Chemical peels form an important part of most aesthetic and cosmetic practices. They are an affordable procedure for patients and significant results can be achieved. Generally chemical peels are a safe procedure, but only if used correctly and with caution. Over recent years we have seen a surge in skin peels used in clinics and the range of skin conditions and disorders they can treat is now considerable. As professionals it is important to understand the different types of peels in order to be able to make an informed decision about which one should be used for which patient and how they should be used.
History of chemical peels
Skin peels have a very long history. Early records show that they were used by ancient Egyptians when women used to apply sour milk to their skin. This sour milk contained lactic acid, an alpha hydroxy acid, which rejuvenates the skin. In addition, they used other substances such as animal oils and alabaster to improve the skin’s texture [1].
In Roman times, people were conscious of their skin and would use fruit such as grapes to exfoliate their skin. The active ingredient responsible for the use of grapes was tartaric acid. Other treatments included poultices containing substances such as sulphur, mustard and limestone, which were used to fade freckles and to even the skin. These ancient records show us that skin care has been important, particularly to women, through much of history. In 1874, a dermatologist in Vienna called Ferdinand von Hebra, used peeling techniques to treat pigmentation conditions such as melasma, freckles and Addison’s disease. In 1882 in Germany, Paul G Unna described the use of salicylic acid, resorcinol, trichloroacetic acid (TCA) and phenol on the skin. It was following his reports that other authors started publishing their work [1,2,3].
In 1917, during World War I, Douglass Montgomery made reference to his use of phenol under bandages for healing and ‘beautifying’ the skin [1]. However it was not until 1952 that George MacKee published his results in England, using phenol for the treatment of scarring. Interestingly, despite this publication date, he had actually been using phenol peels since 1903 [4]. It is not surprising that these doctors used phenol in the early days of skin peels, particularly in patients with scarring, as in current day practice this is classed as a ‘deep peel’.
The use of chemical peels really started to gain momentum in the 1960s as modified solutions of phenol were developed and histological assessment comparisons were drawn between phenol and TCA. Scientific work continued into the 70s and 80s and at the same time, the use of alpha hydroxy acids (AHAs) was developed by Van Scott and Yu for more superficial treatment [3].
Different types of chemical peels
Chemical peels are a means of rejuvenating the skin by removing the keratin layer of dead skin cells that sits on the skin’s epidermal surface and also by stimulating the production of new healthy epidermal cells. They are designed to introduce a controlled injury to the skin to a specific depth. As the healing occurs there will be an improvement in the skin’s texture and appearance. This technique stimulates epidermal growth, with collagen stimulation in the underlying dermis, giving a tightening effect and a more even distribution of melanin [5].
Skin peels are classified by their depth of penetration. They are divided into three categories: superficial, medium and deep peels. The depth to which each specific peel penetrates when applied to the skin affects the clinical outcomes achieved. Not surprisingly, the deeper the penetration of the peel, the greater the changes achieved. However, the depth of peel also represents the amount of injury caused to the skin and so will have an effect on the length of downtime, or ‘healing time’. Hence increasing depth will increase the risk of possible complications.
Superficial peels
Superficial peels are the ‘lightest’ peels and are really the only type of peel that can be used as a ‘lunchtime peel’. As they are so superficial there is rarely any downtime as a result of the treatment. These peels only penetrate into the epidermis, are similar to a good exfoliation, giving an instant brightening and smoothing of the skin. Light chemical peels are suitable for those with mild sun damage with pigmentation, mild acne scarring, dry skin, post inflammatory pigmentation, very fine lines and wrinkles and ‘dull’ skin. These are a great introduction into skin peels, particularly for patients who are new into aesthetics and are quite nervous. Discomfort during the treatment is unlikely although some patients may experience some mild stinging or tingling to the skin. As stated above, downtime after a superficial peel is minimal, and some patients (not all) may experience light shedding of the skin for three to five days which is usually well accepted. The beauty of a superficial peel is that normal life can continue almost immediately and any light shedding can usually be disguised with make-up.
