
Why do we need awareness?
Around 40% of women in the UK are overweight or obese. Yet, within that 40% statistic, is a sub-set of women for whom that is not the full story. They suffer from a condition called lipoedema, which actually lays down fat and makes it difficult to lose weight.
Most women have neither heard of it nor know they have it, so they struggle, not only with weight gain, but the humiliation and negative stereotypes, even though they know, deep down, that something does not add up about their situation. Many doctors have also never heard of it either, so raising the profile of this condition is vital.
Awareness surrounding every aspect of lipoedema must improve, as it affects an estimated 11% of the whole adult female population.
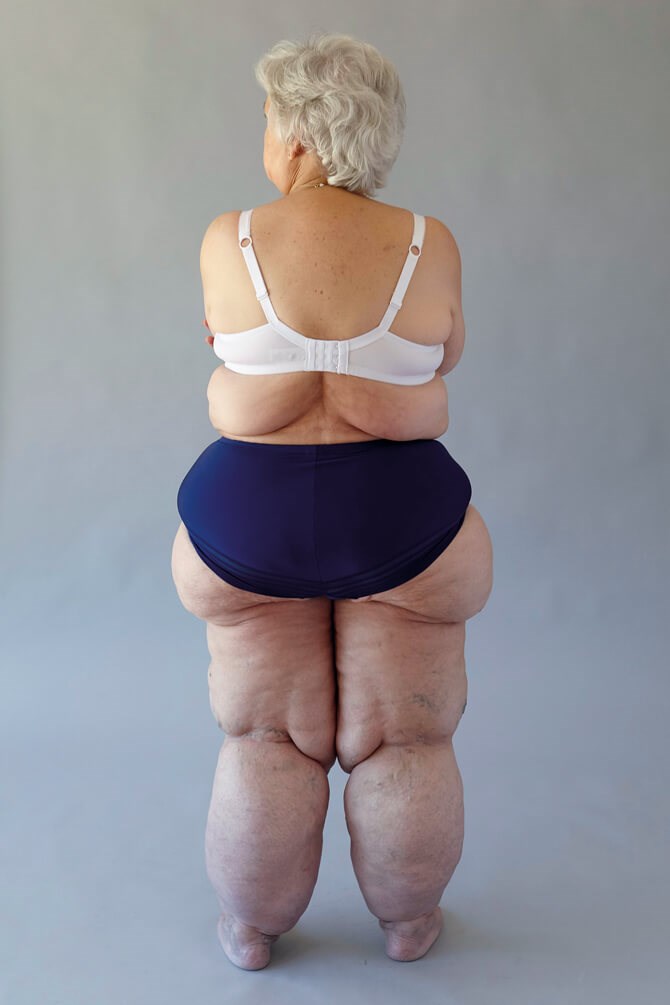
What is lipoedema?
Lipoedema is thought to be genetic and, almost exclusively, affects women. It is triggered at times of hormonal fluctuation, such as puberty, pregnancy and the menopause, when an excess accumulation of rogue fat cells forms in the legs, hips and buttocks. The upper body is not affected (except for arms in some types), so the size of the lower body is disproportionate and the body shape is distorted.
This body type would be described as an endomorph; stocky and built for endurance rather than sprinting, with slower metabolism and higher fat content. Over time, the ‘pear-shaped’ fat distribution may progress to gain the appearance of harem pants, with characteristic ‘cuffs’ at the ankles but the feet are typically not affected.
Because of low-level inflammation and distended tissues, there can be several symptoms including pain and tenderness, fatty lumps and bumps, a pale appearance, easy bruising, spider veins, varicose veins and cellulite with the appearance of a buttoned mattress. The lipoedema fat, itself, is abnormal, containing over 4400 differences to normal fat. The membrane walls do not respond to regulating metabolic signals to stop growing or accumulating, while oestrogen within the abnormal connective tissue triggers stem cells to turn into more rogue fat cells, which can grow to an extraordinary size.
When women seek medical help because of their symptoms, lipoedema is often misdiagnosed. This is very common because lipoedema shares characteristics of both obesity and another condition, called lymphoedema. Lymphoedema causes limbs to grow, but is due to malformation from birth or damage to the lymphatic system.
