In part one of a two-series article Professor James Frame, from the Anglia Ruskin University, gives us his opinion on what needs to be done to improve cosmetic surgery and patient safety in the UK.
Cosmetic surgery is most easily defined as ‘the surgery of want rather than the surgery of need’ to improve, change or rejuvenate the human body from its normal shape, form or natural ageing process. Whether this is a patient with very large breasts that are symptomatic, a heavy abdominal apron that causes pain and intertrigo, a flat gluteal region that doesn’t allow trousers to stay up (Figure 1 and 2), an asymmetric thorax that causes significant breast size, a facial palsy causing drooling, a confidence draining class two malocclusion (Figure 3) or prematurely aged face, a nasal septal deviation causing breathing problems or pseudoptosis of eyebrows (Figure 4) causing visual field impairment, this is hardly the surgery of want because all the symptoms can improve massively if treated appropriately using modern cosmetic medical and surgery techniques.
This surgery is clearly the ‘surgery of need’ for many patients. Plastic surgeons therefore mainly perform ‘aesthetica’ which is the application of cosmetic surgery techniques to help those with disfigurement and deformity [1].
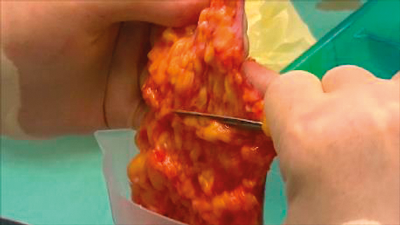
Figure 1: Autologous fat graft harvest. Composite of fat and fibrofat shaved from the subcutaneous deep surface of an apronectomy specimen following MWL. The patient had successfully completed a MWL programme but had the legacy of loose tissues. Traditional lipoharvest for large volume transfer is often impossible in these cases. Whilst bariatric surgery is carried out within the NHS the consequences of MWL are unfortunately rarely funded and consequently have to be carried out in the private sector. The modified Brazilian abdominoplasty is the surgery of choice for these patients because of a very low complication rate and rare need for drains. Very few units in the UK are aware of this procedure, preferring the traditional extensive undermining procedure with up to a 20% complication rate and two drains. A good example of aesthetica in practice.
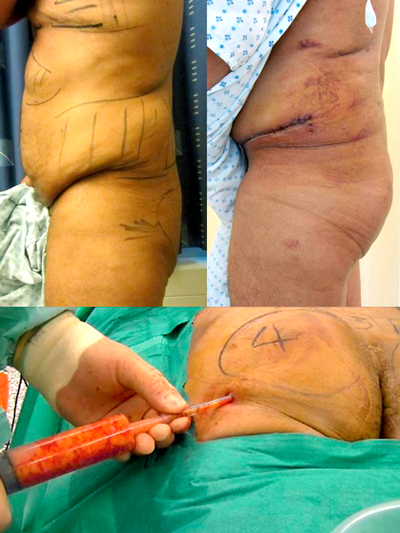
Figure 2: Pre and postoperative lateral buttock view of a 60-year-old male with no buttock projection. His problem of holding trousers up has been solved by augmenting the buttock with autologous fat harvested from the abdomen as shown in Figure 1. It is extremely unlikely that this surgery would be permitted within the NHS and therefore trainees have no exposure to the concept.
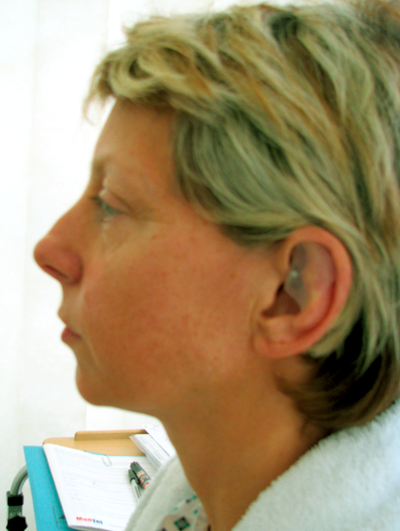
Figure 3: Preoperative lateral photograph of a 42-year-old woman lacking confidence because of a class 2 malocclusion. A small chin implant has boosted her confidence and she now has national awards in competitive ballroom dancing. Whilst it may be ‘surgery of want’ the psychological impact is huge and therefore can be justified as ‘surgery of need’.
