technologies to find a device that brings the nuances of a patient’s face to life. Aura’s...
How I Do It - Auricular reconstruction: Helical advancement flap
As the incidence of cutaneous malignancy increases further due to both the ageing population and greater disease awareness, the demand for surgical resection within the high-risk regions of the face, including the pinna, is rising [1,2]. Approximately 50% of all...