The operation called hymenoplasty is requested by women all over the world before marriage if they have engaged in premarital sex. They think that by undertaking the procedure of hymenoplasty they will regain their lost virginity, a theory that is widely accepted by patients and medical professionals. We believe however that hymenoplasty restores the torn hymen but does not regain ‘lost virginity’. Instead, the procedure of revirgination is undertaken to restore all changes in the genitalia which occur following recurrent intercourse, including hymen restoration by hymenoplasty, correction of looseness of the vaginal vault by vaginoplasty, and correction of labial flare by bulbospongioplasty.
Introduction
As previously stated hymenoplasty is the procedure to restore the torn hymen. The typical patient is an unmarried woman who has experienced premarital sex and is soon going to be married. However, most patients are not aware of the difference between hymenoplasty and revirgination. After undertaking hymenoplasty in many patients over many years, we have now realised that most patients actually require revirgination surgery and not hymenoplasty.
The academic literature is devoid of details about hymenoplasty procedures. We have found one report of the procedure but the description is limited and there are no photographs [1]. There is also a paucity in the literature of information about the procedures involved in revirgination, and, in a few cases, hymenoplasty and revirgination have been described as similar if not synonymous. From our considerable clinical experience of female genital surgery we have identified a few changes which occur following repeated sex and revirgination should mean the reversal of all such changes. Hymeneal rupture is obviously one such change, but vaginal looseness is another and flaring of labia majora due to disruption of fibres of the bulbospongiosus from the perineal body also occurs.
We have described a procedure for hymenoplasty by using the remnants of torn hymen [2]. However, revirgination is a more complex procedure.
“Hymenoplasty and revirgination are not the same, and there is a need to change this perception in both patients and medical professionals.”