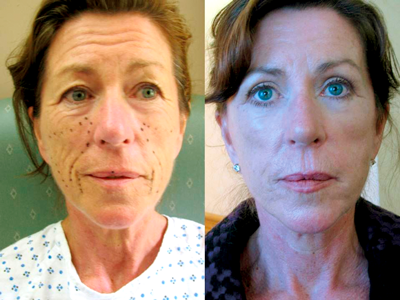
Figure 4: Pre and postoperative frontal view of a 54-year-old woman with visual field impairment caused by pseudoptosis of the upper eyelids which has been significantly and safely improved by standard upper eyelid blepharoplasty. This aesthetica can prevent accidental trauma caused by blind spot to vision.
Aesthetica can be easily misrepresented through ignorance but it should be remembered that plastic surgeons are unique in their training having dealt with serious and life-threatening illnesses, congenital disorders and traumas that disfigure, maim and bereave, and these are not seen in totality by any other specialty. The respectable plastic surgeon has an unquantifiable desire to improve function and restore appearance in such patients and to be rewarded by the knowledge that patients’ feeling of value and well-being has been restored.
“Aesthetica can be easily misrepresented through ignorance.”
Unfortunately the National Health Service (NHS), General Medical Council (GMC), Royal College of Surgeons and various national associations, for all their many values, do not accept that the ‘real’ completion date of training in plastic surgery should include an extended period of training for those interested in working in aesthetic surgery. This has already been recognised by training programmes elsewhere including in the USA. Real cosmetic surgery cannot be taught or practised within the NHS environment and for those newly accredited plastic surgery consultants that feel that they are so entitled to carry out these procedures in the private sector, there is a wealth of evidence from the UK and the USA to suggest the contrary, including a recent presentation to the Winter British Association of Plastic, Reconstructive and Aesthetic Surgeons (BAPRAS) meeting in 2017 from Manchester [2].
In addition, some NHS trainers are woefully inexperienced in many aspects of modern aesthetic techniques, including medical aesthetics, and this adoption of downward normalisation of standards is potentially harming patients [3], albeit not quite as much as when the GMC approves surgeons from the European Union onto the specialist register without any major scrutiny of that surgeon’s experience and outcomes. This is in contrast to the mandatory appraisals and revalidation required for UK Surgeons where NHS consultants are appraised on their whole practice, which by definition should include private patients. However, there is much debate as to the extent of such disclosure during an NHS-led and funded appraisal process. In the private sector there is a compulsory fee of about £800 payable to the private hospital to cover the fee of their appointed appraiser.
Cosmetic surgery needs to be learned and examined as a super-specialty, away from the rigours of the NHS. This then gives credibility to the independence of the appraisal system. The GMC needs to recognise and endorse the few good aesthetic surgery training programmes currently available and stop listening solely to those with very little actual experience in this field. For example, the Anglia Ruskin University has had such a programme for over five years and BAPRAS, British Association of Aesthetic Surgeons (BAAPS), and the Royal College of Surgeons were made aware of this. Their alternative accreditation scheme is designed to introduce an ‘approval to practice’ environment but costs significant sums of money to prospective cosmetic surgeons seeking a license to practice cosmetic surgery within an anatomical area.
A much clearer thought process needs to go into this and should be inclusive of the opinions of other reputable aesthetic surgeons, from whatever their specialty base. If we normalise low standards of care we do not allow patients to get the best treatments and in ignorance we do not then understand the importance of aesthetica.
Who can do cosmetic surgery?
Like it or not cosmetic surgery is now interdisciplinary. The days when plastic surgeons kept a closed shop on the subject have long gone. It is now the realm of the interdisciplinarians on the regulatory committees who may collectively outweigh the wishes of the plastic surgeons. Cosmetic surgery has become a scrum of oft cavalier, website-promoted, self-promoted individuals with any medical degree playing for the busiest practices. For some in cosmetic medicine the standards are so low there is no need for a medical degree. This is the ‘lure of the loot’ effect and in addition to the good guys, this has been an invite for failed and unscrupulous surgeons to enter a lucrative market, where media and website skills promote and misrepresent the actual experience and skill of the surgeon.