Superficial skin peels tend to be made from AHAs or beta hydroxy acids (BHAs). AHAs originate from milk and fruit sugars, the most commonly used are glycolic and lactic acid. These acids penetrate the skin well and have significant scientific research to support their efficacy. Other AHAs that are starting to feature more in chemical peels as these treatments evolve are malic, citric and tartaric acid [6]. BHAs such as salicylic acid, have been used for some time and seem to be used less, as the growth of peeling with AHAs develops [3]. A study comparing both AHA and BHA in the treatment of acne vulgaris was reported by Kesseler in 2008, and showed that both were effective [7].
“As aesthetic practitioners it is important that we really understand what a patient is hoping to achieve from their skin peel and that we are able to inform them of all the options available.”
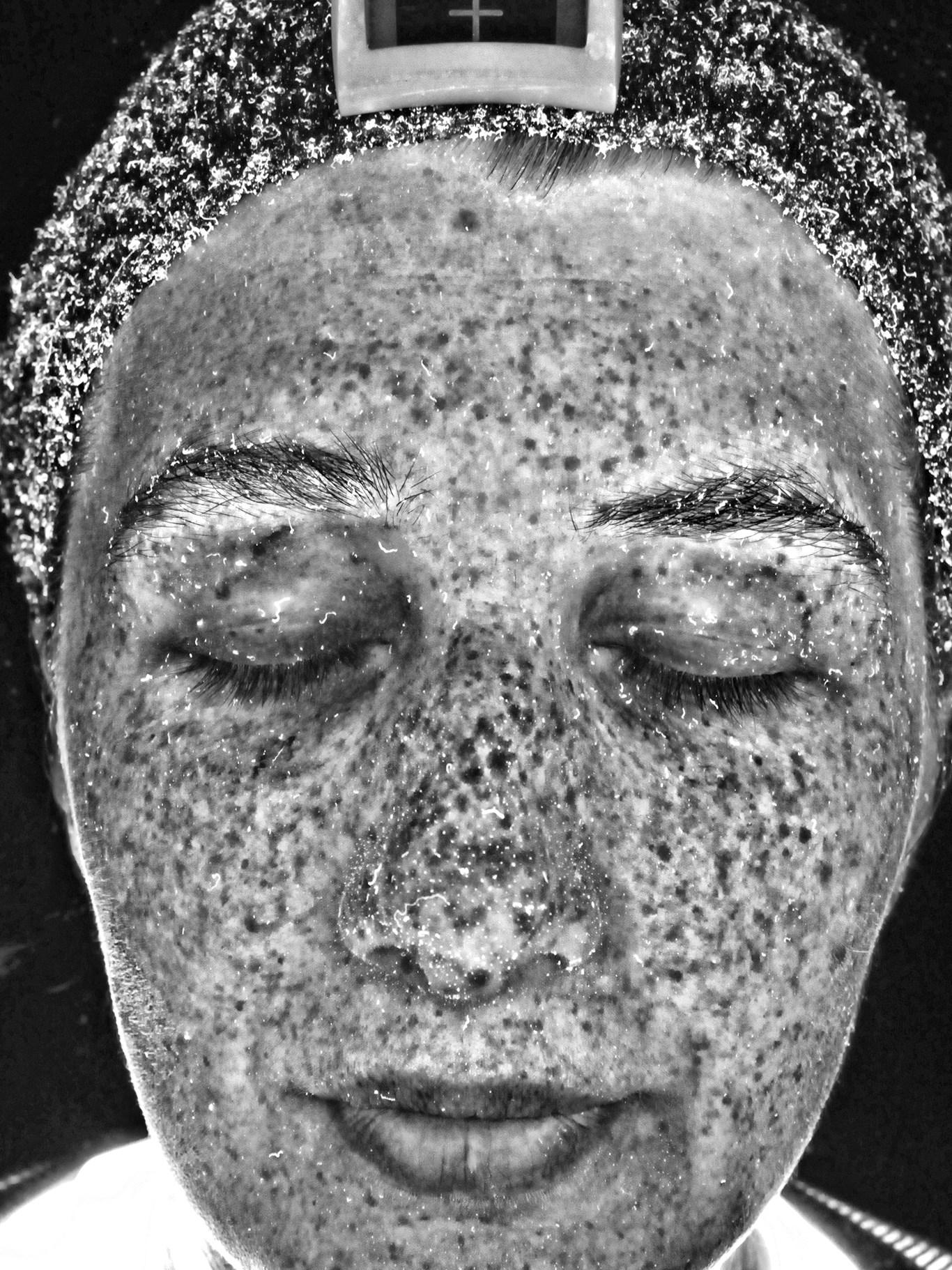
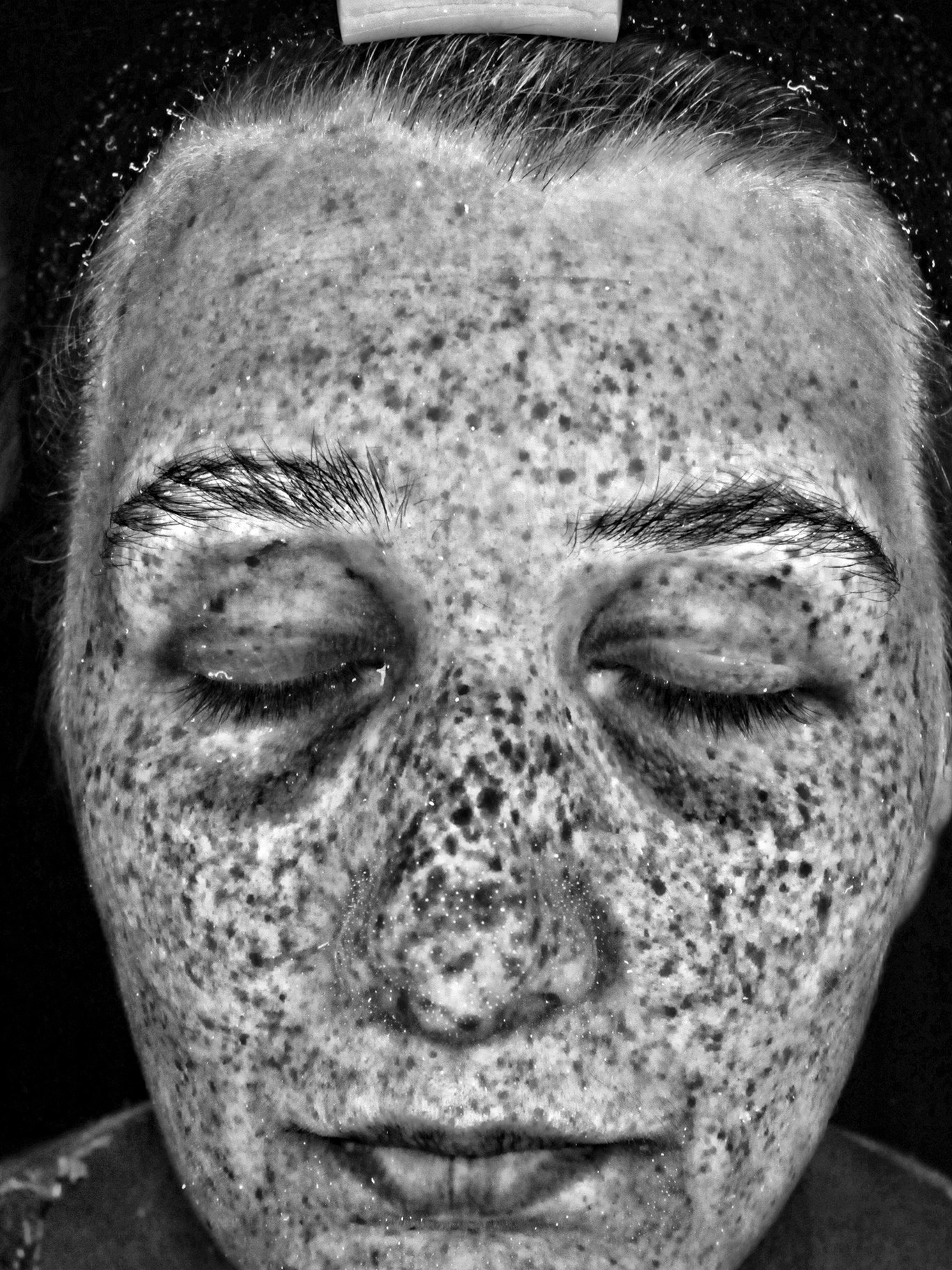
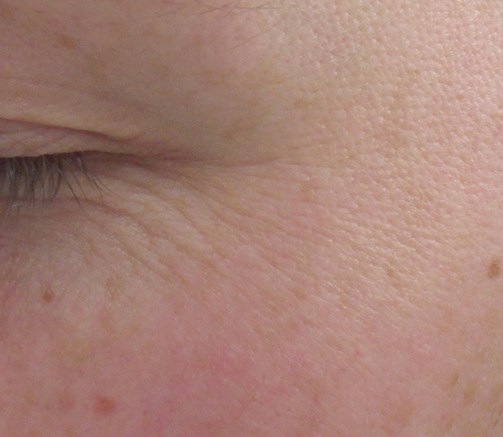
Top: Before. Bottom: After.
Before.
After.
Medium peels
