The radix-rhinion complex forms one of the most important pillars of nasal aesthetics. Due to its complex anatomical nature and distance from the point of access, this region can be commonly involved in suboptimal results.
Tailor-made operative planning
Most of the undesirable effects of rhinoplasty in this region can be prevented by adequate preoperative facial analysis and subsequently, the creation of a tailor-made surgical plan [1].
The desired position of the radix needs to be planned based on factors such as the patient’s racial background, the length of the nose, and its overall projection. Although the height of the radix is usually described as being at the same level as the supra-tarsal crease, this must be carefully considered in view of the overall harmony of the facial features [2]. First, the nasal tip must be analysed in terms of its projection and rotation. Once this has been decided, a healthy, straight dorsal line becomes the ultimate goal. In female patients a very mild concavity may be acceptable, however, in general, the aim should be a straight line from the tip to the radix. Therefore, the position of the radix follows naturally from the desired position of the tip, the dorsum, and the particular racial characteristics of the patient [3,4].
Sources of error
The commonest source of over-reduction of a hump is misjudgement of the angle of the humpectomy instruments during the procedure. Furthermore, blunt instruments shatter bone, rather than cut through them, resulting in unpredictable lines and palpable irregularities in the postoperative period. Powered instruments have been developed in recent years in order to reduce this source of error, however, without correct planning, it is still possible to over-resect the dorsum [5,6]. In addition, failure to release the bony-cartilaginous hump from the overlying soft tissue envelope can lead to irregular tearing of the procerus muscle, intraoperative difficulty in removing the excised segment, and unnecessary postoperative contusion.
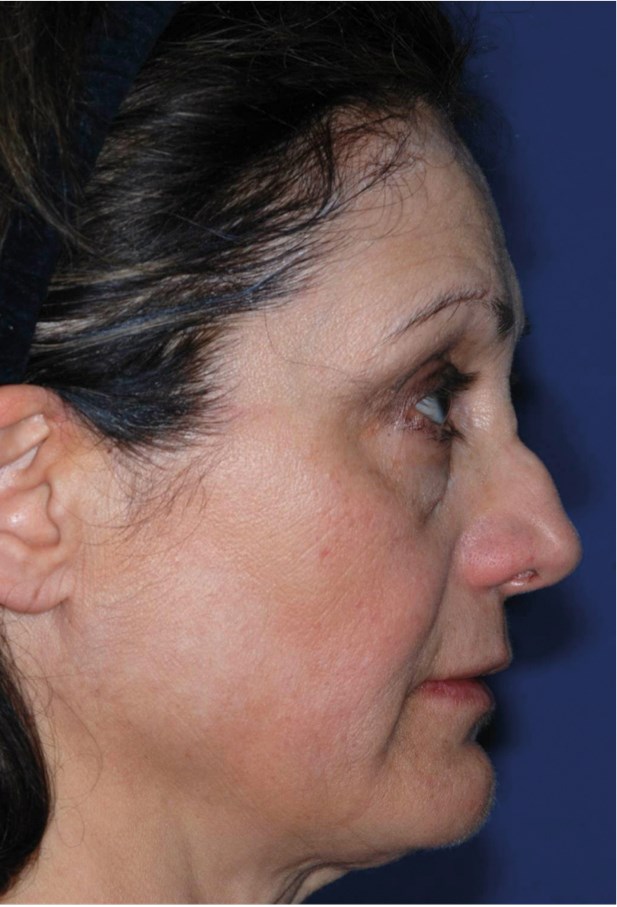
Figure 1: Right profile. Over reduction of nasal bones while the
cartilaginous hump has been left relatively unharmed.
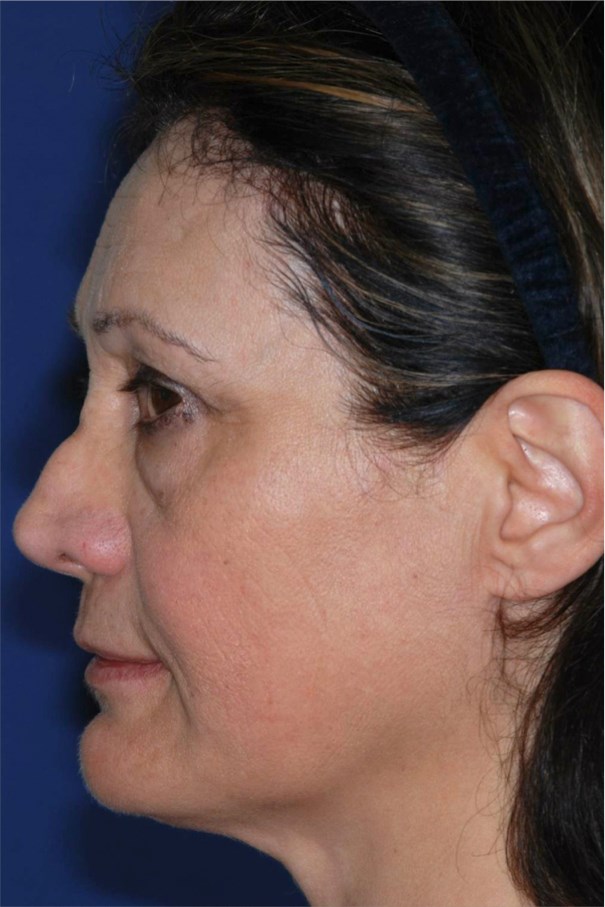
Figure 2: Left profile. A common misconception is thinking of the hump as being made of mostly bone. Often, the hump is overwhelmingly made of cartilage. Loss of the radix-rhinion complex shortens the nose and creates a very unnatural, ‘operated’ appearance.