Lipoedema is not a progressive disease, as it does not progress on its own, but is made substantially worse with any weight gain and natural ageing. Although not every lipoedema sufferer has an eating disorder, most women with lipoedema have known disordered eating throughout their lives, as weight gain is extremely easy and laboriously difficult to keep stable or lose. Most women have yoyoed or struggled with constant food deprivation and crash dieting, whilst accused of being overweight or eating too much. Dieting does shed weight, but it often drops normally from the upper body, while stubbornly clinging to the lower body, thus enhancing the disproportion. This cycle often dominates internal dialogue and leads to endless issues with confidence and self-esteem, which are especially cruel if lipoedema kicks in at puberty when young girls are so vulnerable to lifelong poor self-image.
What is the cause?
The cause is, as yet, unknown. First described in 1940, by Drs Allen and Hines of the Mayo Clinic in America, the name lipoedema (lipid-fat, oedema-fluid swelling) was coined to describe a condition of abnormal deposition of fat in the lower legs and buttocks with an accumulation of fluid. It remained under the radar for decades. The second world war and subsequent food rationing had a negative effect on cases, but with the advent of hormonal contraception and replacement therapies, intensive farming practices, the arrival of ultra-processed foods, improved nutrition and increased lifespan from the 1960s; the incidence of lipoedema and obesity have continued to balloon to crisis point. Awareness of lipoedema only really grew in the UK from 2011, when the first patient charity, Lipoedema UK (www.lipoedema.co.uk) was formed, followed by Talk Lipoedema (www.talklipoedema.org) in 2015. In real terms this makes it a newly recognised condition.
Hormonal imbalance is implicated because lipoedema appears at times of oestrogenic fluctuation, and in places where fat stores traditionally accumulate so that women can feed babies; thighs, hips, buttocks, upper arms, tummy. However, this is only part of the puzzle. Many women with lipoedema have co-existing autoimmune conditions, connective tissue disorders or inflammatory conditions. From gut malabsorption to polycystic ovaries, thyroid dysfunction to Ehlers Danlos Syndrome, many lipoedema patients are extremely complex. They seem to have problems with regulating and balancing numerous hormones.
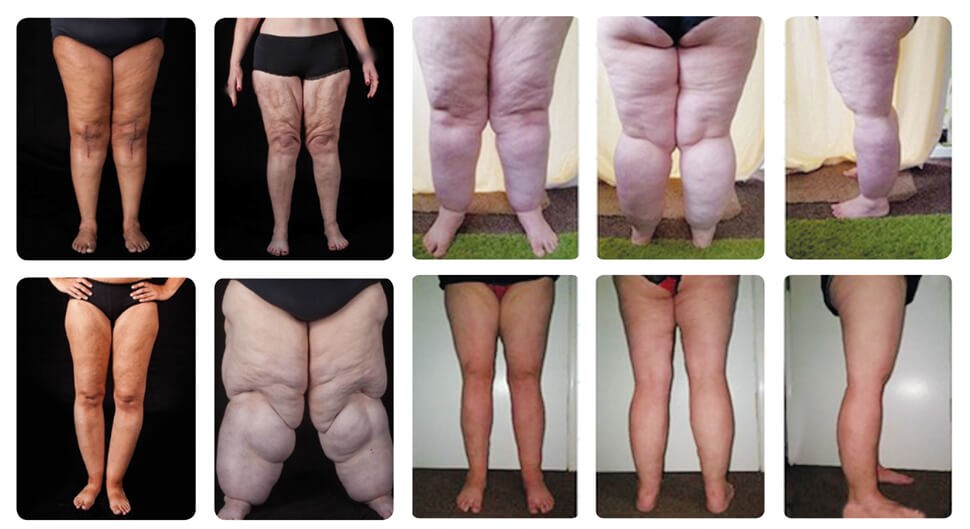
These images highlight some of the stages and types of lipoedema. The condition may present at puberty, during pregnancy or around the menopause. All stages have a negative impact on the quality of life for an individual. Early recognition and treatment are vital to prevent progression and deterioration. Images used with permission from FDRS https://www.fatdisorders.org/
How is lipoedema diagnosed?