The patients
We have performed revirgination surgery in 56 women over a period of three years. All were unmarried women who requested tightening of the relaxed vagina and hymenoplasty at the same time. None of the patients were aware of the difference between the two procedures, all believing that hymenoplasty is tightening of vagina. Thirty females were accompanied by their parents, five were accompanied by their boyfriends or fiancée, while the remaining patients were unaccompanied. Patient history was taken and all patients were informed that the absence of hymen alone is not a sign of lost virginity, and that the same is true for post-coital bleeding on the first post-nuptial intercourse. All of the patients agreed to undergo revirgination surgery, consisting of hymenoplasty, tightening of the vagina and bulbospongioplasty to correct flare of the labia. No patients requested just the simple hymenoplasty procedure.
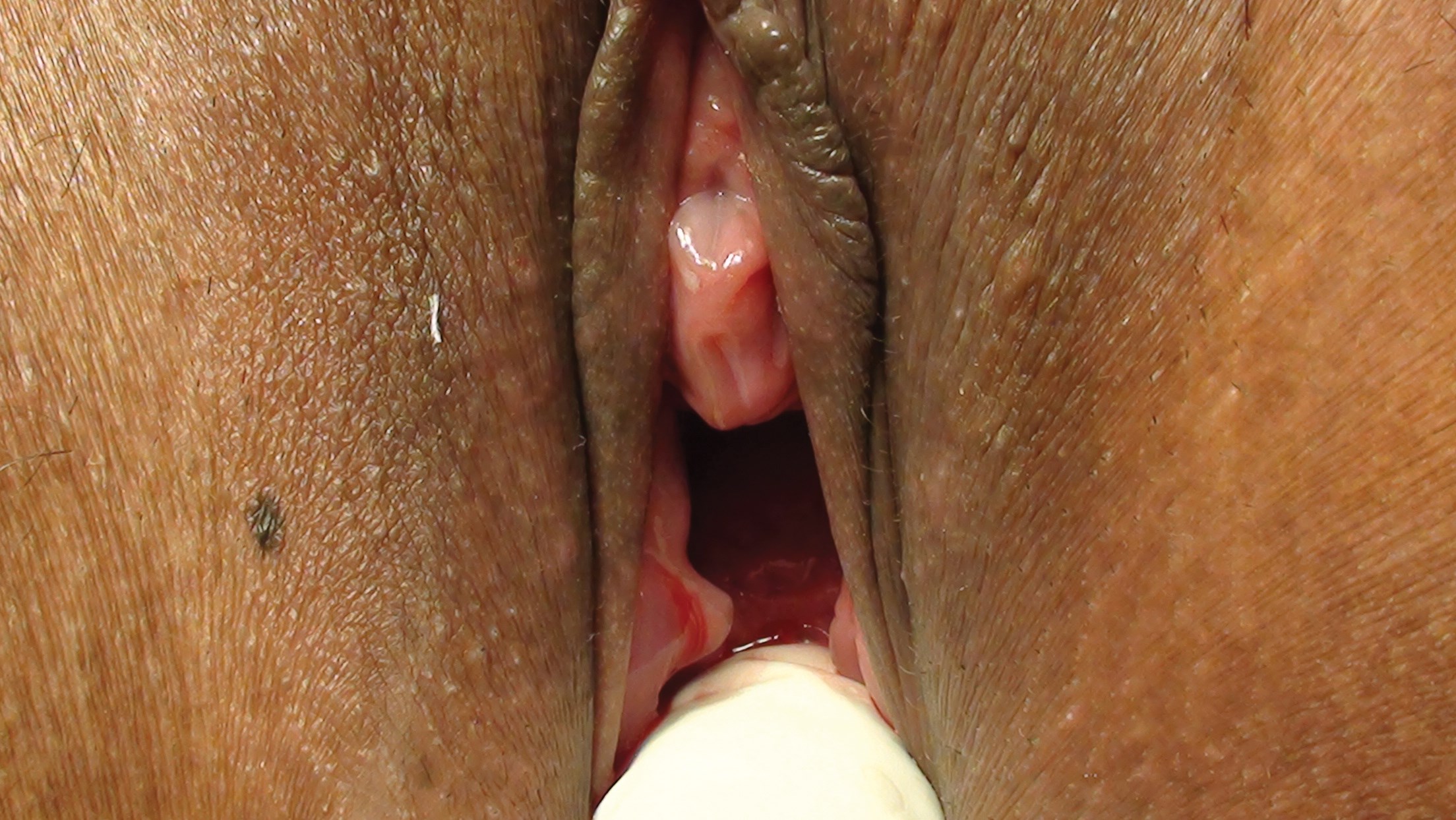
Figure 1: Showing torn pieces of hymen.
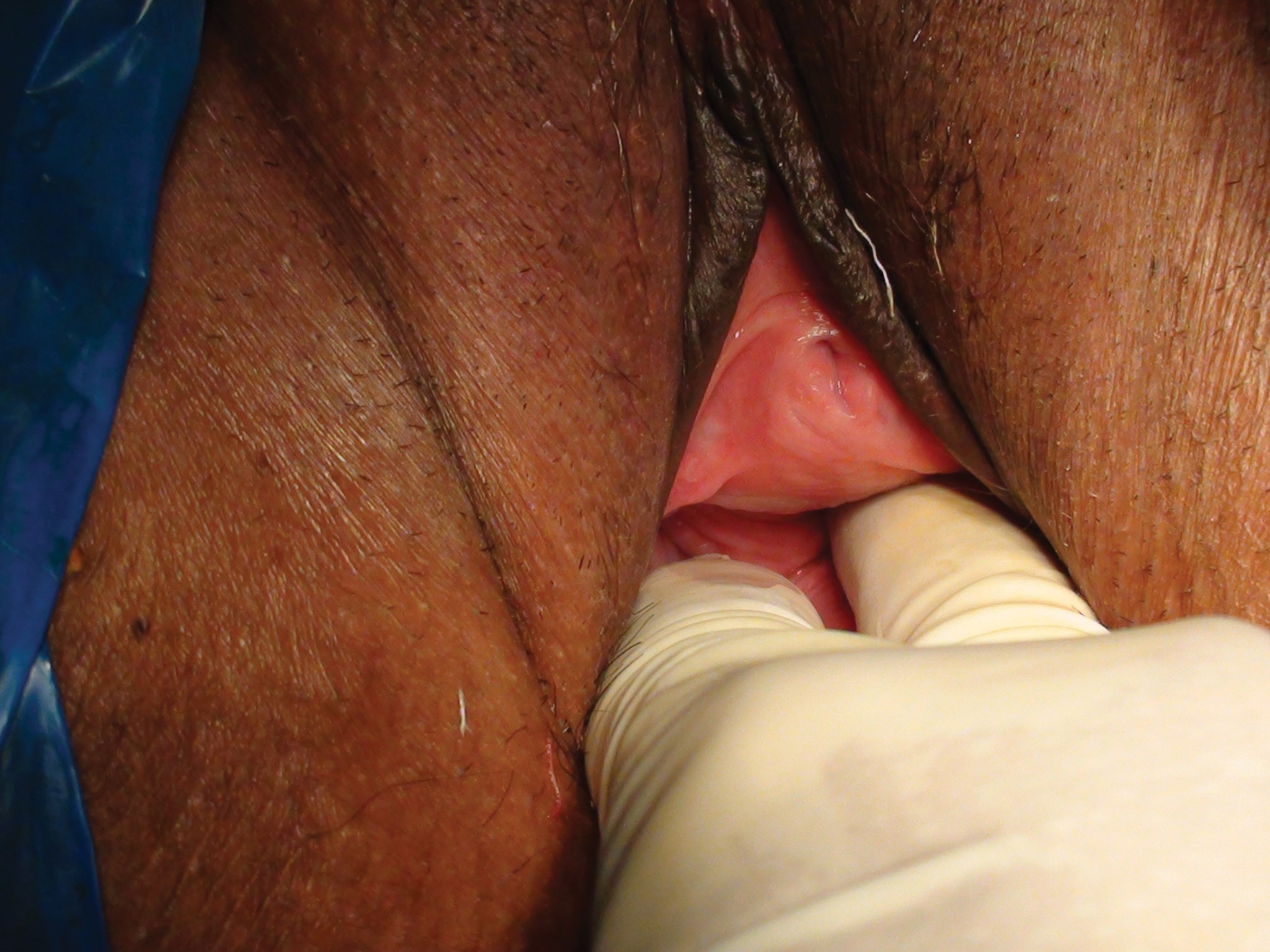