As many will know you can train just about anyone to do surgery but understanding the effects on the individual, from the range of physical harms to psychological disasters, cannot be taught without tissue handling experience in disfigurement and deformity. As many a plastic surgeon has said to me “If we can’t beat them being honest brokers in this field, we have to join them and do it better”! This philosophy hasn’t helped protect the vulnerable patient. Unfortunately ‘they’ have beaten us again by publishing standards on outcomes before the plastic surgeons have their act together and so have set the yardstick by which we must all be measured. A 3% reoperation and complication rate is what we aim for, at the very worst, but unfortunately 30% is nearer the mark when all complications are taken into account, even in some of the better units. Surely this is unacceptable?
Publishing outcomes is therefore essential and if we want to improve patient care these need to be centrally held and monitored in a situation that can offer advice and corrective management. Although BAAPS ‘markets’ annual data through the media, it is non-validated, outdated and non-representative of the industry as a whole with a large proportion of the busiest plastic and non-plastic surgeons’ cases not being represented within the data collection because they are not members of this association. If there can be a certification scheme, and a mandatory ‘whole practice assessment’ during appraisal, surely there can be a central data collection point for aesthetic surgery. Even though this has been suggested many years ago to BAAPS, the Anglia Ruskin University would still be happy to take on this independent validation role, if invited by the higher authorities and regulators.
Prerequisite skills
I can’t speak for the training of consultant ENT, oral, breast and general surgeons but plastic surgeons rotate through ‘firms’ of special interest that include the repertoire of the general plastic surgeon within the NHS. As in plastic surgery training I suspect that there is little or no cosmetic surgery training in these NHS specialties but eventually, once they have courage, many will learn on the hoof after becoming consultants. The interval for this will be measured in years and in between there will be de-skilling even if they had received previous training. You can’t walk into a private practice unless you join a ‘group’ and in this event you are in a ‘chop shop’.
Trainee plastic surgeons are examined for the FRCS(Plast) just after the midway point of their training – far too early as far as I am concerned – and can elect to do aesthetic surgery towards the end of training should they so wish. Most don’t do this and there is some evidence that they are advised against this if they wish career progression within the NHS. This is a disgrace, of course, because the skills learned in the private sector are to the advantage of all within the NHS. Burns patients are the most challenging of all patients to treat and if their well-being can be aesthetically improved by modern techniques in cosmetic surgery, then they should be offered the chance (Figure 5). Here is where the skills of the aesthetic surgeon have to be taught to surgeons in training, for the benefit of the patient. It is also amazing what medical aesthetics can offer such patients but NHS training in this field is negligible.
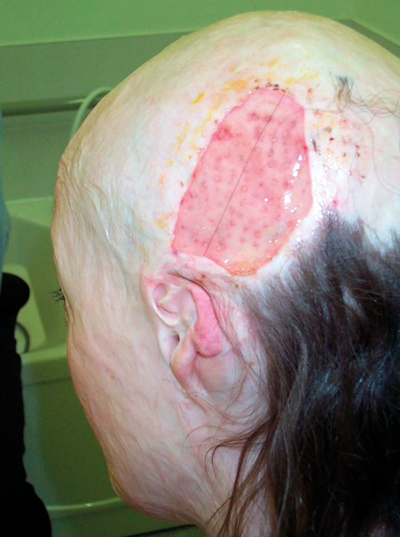
Figure 5: Aesthetica research in practice. Attempting to improve appearance of scalp in a young girl using ‘immunoprivileged’ allogeneic single follicle hair grafts at 1cm spacing through fresh integra into a burn scar scalp. The consented donor was her mother and there is a complete re-epithelialisation after separation of the silicone layer at three weeks, without the need for autograft. This concept had been applied to a massive burn injured patient with successful long-term healing using autologous micrografts through intact integra. The surgical technique of micrografting is the same as that used in the private cosmetic sector for male pattern baldness. Immediate burn injury excision and cover with integra means that the follicle grafts can be carried out at leisure post injury. It is however easily carried out as a primary procedure soon after injury.