It is important to understand that every case of lipoedema is as individual as the person. Lipoedema is often classified as having five types and four stages. Every combination of these is possible, plus the age of onset is different for everyone, making a definitive diagnosis very difficult; especially given the potential of co-existing symptoms of rare autoimmune illnesses. There are currently no specific investigations to diagnose lipoedema, so it is based on a differential diagnosis of probability, which includes a complete holistic assessment with past medical and family history and a thorough physical examination.
The usual biometrics can be misleading, especially the body mass index (BMI), used to establish obesity, because every litre of carried lipoedema fat weighs 2lbs or 1kg, and the fat can be extremely compacted. This is why so many women have been incorrectly diagnosed as obese by stepping on the dreaded scales. Instead, with the ‘classic’, most recognisable presentation, where the hips are disproportionally larger than the waist measurement, the difference between these two measurements, ‘the waist to hip ratio’ is seen as a more accurate, reliable diagnostic tool.
In earlier stages of disease, diagnostic tests for lymphoedema (called lymphoscintigraphy) and lymph scanners show that most stage one and two lipoedema patients have perfectly healthy lymphatic systems and normal levels of fluid within their tissues. If large amounts of weight are gained, it is thought that the lymphatics, nerves and blood vessels are overwhelmed with fat cells, leading to a lack of oxygen. This could explain why pain and bruising occur, except that many women also report fibromyalgia, hypermobility and chronic fatigue. These conditions are currently studied in the field of myofascial or connective tissue research, where there is much to compare and contrast when searching for answers for lipoedema, which has more recently been described as ‘a disorder of the loose connective tissue’.
How is lipoedema treated?
Conservative treatments for lipoedema require a variety of procedures including, lifestyle interventions, dietary changes, exercise, manual lymphatic drainage, deeper connective tissue massages and medical compression therapy to limit pain and control fluid content. Treatments depend on how debilitating the condition has become before it was diagnosed. Many older women have taken an average of 30 years to be diagnosed, because awareness was limited before 2011. For some, the lipoedema has progressed unfettered over a lifetime of hormonal change and become a major disability; with distorted legs and skin folds making normal movement impossible.
Getting treatment
However, suspecting you have lipoedema and getting treatment for it are often two different things. In the UK we are used to the NHS providing diagnosis and clearly delineated pathways of care. This is rarely the case with lipoedema. In fact, there are still many medics who have never heard of it. There is growing awareness within the healthcare professions, so this scenario is not as familiar as it was five years ago, but it is still frustratingly commonplace.
In the UK, each medical condition has an official code from the World Health Organization (WHO), International Classification of Diseases (ICD) – currently under 10th revision – thus, an ‘ICD-10’ code. Lipoedema has yet to receive its own UK ICD-10 code. Without this, lipoedema does not technically exist, so it is not taught at medical schools, which explains the lack of knowledge from many GPs, nurses, doctors and consultants.
Without a UK ICD-10 code, there can be no protocols for treatment or gold standard care pathways and lipoedema patients cannot receive specific NHS funding for their care. While this situation continues, no lipoedema specific statistics are being collated by healthcare providers to put forward a financial case to support lipoedema funding in the future, so a vicious circle exists. This is quite unbelievable for a condition that could affect around 1 in 11 women in the UK (a widely adopted statistic, but there are no official NHS data to refute or verify this).
Non-cosmetic liposuction
Another issue relating to the lack of a UK ICD-10 code, is that apart from conservative lifestyle management, non-cosmetic liposuction surgery is considered gold standard treatment to debulk and remove lipoedema fat. Water-assisted liposuction for lipoedema was pioneered early in the 2000s and has been adopted worldwide. Women often require a series of procedures to treat separate body areas, over many months or years.
Doctors and surgeons in the UK began providing liposuction, but to date, there are still no official treatment protocols or parameters regarding which type of liposuction is suitable to use, safe weight restrictions for patients or the maximum number of litres that can safely be removed during one procedure. Very large women, who represent a high-risk patient group for complications, were having in excess of 10 litres of fat removed during each procedure. Following a fatality in 2019, where the performing surgeon was cleared of any wrongdoing, limitations were introduced. In 2020, guidelines were written for members of the British Association of Aesthetic Plastic Surgeons (BAAPS) and the British Association of Plastic Reconstructive and Aesthetic Surgeons (BAPRAS).