Medium depth peels, such as TCA, are used as a stand-alone treatment or as part of a combined or blended peel, e.g. Jessner or modified Jessner peel. TCA is used in various strengths. Those less than 20% work well on superficial lines and wrinkles but not so successfully on deeper lines or scars, whereas TCA greater than 25% can cause deep epidermal necrosis increasing the potential of complications. Even more concentrated, TCA 35-50% is one of the more commonly used peels for the treatment of actinic keratosis, pigmentation and severe photoageing [5,8,9].
The depth reached by TCA peels is affected by a number of factors:
- The type of skin (thicker skin can tolerate the higher concentrations).
- The strength of the TCA (15-20% penetrates only the epidermis, 45% penetrates the upper reticular dermis).
- The combined use of retinoic acid (0.025%-0.1%) enhances penetration and results.
- Cleansing the skin before application with an active cleansing substance or mild cleanser affects the aggressiveness of the peel.
- Lower concentrations of TCA can be used if blended with other active agents with the aim of giving the same results whilst reducing the risks of complications.
Blended peels tend to be used for treating mild sun damage, acne and acne scarring. It is possible to get the desired results with these peels but, as they are less aggressive than TCA alone, there is less recovery time or shedding of the skin [9]. There are many different blends available, such as TCA with glycolic, salicylic and / or lactic acid, and mixtures will vary with each manufacturer. By combining the acids together, the concentration of the acids is reduced and so the toxicity levels are lower [5,8].
Medium depth peels work successfully on fine lines and wrinkles, solar lentigo, scarring (acne or following a trauma), irregularities of skin texture and pigmentation disorders. When applied to the skin, these agents penetrate sufficiently to destroy the epidermis and part, or all, of the papillary dermis. The healing process following a medium peel such as TCA is approximately one week, although this will vary with the strength of TCA used, how much is applied and how long it is left on for.
TCA peels should be used with caution in dark skin patients as they have been known to cause post inflammatory pigmentation or scarring [5].
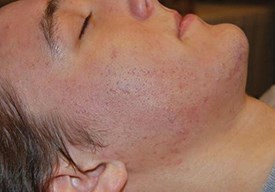
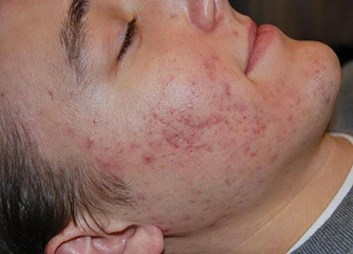
Top: Before. Bottom: After.