Case report
In Figures 1 and 2, the typical manifestation of inadequate technique are displayed. Most humps are made of cartilage not bone. Therefore, more cartilage than bone must be removed, otherwise, the entire relationship of the dorsum and radix will be lost, and the hump will be maintained.
To reverse this situation, an endonasal approach was chosen for two good reasons: after a previous rhinoplasty, the healing capacity of the nose may be compromised, and therefore, an external approach would cause unnecessary trauma. Secondly, the ‘business end’ of the operation is at the radix, not the tip. Through a hemitransfixion incision, adequate access to the radix was obtained through a dorsal tunnel. There are several advantages to this approach: the pocket created for receiving the graft is limited in size and position to the midline. This limits the possibility of the graft from intra- and postoperative displacement. As the graft pocket is not contiguous with the intranasal cavity, the risk of low-grade infection and subsequent resorption is minimised.
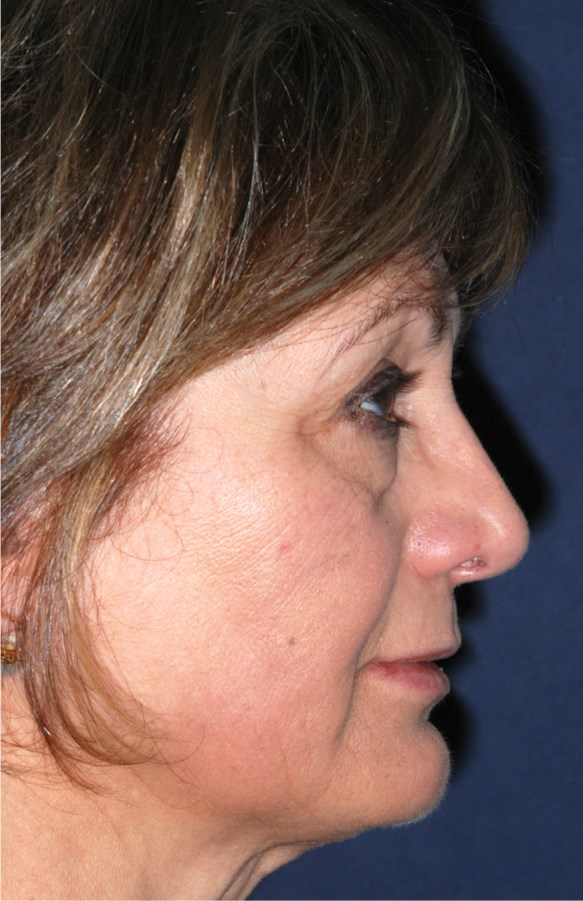
Figure 3: Reconstitution of the radix-rhinion relationship after a conchal cartilage graft restores a natural appearance of the nose. Notice the straight dorsal line that joins the tip to the radix.
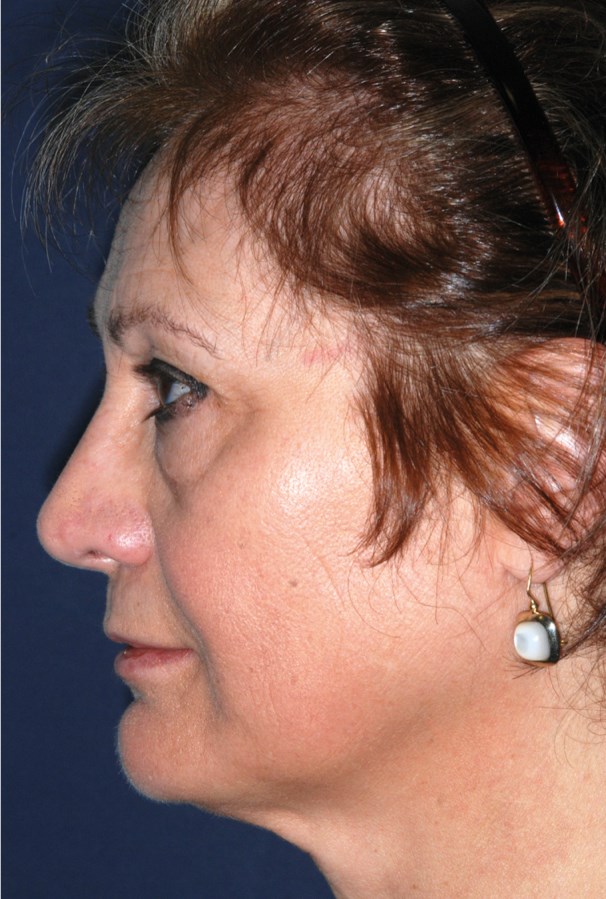
Figure 4: The correct position of the radix can have profound effects on the perception of projection in a ‘see-saw’ effect. Compare the apparent projection in this Figure with Figures 1 and 2.