The National Institute for Health and Care Excellence (NICE) convened to write guidelines on the suitability of liposuction for lipoedema and whether the procedure should be offered by the NHS. The guidelines were published in March 2022 and concluded that there was inadequate evidence on the safety or efficacy of liposuction for lipoedema and raised concerns about possible major adverse reactions. Its recommendation was that liposuction for lipoedema in the UK, should only be used in the context of research. The committee will reconvene when the results of the large, randomised controlled LIPLEG trial that is currently underway in Germany are published. Final data are expected in 2024 and are likely to show that patients benefit when liposuction is performed as an early intervention. However, even though the recommendations clearly state that liposuction should only be used in the context of research, NICE guidelines are only advisory and various types of liposuction for lipoedema are still available in the UK. However, this may pose problems for surgeons, both in the NHS and in private practice, as these guidelines may be adhered to within the organisation's governance framework.
Where is lipoedema treated?
Lipoedema is currently treated under the NHS lymphoedema services, where its recognition, understanding and management have been developed over the years, by clinical experts looking after another specialist niche area in medicine. Lymphoedema clinics are composed of very small, overloaded and underfunded specialist teams, who treat swollen tissues due to cancer and its treatments or failures of lymphatic drainage.
Patients with lipoedema have, as yet, received funding for their treatment through the ICD-10 code for lymphoedema, as an invisible sub-sector, when referred by their GPs into lymphoedema services. There are clinical overlaps, as lipoedema and lymphoedema can co-exist, yet lipoedema is not caused by lymphatic failure nor does it fully respond to treatments for lymphoedema. For every woman with lipoedema who presents at a lymphoedema clinic to receive compression garments for her condition, more funding is received for lymphoedema management. There is a growing trend for patients with lipoedema to be turned away and denied care by their local lymphoedema clinics because there is no longer capacity to support them without specific funding, in extremely oversubscribed NHS services since COVID.
Political turmoil
This leads to a perfect storm. Lymphoedema can no longer support lipoedema. It is time for change. At present, everything about lipoedema is up for intense debate, from its causes, presentation and diagnosis criteria to its treatments.
Without understanding how lipoedema occurs and advances, it is difficult to develop treatments or cures, so it is imperative that researchers uncover the aetiology of the disease. Lymphoedema experts from around the globe have written documents on how to treat lipoedema from their perspective for years; these ‘consensus documents’ contradict each other. The recent 2020 European Consensus document is controversial, as it claims that there is no oedema in lipoedema and suggests a name change to lipalgia (lipid-fat, algia-pain) syndrome; but, as not all lipoedema patients have oedema, not all have pain either. The document advocates bariatric surgery and psychiatric support for patients. It has split opinion and caused shockwaves through a once united, international lipoedema community, who have divided into two new factions: the International Lipedema Association (ILA) formed in 2022, who advocate the contents of the 2020 document, and the World Lipedema Alliance (WLA), formed in 2023, who do not. While debate intensifies, there are implications for lipoedema patients in the UK. NHS Wales have already adopted the ILA position. New diagnostic and treatment pathways have been implemented for lipalgia syndrome, which exclude many women, who are being denied treatment under the new criteria. Lipoedema needs to emerge from the current situation separate from lymphoedema, with its own classification and its own panel of lipoedema experts to write specific treatment protocols.
Patient power
With this political and medical maelstrom of inconsistency, an unusual vacuum of knowledge exists for patients, which makes them very vulnerable. Their salvation lies in private sector medicine, and the information about what treatments to seek out is driven by powerful, lipoedema patient peer groups that flourish online to support, educate and empower each other. Such validation can be exhilarating and emotional after a lifetime of self-loathing, feeling fat, greedy, misunderstood, denied and a hostage inside your own skin. Finding a spiritual home in the company of others who have trodden the same path becomes a very strong sisterhood.
The groups are full of excellent threads, answers to diverse and interesting queries, product reviews, up to date research, advice on everything from diet, exercise, supplements, drugs, fashion, treatments, therapies and liposuction surgery, and give unique insights into how lipoedema affects lives. International groups share knowledge which is local to their country and time zone, that might not be relevant to all members because of different healthcare systems, but it often informs gold standard practice for those who are able to pay for it. For instance, following online conversations with their USA ‘lippy sisters’, the newly registered NHS wonder jab for obesity, semaglutide (Ozempic® or Wegovy®), has been procured on private prescription by many UK lipoedema patients for years for its useful, ‘off ticket’ side-effect of weight loss, when it was only available on NHS prescription for type 2 diabetes in the UK.
