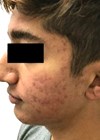
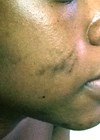
Melasma and post-inflammatory hyperpigmentation (PIH) are among the most common skin disorders in society with prevalence of up to 50% in some populations. Melasma is more prevalent among females and also among those with darker skin types III–V on the Fitzpatrick scale.
The aetiology of melasma remains unknown, however, sun exposure, pregnancy, and use of oral contraceptives are well-known triggers. It is believed that the development of melasma is influenced by many factors including hormones and genetics.
PIH is an increasingly common acquired disorder that follows endogenous inflammation of the skin or other injury. One study found the incidence of PIH in acne patients with skin of colour to be 65.3% among African-Americans, 52.7% among Hispanics and 47.4% among Asians [1]. These disorders can cause significant psychosocial distress and a marked reduction in the quality of life of those affected.
Melasma and PIH are hard to treat and treatment protocols involve vigilance against environmental triggers, high daily sun protection, as well as topical agents such as hydroquinone or systemic agents such as tranexamic acid. More recently other modalities such as lasers, micro-needling, and chemical peels have been used with varying levels of success. In my practice I have begun to use a new short-pulsed Nd:YAG laser called the Aerolase Neo Elite (Aerolase Inc., Tarrytown, NY, USA).
Patient selection and preparation
One of the key benefits of the Neo Elite is that it is safe and effective on all skin phototypes due to the very short, 650ms pulse, so I can use it safely on most patient cohorts. Preparation is key and I am vigilant in ensuring the area to be treated is not sunburnt and does not have any other irritation. If a patient is taking photo-sensitising medication, such as Accutane, I recommend they consult with their dermatologist before embarking on treatment. I also ask my patients to stop using topical retinols at least 72 hours before treatment and I will not use this technology on patients who suffer from lupus or other light sensitive autoimmune disorders.
Treatment
Prior to treatment I thoroughly clean the target area and closely assess the patient’s skin to ascertain their phototype, skin quality, hydration and pigment, as this will influence the settings used on the laser and what changes may be expected.
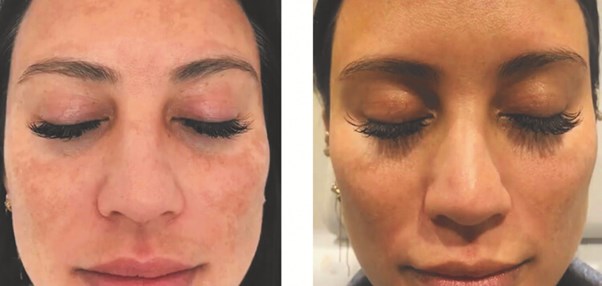
Patient with melasma – before and after treatment with four sessions
with Aerolase and one light peel (courtesy of Dr Roberta Del Campo MD).
For all patients I set the device at 650ms pulse and use a 6mm lens with a collimated beam profile. For my patients with skin phototypes I-III the device is set to an energy level between 6 and 8 which is a fluence of 21-28J/cm2. For my patients with skin phototypes IV-VI I use a lower energy setting; typically mode 3-6 which is a fluence of 11-21J/cm2.
I perform five to six passes of non-overlapping pulses over the treatment area; my endpoint is seeing a change in colour of the affected area, either a darkening (deep pigment) or lightening (superficial pigment) depending on the depth of the pigmentation. I advise my patients that the treated area may appear darker for two to three weeks after the treatment but will fade naturally.This process can be speeded up by including a superficial or very superficial chemical peel immediately after each laser treatment. A complete treatment will involve three to five sessions spaced three to four weeks apart.
Post-treatment care
I advise my patients that they may return to normal activities immediately after treatment with the recommendation to use a broad spectrum UVA / UVB sunscreen (minimum SPF 30) and / or physical sun-blocking measures (hat, sunglasses).
A good skincare regimen is most certainly an essential complement to this treatment so I will always recommend the use of appropriate skincare products to enhance the results.
Reference
1. Taylor SC, Cook-Bolden F, Rahman Z, Strachan D. Acne Vulgaris in skin of color. J Am Acad Dermatol 2002;46(2):S106.
Declaration of competing interests: None declared.
COMMENTS ARE WELCOME