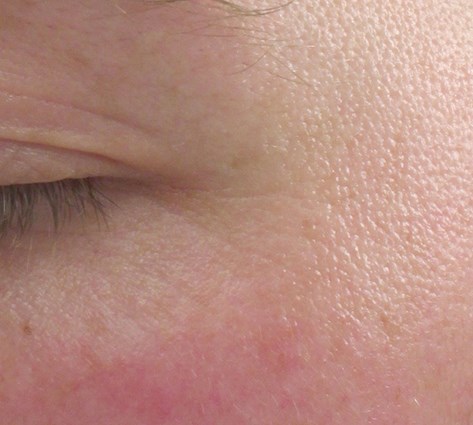
Top: Before. Bottom: After.
Deep peels
Deep peels are used less commonly nowadays. This might be because they cannot be performed within a typical aesthetic clinic environment as they require sedation or anaesthetic. Also the continuous development of superficial and medium peels, and the practice of having more and more frequent treatments, means that patients can get the desired results without the downtime that is associated with deeper peels. Despite this, there is still a need for deep peels as some patients are not going to be able to achieve their optimum result with lighter alternatives and some patients are happy to have the associated increased downtime.
Deep peels are suitable for those who have severe photo-ageing, deep or heavy wrinkles and scarring. Phenol is usually used in combination with croton oil in various concentrations and once applied, it penetrates to the dermis and even the reticular dermis, maximising the effect for new collagen production. After a phenol peel the epithelial layer takes about 5-10 days to form but, unlike many of the lighter peels that are applied and removed, the phenol peel requires a mask to be placed on the skin for approximately 24 hours and various antiseptic ointments and occlusive dressings are required in addition to antibiotics to prevent infection. It can take up to three months for healing to be complete and the final result to be seen [8].
As phenol is absorbed into the circulation, it increases the risk of cardiotoxicity in the form of arrhythmias. As a result cardiopulmonary monitoring is required, as is intravenous hydration. As such, these peels are performed in a hospital environment, commonly in an operating theatre, and often as an addition to other surgical procedures [5].
Phenol is an aromatic hydrocarbon derived from coal tar. Croton oil is a plant seed extract (Croton tiglium) and has been used commercially since 1932 and when used on the skin causes skin vesiculation [10].
Dark skinned patients are not recommended to have deep skin peels due to the increased risk of permanent pigmentation changes after treatment, so other options, such as laser resurfacing, have become popular as alternatives to avoid the adverse effects.
Who is suitable for a peel and who is not?
A typical chemical peel patient comes to a clinic because they want to improve or enhance the look of their skin. As many people have different thoughts on what they want, the consultation process is particularly important to ascertain what the patient wants and wishes to achieve. As most people want ‘healthy skin’ we have to know what is classified as ‘healthy’ skin.
Generally healthy skin:
- Is smooth – with even keratinisation.
- Is firm – with good collagen and elastin production.
- Is even in colour.
- Is hydrated.
- Has no damage as a result of environmental exposure or medical conditions, e.g. sun damage, acne.
- Is able to heal quickly and effectively – efficient healing and repair response after injury.
- Has good circulation.
As aesthetic practitioners it is important that we really understand what a patient is hoping to achieve from their skin peel and that we are able to inform them of all the options available. Peels are a popular treatment and, when used correctly, the results can be very pleasing. Understanding the different ingredients, the effect they have on the skin during and post treatment and how they should be used is key. Patients should have a thorough consultation and skin analysis before treatment where all this information is discussed, so they can schedule the treatment into their life and have realistic expectations of what can be achieved. The depth and type of peel chosen to treat the patient is dependent on their skin type and skin disorder being treated. Some of the treatable skin disorders and concerns include [11,12]:
- Photo damage and pigmentation.
- Anti-ageing.
- Reducing the appearance of lines and wrinkles.
- Improve skin tone and texture.
- Lighter, brighter skin.
- Open pores.
- Acne and acne scarring.
- Stimulating cell renewal.
- Renewal of the skin’s structure, e.g. collagen and elastin.