Figure 2: Showing loose vagina admitting two fingers with ease.
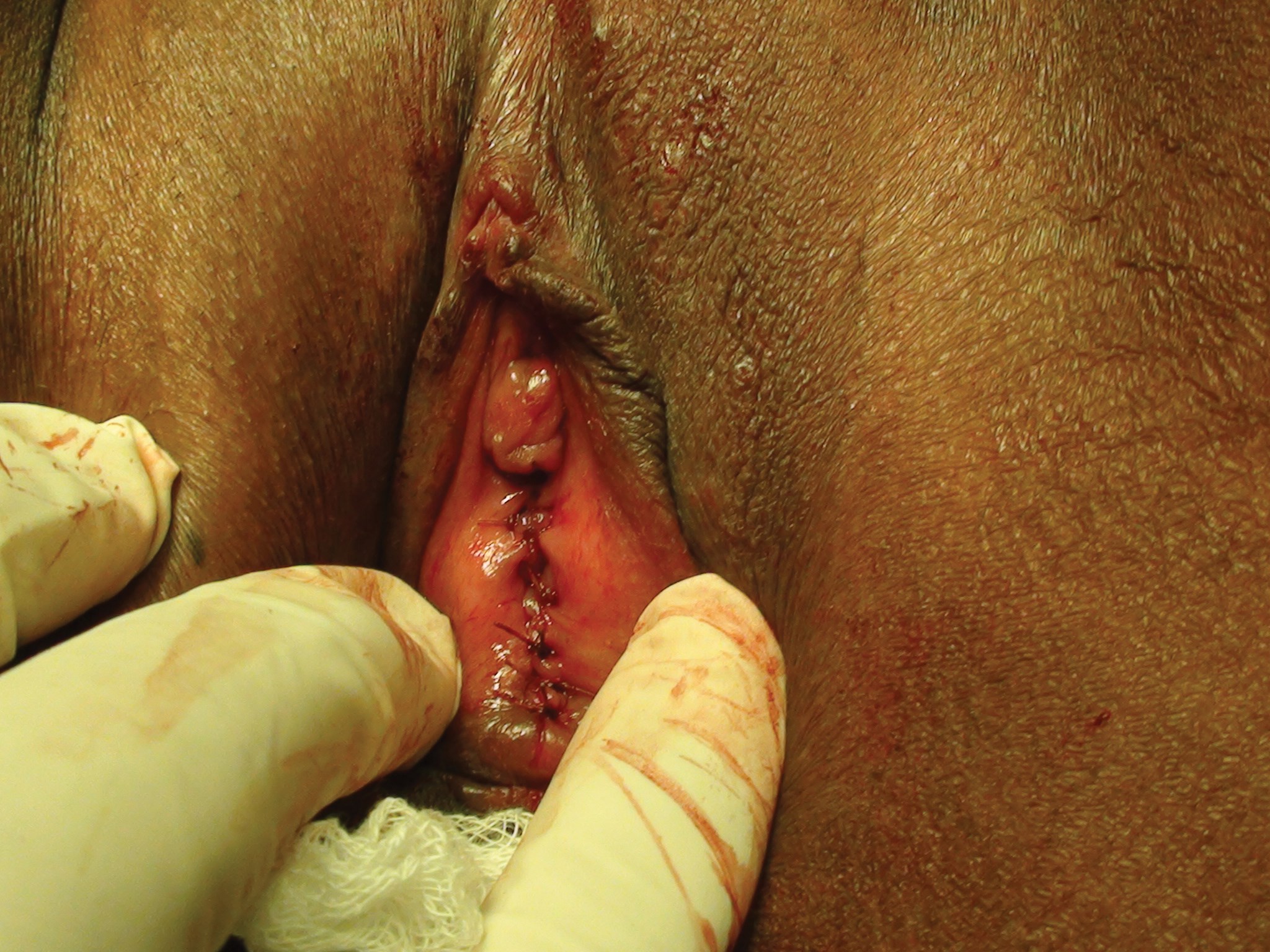
Figure 3: Showing completed hymenoplasty.
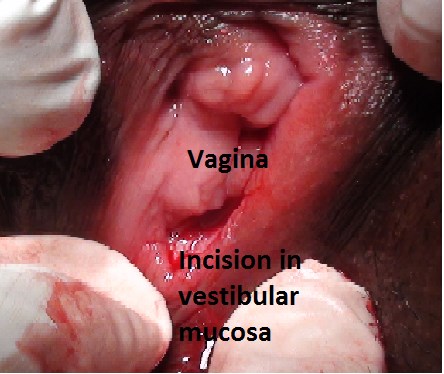
Figure 4: Showing incision in vestibular mucosa about
0.5cm posterior to posterior vaginal wall.
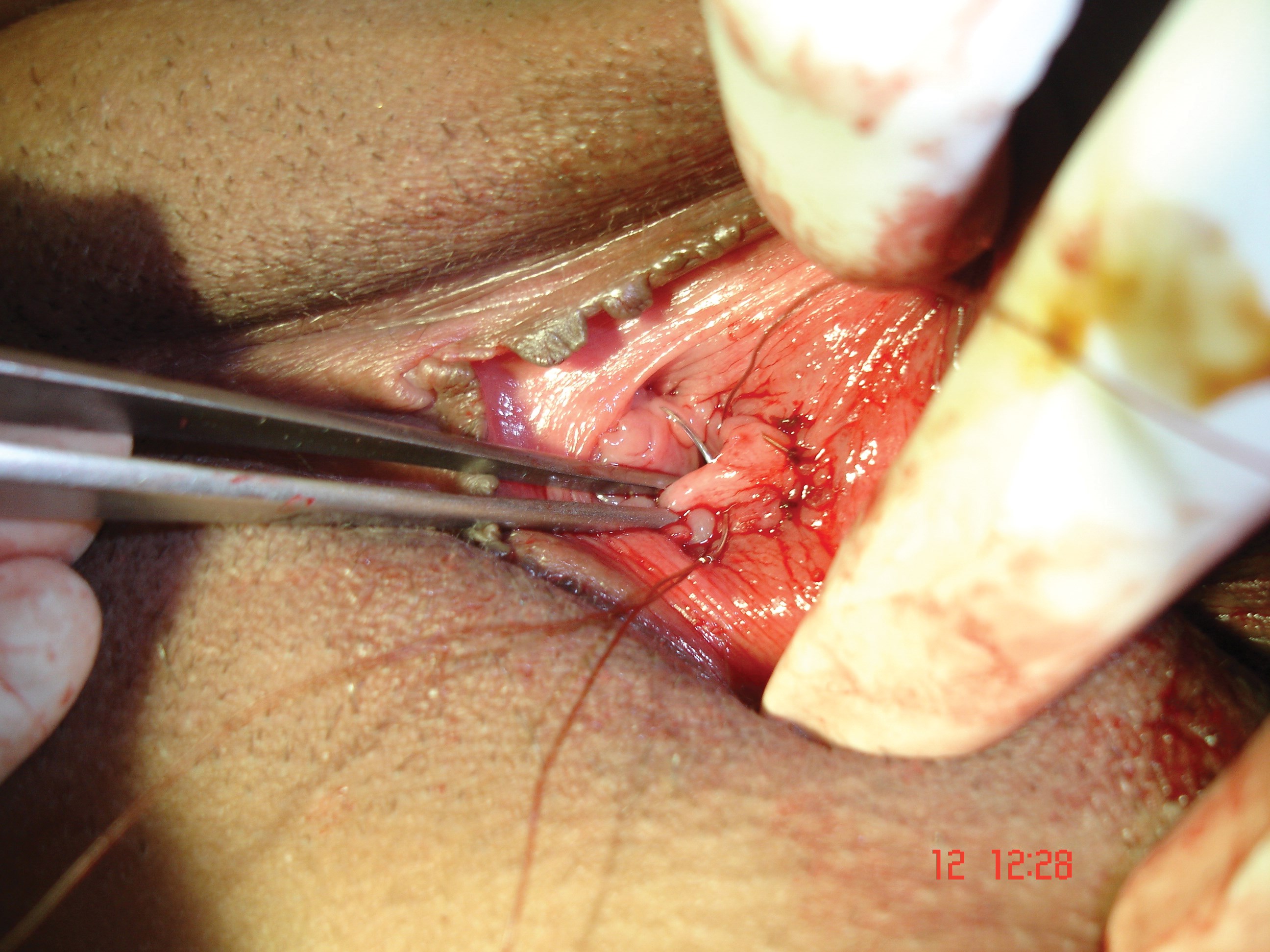
Figure 5: Showing reefing of superficial muscles.
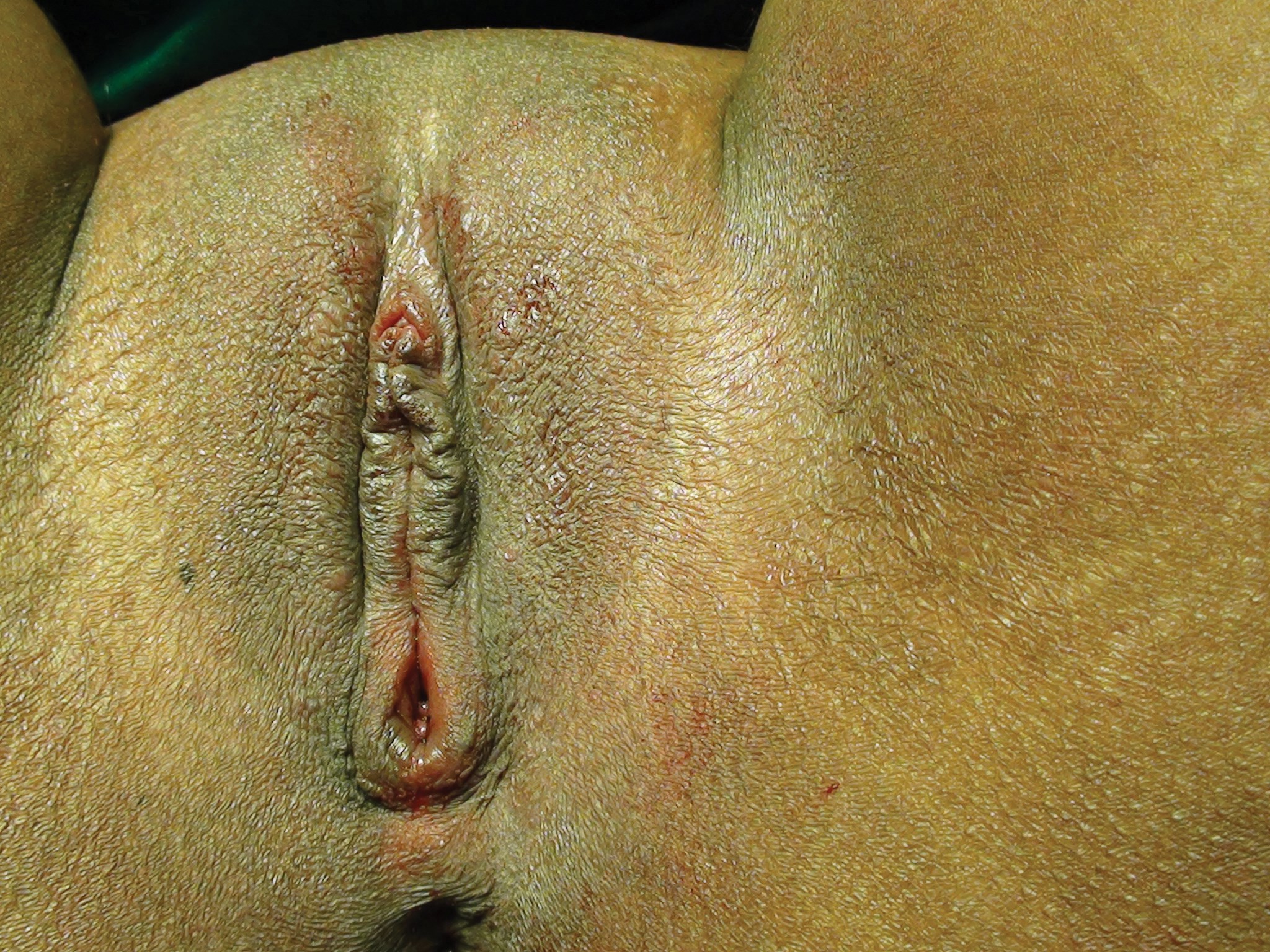
Figure 6: Showing completed revirgination after bulbospongioplasty.
Technique
The operation is performed under local or general anaesthesia as per the wishes of the patients. Forty-seven patients chose local anaesthesia and the remaining patients elected for general anaesthesia. Patients were placed in the lithotomy position. The surgical site was prepped and draped. The hymenoplasty was first performed by uniting the torn remnants of hymen (Figure 1-3). A transverse incision was then made in the vestibular mucosa posterior to the posterior vaginal wall (Figure 4). The posterior vaginal wall was raised as a flap and superficial muscles were reefed (Figure 5). The mucosa of posterior