Most maxillofacial procedures have an aesthetic element. Reconstructive procedures and surgery to correct congenital abnormalities such as cleft lip have an obvious aesthetic impact. When making surgical incisions for access to the underlying facial skeleton consideration will be made to achieving the most inconspicuous scar. Whilst oncological principles take precedence, aesthetic units are considered when resecting skin tumours.
Few procedures, however, have the potential to change facial appearance as much as those used routinely in orthognathic surgery. Commonly performed jaw osteotomies, such as the Le Fort I maxillary osteotomy and bilateral sagittal split mandibular osteotomy, if planned and carried out appropriately, can produce dramatic aesthetic results.
The aims of orthognathic surgery, which is defined as the treatment of dento-facial deformity, are twofold: firstly, to achieve the best functional dental occlusion and secondly, to give the best aesthetic outcome. Treatment planning determines the jaw movements necessary to achieve a good occlusion but when deciding which jaw to move and by how much account must be taken of the effects of planned movements on facial appearance. Patients neither know nor care whether they have a class 1 molar relationship at completion of treatment but all can look in the mirror and judge their facial appearance. All expect it to be improved or certainly not worsened following surgery.
The word aesthetic means ‘pertaining to beauty’. Beauty, however, is difficult to define. Perceptions of beauty have varied throughout history. The strong nose and chin exemplified by the classical profile would not be considered ideal today. There are also cultural and racial variations in what is considered beautiful. Beauty is clearly in the eye of the beholder, but there are guidelines which must be followed in orthognathic planning to achieve the best results. In common with other forms of aesthetic surgery, planning is based on clinical assessment:
1. Facial balance
This is assessed by measuring reference to facial ‘thirds and fifths’ (Figure 1). Aesthetically pleasing faces have good facial proportions.
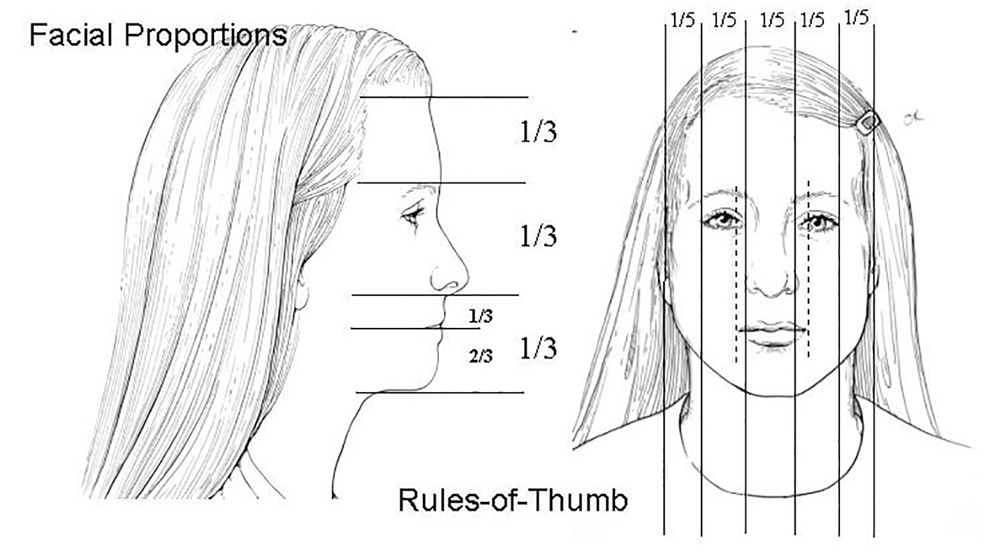
Figure 1.
2. Lip balance
In general the width of the upper and lower lip vermillion should be approximately equal. Width is related to the support given by the related jaw and teeth and can therefore be changed by the appropriate jaw movement. Similarly, anterior-posterior projection of the lips is determined by the position of the jaws and should ideally be equal.
3. Chin-nose balance
The balance between chin and nose is an aesthetic judgement. The perceived size of the nose is related to size of the chin. Patients presenting with concerns related to the size of their nose may be retrognathic, requiring treatment by mandibular advancement or genioplasty rather than reduction rhinoplasty.
4. Nasolabial angle
This varies between 100 and 120 degrees and is greater in females than males. Maxillary movements directly affect nasolabial angle and nostril show. Maxillary advancement and impaction increase nasolabial angle and alar width. In patients with an obtuse nasolabial angle the potential for producing the ‘Miss Piggy’ nose by ill-considered maxillary movements must be taken into account (Figure 2).

Figure 2a.
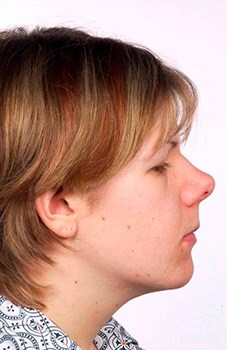
Figure 2b.
5. Cheekbones and inferior orbital rims
Class 3 patients frequently have a degree of pan-midface hypoplasia. This can be corrected by cheek implants which can be simply combined with Le Fort I maxillary advancement (Figure 3).
Figure 3a.
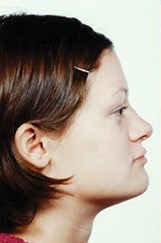
Figure 3b.

Figure 3c.

Figure 3d.
6. Age changes
The facial soft tissue changes which occur with age are well known. Skeletal age changes and their effects on facial morphology are less well recognised but should be taken into account when planning orthognathic surgery. For instance, the upper lip thins and lengthens with age and therefore the amount of upper incisor show with lip at rest decreases. Resorption around the piriform apparture and anterior nasal spine occurs, leading to the nasolabial angle becoming more acute. Dental wear leads to a decrease in the vertical dimension of the lower third of the face. In general, soft tissues should be left well supported by maxillary advancement and vertical changes anticipated by conservative impaction of the maxilla when indicated.
In conclusion, although the primary aim of orthognathic surgery is to provide the patient with a functional dental occlusion, this form of surgery is also a powerful aesthetic tool which can produce dramatic changes in appearance. If the aesthetic outcome is to be optimal and unaesthetic changes are to be avoided it is important that clinicians involved have a thorough understanding of the immediate and long-term consequences of facial bone reconfiguration.
Declaration of competing interests: None declared.