Side-effects and possible complications should also be discussed and taking images of the skin pre and post treatment gives a good baseline for future comparison. Having photographic evidence is also helpful both to see what results have been achieved as well as being of use if a complication should arise.
The risks of complications should be minimised with:
- A thorough consultation including a good discussion and choice of appropriate peel.
- Good clinical practice in preparing the skin for peeling.
- Good application of the peel.
- Supporting the patient with the appropriate aftercare advice.
However, if complications do occur, as will inevitably happen, it is essential that you are able to support and manage the patient through that difficult time. The kind of complications that may occur include: blistering, post inflammatory hyperpigmentation (which is a risk for ethnic skin types), herpes simplex, acne or breakouts of spots [11].
Aftercare
After a chemical peel it is likely the patient may experience some erythema, oedema and skin shedding for a number of days. The application of a sun protection factor (SPF) 30-50 cream worn daily and avoiding direct sunlight is standard until the skin has recovered completely. This also maintains the results and so it is good practice to continue. Some peels come with a product range that needs to be applied afterwards to optimise the results, and the aftercare instructions will vary depending on the depth of peel and the peel range used. Ideally patients should be given this information verbally and also in written form to ensure that the patient has understood the instructions.
Summary
Skin peels can work very well as a stand-alone treatment. Over the last few years there has been more focus on the use of combination treatments such as combining skin peels with active product ranges, microdermabrasion, skin needling and laser-based treatments.
Although chemical peels are becoming increasingly popular in aesthetic and cosmetic clinics, they do damage the skin and are a medical procedure and hence adequate medical supervision is required to ensure the patient’s safety. Clearly this is more applicable for the medium to deep peels, but when exploring the range and levels of peels to introduce into your clinic, you should be advised by the supplier / trainer as to the supervision and support that might be necessary, particularly if complications arise. There are many ranges of skin peels available, and by doing thorough research as to what is available and by talking to the companies that provide them, you will be able to find a range that works for you and your clinic.
References
1. Brody HJ, Monheit GD, Resnik SS, Alt TH. A history of chemical peeling. Dermatol Surg 2000;26:405-9.
2. Bryan CP. Ancient Egyptian Medicine: The Papyrus Ebers [translation]. Chicago, USA; Ares Publishers; 1974:158-61.
3. Fischer TC, Perosino E, Poli F, et al. Chemical peels in aesthetic dermatology: an update 2009. J Eur Acad Dermatol Venereol 2010;24(3):281-92.
4. MacKee GM, Karp FL. The treatment of post-acne scars with phenol. Br J Dermatol 1952;64(12):456-9.
5. Rendon MI, Berson DS, Cohen JL, et al. Evidence and considerations in the application of chemical peels in skin disorders and aesthetic resurfacing. J Clin Aesthet Dermatol 2010;3(7):32-43.
6. http://www.glycolicacid.com/
alpha-hydroxy-acid.html
Accessed June 2016.
7. Kessler E, Flanagan K, Chia C, et al. Comparison of alpha- and beta-hydroxy acid chemical peels in the treatment of mild to moderately severe facial acne vulgaris. Dematol Surg 2008;34(1):45-50.
8. Bowes L. An introduction to superficial, medium, deep and combination chemical peels. Journal of Aesthetic Nursing 2013;2(5):224-30.
9. Camacho FM. Medium-depth and deep chemical peels. Journal of Cosmetic Dermatology 2005;4(2):117-28.
10. Landau M. Chemical peels. Clinic in Dermatology 2008;26(2):200-8.
11. Zanna N. Maximising treatment outcomes with skin peels: products, preparation and procedures. Journal of Aesthetic Nursing 2015;4(4):173-80.
12. Small R. A Practical Guide to Chemical Peels, Microdermabrasion & Topical Products. Philadelphia, USA; Lippincott Williams & Wilkins; 2013.
Acknowledgement:
All images are courtesy of Temple Medical, Aberdeen
Declaration of competing interests: None declared.
COMMENTS ARE WELCOME