vaginal was tightened by creating rugae. Then, through the existing incision in the vestibular mucosa, the bulbosponsgiosus muscles were dissected on either side (Figure 6) and reefing was performed.
Creation of rugae
The rugi are created on vaginal mucosa by holding the tissue in forceps and passing a stitch from the superior end and exiting from the inferior end [3]. Many longitudinal and transverse rugae are created by this technique until the vagina is tight. Neosporin ointment was applied over the suture line and no dressing was given. Postoperatively, patients were advised to clean the area with warm water and apply the ointment, with no dressing being required. For pain relief simple analgesic tablets are enough. A combination of metronidazole and ofloxacine is given for five days.
Results
For the first seven days following revirgination patients complained of slight pain and occasionally slightly bloody discharge. After one week all patients stated they were comfortable apart from one individual who complained of pain for three months. There was no obvious cause for this.
In a follow-up study 17 patients responded. Out of this 16 were extremely satisfied on the eve of their first sexual intercourse after surgery. All 16 were extremely satisfied with vaginal tightness but three of the patients were not satisfied with bleeding, as they expected more post-coital bleeding. After their feedback we have devised another hymenoplasty procedure which we have called the ‘superhymenoplasty’. One patient was not satisfied with the tightness of the vagina. However, on follow-up vaginal examination only one finger could be passed with difficulty and it is possible that the penis of her partner was small, particularly on erection as happens in venous impotency.
Discussion
Genital plastic surgery for women has come under scrutiny and has been the topic of discussion in the mainstream media, both print and online, and in medical journals. In the absence of measurable standards of care, lack of evidence-based outcome norms and little standardisation, either in nomenclature or training requirements, concern has been raised by both ethicists and specialty organisations [4].