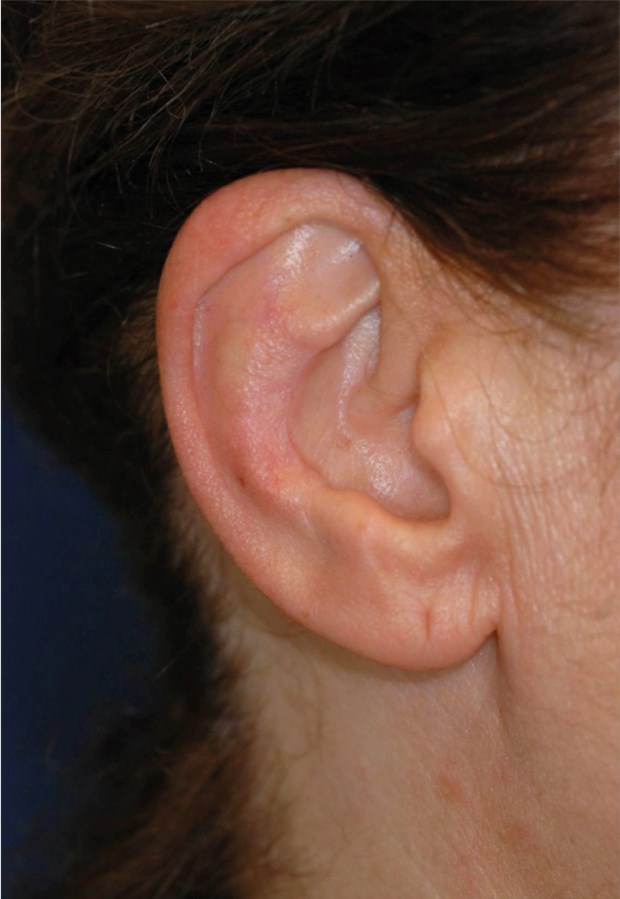
Figure 5: The site of conchal graft harvesting becomes almost totally
invisible within a short few weeks after the operation.
The graft was harvested from the conchal bowl from an anterior approach for ease of access. Septal cartilage represents the first choice, but in this specific case septal cartilage was almost totally removed in previous surgery. Figure 3 displays the inconspicuous scar a few weeks later. The multi-layered graft consists of a deep and intermediate layer of solid cartilage, while the superficial layer was made of cartilage flakes. A sheet of absorbable haemostatic gelatin that prevents graft displacement in the immediate postoperative period covers the graft.
Conclusions
Adequate preoperative planning and correct surgical techniques can prevent disruption of the radix-rhinion complex. This relationship can be re-established using an endonasal approach and autologous cartilage grafting. Septal cartilage represents the first choice. When the septum is missing, the authors resort to ear cartilage.
References
1. Palma P, Khodaei I, Tasman AJ. A guide to the assessment and analysis for the rhinoplasty patient. Facial Plast Surg 2011;27(2):146-59.
2. Steiger JD, Baker SR. Nuances of profile management: the radix. Facial Plast Surg Clin North Am 2009;17(1):15-28.
3. Berkowitz RL, Gruber RP. Management of the nasal dorsum: construction and maintenance of a barrel vault. Clin Plast Surg 2016;43(1):59-72.
4. Fu S, He H, Hou ZG. Learning race from face: a survey. Trans pattern anal Mach intell 2014;36(12):2483-509.
5. Wayne I. Osteotomies in rhinoplasty surgery. Curr Opin Otolaryngol Head Neck Surg 2013;21(4):379-83.
6. Becker DG, Toriumi DM, Gross CW, Tardy ME Jr. Powered instrumentation for dorsal reduction. Facial Plast Surg 1997;13(4):291-7.
We would like to apologise for two errors which appeared in the December/January 2016 How I Do It feature. Please note that Mr Justin Chatterjee is a Consultant Plastic, Reconstructive and Aesthetic Surgeon in Newcastle-upon-Tyne, not Glasgow as the article stated. The contact email was also incorrect, and should have been elitesurgicalltd@gmail.com
COMMENTS ARE WELCOME