A specific Facebook group, ‘Global Lipoedema Awareness-Surgeries/Doctors’, with 21,000 members, holds a meticulous database of every specialist lipoedema liposuction surgeon in the world, along with their location, speciality and cost per procedure. Within the group, members can research, plan and post every aspect of their surgical journeys with women who have undergone their own series of surgeries. Pre and postoperative photographs are shared for comparison, with personal reviews of surgeons and facilities, preoperative planning, where to source properly qualified manual lymphatic drainage therapists, postoperative complications and realistic outcomes; even what extras to pack in your suitcase.
On the flipside, these groups are echo chambers, misinformation abounds, and it is difficult to fact check. Women post photographs of themselves to be diagnosed by keyboard experts, while hearsay becomes verified fact. As with any online community, there are good and bad aspects.
The private health sector
Because of these avenues of self-research, awareness of lipoedema and its treatments is growing rapidly amongst the women who worry they might have it. With most medical conditions, ‘patient led’ care means the experts take the patient’s wishes into account when planning their treatment pathway. With lipoedema, the narrative is often led by the patient, who enters the GP surgery with a folder full of leaflets or printed research and a triumphant look on her face, as she can finally validate her long-term intuition that ‘something is wrong with me,’ without accepting a repeat diagnosis of having lymphoedema, or being overweight and being given yet another diet and exercise plan. Possibly, the blank look from the doctor is even more demoralising than the disingenuous lifestyle advice? Faced with years of ignorance from GPs and nurses who have not been educated on lipoedema, sufferers begin by being frustrated, which over time, degenerates to becoming desperate and angry. Patients know they are very well informed, but they are often demanding things that are not even available on the NHS. So where do they turn?
Unknowing patients can be easily swayed by glossy magazine articles and slick, self-promoting, filtered or photoshopped Instagram ‘before & after’ campaigns, where ‘likes’ and ‘follows’ dictate the calibre of the surgeons, practitioners and therapists far more than any qualifications or experience they may have.
But the stakes are high. Finding the right way to control and manage lipoedema, or have liposuction surgery to remove it, can be completely life changing. Belonging to positive communities who understand can also be extremely life affirming. Thousands of women every year transform their bodies and their attitudes towards lipoedema to either embrace themselves with it or treat it. Their shared successes uplift and educate the whole community and give hope.
Looking to the future
How can things change? Sharie Fetzer, chair of Lipoedema UK says: “It all comes down to the lack of facts – on top of that it is really important to start documenting early lipoedema and the effects of early treatment. All the current thinking and research is based on older, later stage patients. Patients are tarred with being ‘responsible’ for their own weight gain but are denied any support offered to genuinely obese patients. We need money to invest in long-term studies, following young patients and proper evidence to show what differences there are in the mindset / lifestyles of people who gain weight and why, along with the medical consequences of a disproportionate body. Modern food is generally highly processed and bad for everyone, is it far worse for people with lipoedema? What are the effects of contraception? Have the number of women with lipoedema increased with the introduction of contraceptives and junk food? How do we collect stats? There are so many questions.
Awareness of lipoedema is growing exponentially every year, from vibrant online communities, charities and associations. Healthcare professionals are working diligently towards getting recognised classification and treatment pathways for this complex condition, while they support the, equally complex, women who have it, in the hope that the upcoming generations of girls with lipoedema will not struggle to receive timely healthcare, unlike the ones who came before them.
Resources
BAAPS and BAPRAS members promote safety, innovation and research and do not recommend liposuction for lipoedema under the current NICE guidelines.
Charities like Lipoedema UK advise and advocate on behalf of their members, petitioning parliament and the NHS to give them a voice.
Nationwide registers of lymphoedema and lipoedema specialist therapists are available from MLDuk (www.mlduk.org.uk) and the British Lymphology Society (www.thebls.com).
The first UK course developed to specifically diagnose and manage lipoedema has just trained its second cohort of clinicians at the Lymphoedema Training Academy in Staffordshire, which also holds a register of therapists they have educated (www.lymph.org.uk).
COMMENTS ARE WELCOME