The celebration of the ‘bloody sheet’, portrayed in popular films, is based on strong religious and cultural beliefs. Religious texts state that a bride has to be a virgin, and according to certain customs a woman found on her wedding night to have been ‘touched’ brings shame to her family. Consequences include divorce and even death [5]. It is understandable then that young women go to great lengths to ensure their hymen is intact and repaired if necessary. However such a procedure is illegal in most Arab countries [6]. Moreover, currently an increasing number of patients are requesting hymenoplasty, not for fear of being discovered as unchaste, but because of a desire to be a ‘virgin’ on their marriage day and many with the knowledge and consent of their husbands to be. A similar observation has been made of couples requesting for the female to undergo hymenoplasty to mark a significant wedding anniversary and to enjoy a symbolic revirgination.
We must emphasise however that hymenoplasty and revirgination are not the same, and there is a need to change this perception in both patients and medical professionals. In addition, some surgeons will just remove the mucosa of the vagina resulting in tightening, which is certainly not a hymenoplasty; vaginal tightening done in this way results in dyspareunia. To avoid the problem of dyspareunia we have described a method which restores the ruage and tightens the vagina at the same time [3].
Whilst hymenoplasty and revirgination are not the same, neither of these should be confused with female genital mutilation (FGM) – previously known as female circumcision. Unlike FGM, hymenoplasty is performed on women who have reached the age of consent and who request the surgery themselves to regain the virginal status before marriage. Therefore, the medical, ethical and human rights arguments against FGM cannot be extended to hymenoplasty and not at all to revirgination. This is a cosmetic procedure like mammoplasty, etc. [7].
In Western society and in India hymenoplasty is legal. The concept of deception is not relevant. This operation is done for the patients, and the principle of confidentiality is as old as medicine itself. But factors such as sporting activities and the use of tampons mean that bleeding with first sexual intercourse is not essential [8]. An intact hymen was seen in only 57% of virgins in previous reports.
The role and need of hymenoplasty is debatable. But that is not true for the revirgination procedure. In revirgination the tightness created cannot be denied to a patient by any law anywhere in the world, and it is the right of every woman to request this. Every married couple is entitled to the feel of vaginal tightness and accompanying intensified sexual pleasure.
Irrespective of the scientific and ethical controversies, the demand for hymenoplasty is ever increasing. Hundreds of doctors advertise their hymenoplasty services over the internet. Unfortunately, there is usually no evidence of the results of the procedure. Unless specifically trained specialists can offer the procedure patients will be at the mercy of inexperienced doctors and the risks and complications of the procedure are not insignificant. Contraindications to this operation such as female sexual dysfunction, mental impairment and body-dysmorphic disorders should be emphasised before embarking upon this procedure. Women demanding such procedures should be made aware that they may undergo hymenoplasty or vaginal tightening but this does not mean that they are structurally abnormal.
Conclusion
Hymenoplasty is not same as revirgination surgery and patients do not always appreciate the differences. Women requesting hymenoplasty should be offered complete revirgination surgery which includes hymenoplasty, vaginoplasty and bulbospongioplasty.
References
1. Longmans A, Verhoeff A. Who wants the procedure and why. BMJ 1998;316:459-60.
2. Prakash V. How I do Hymenoplasty. Indian Journal of Surgery 2009;71:221-3.
3. Prakash V, Neeta G. New Technique for Management of Relaxed Vagina –Preliminary Study. Anaplastology 2014;3:1.
4. Goodman MP. Female Cosmetic Genital Surgery. Obstetric Gynec 2009;113:154-9.
5. Kandela P. Egypt’s Trade in Hymen Repair. Lancet 1996;347:1615.
6. O’Connor M. Reconstructing the hymen: mutilation or restoration. J Law Med 2008;16(1):161-75.
7. Ou Mc, Lin C, Ou D. A cercelage method for hymenoplasty. Taiwan J Obstetric Gynecology 2008;47(3):355-6.
8. Emans SJ. Hymeneal findings in adolescent women. J Pediatric 1994;125:153-60.
Declaration of competing interests: None declared.
COMMENTS ARE WELCOME