Maybe platelet rich plasma (PRP) or stem cell generated proteins can generate tissue healing and a return to normality after injury or even reverse the ageing process as claimed. This is what is actually going on in aesthetic surgery research. A plastic surgeon needs the dexterity and finesse of fine hand motion, clarity of thought, the ability to make rapid and accurate decisions, to have artistic skills and realism of outcome. Above all though the plastic surgeon needs to be able to deal with the difficult, unrealistic or dysmorphic patient and the patient with less than satisfactory outcomes from surgery.
Working the tissues
It is hardly ever mentioned that exceptional tissue handling skills by the surgeon are mandatory if complications are to be avoided. Within this though is the importance of recognising that soft tissue compliance and strength varies between individual patients. Avoiding surgical dead space is mandatory and it should therefore be very rare to use drains in aesthetica. Surgery is not a race, it is a process of precision and layered closure in as rapid a time as is required; but in virtually all cases surgery should be completed within five hours to avoid well known complications.
Whilst the use of multiple teams working simultaneously on patients can be of benefit and shorten anaesthetic time it does create more of a challenge to the anaesthetist and may increase risk to patients in some instances particularly with decompensated blood loss as seen during massive weight loss (MWL) surgery. The surgeon’s skill is to know how to compensate and adapt the technique to ensure speedy, efficient surgery and avoid suture cheese-wiring, haematoma, infection and poor scar.
Specifying the anatomical area of expertise
We all know what is needed yet most are too scared to say it. This is the Dunning Kruger Effect (DKE) [4] and those that are making the new rules suggested by the GMC need to reflect on what they are offering. They may not be right and perhaps the ‘DKE negatives’ need to be consulted. NHS trainees have no experience or training in cosmetic surgery in the UK – period. They have neither been examined in cosmetic surgery, nor have they actually operated on cosmetic surgery patients and a logbook showing to the contrary needs closer scrutiny. Forgive me, but attending an annual BAPRAS conference with very little aesthetic surgery content or being second assistant in closing a deep inferior epigastric perforators (DIEP) flap donor site, augmenting a post-mastectomy patient or assisting in parotidectomy cannot possibly permit the granting of privileges to operate on cosmetic surgery patients in the private sector, yet this is what is going to happen. It is all very well specifying and paying for the privilege to register to work within an anatomical area of expertise but this is a nonsense to the fully trained plastic surgeon who has earned the right to operate within all regions of the body and needs unrestricted freedom to operate in all areas.
Obviously there will be a rush to register from non-plastic surgeons and those not on the specialist register. Who is going to offer buttock augmentation – the rectal surgeons? Give us a break! In addition surgeons have to pay thousands of pounds for the privilege of being granted a certificate by a quango of dubiously qualified practitioners anyway. This is a license for the unscrupulous to harm unsuspecting patients yet it seems the Care Quality Commission (CQC) will enforce the certification of surgeons before they can practice at that private hospital. I doubt whether medical indemnity companies will be so easily fooled by the value of these certificates otherwise they might have to lower their premiums!
References
1. Klaassen MF, Frame JD, Levick P. Aesthetica in practice: the flick lift in assisting closure of large cutaneous excisional defects on face. Clin Surg 2017;2:1684.
2. Pantelides N, Highton L, Lamb A, et al. An analysis of the cosmetic surgery experience that UK Plastic Surgery registrars acquire during their training. Presentation at BAPRAS Winter Scientific Meeting 29 Nov 2017.
3. Halligan A. The Francis Report: what you permit, you promote. J R Soc Med 2013;106:116-7.
4. Kruger J, Dunning D. Unskilled and unaware of it: how difficulties in recognizing one’s own incompetence lead to inflated self assessments. J Personal Social Psychol 1999;77(6):1121e34.
Part 2 of Prof Frame’s fascinating article is available here.
Share your views on these topics in a letter to the editor, by emailing diana@pinpoint-scotland.com
COMMENTS ARE WELCOME





