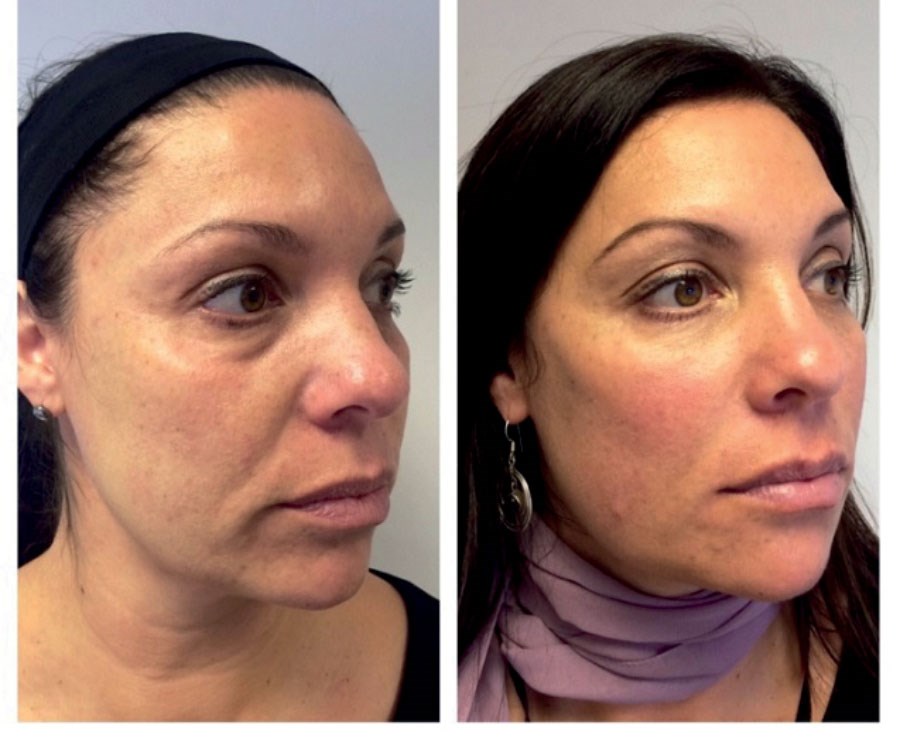
The peri-orbital region is the first to show signs of ageing due to thin skin and changes in texture, colour and volume. This can make the eyes look tired or sunken which can have a negative impact on the global aesthetic. In this article I will explore the anatomical basis and aetiology of peri-orbital ageing. In particular we shall highlight the changes occurring in the facial skeleton, fat compartments, musculature and skin.
Understanding the pathology allows us to generate a treatment protocol in keeping with the most effective sequence of treatments at the correct injection sites in order to generate tissue lift and support. Effective treatment of this area can produce impactful results associated with high levels of patient satisfaction.
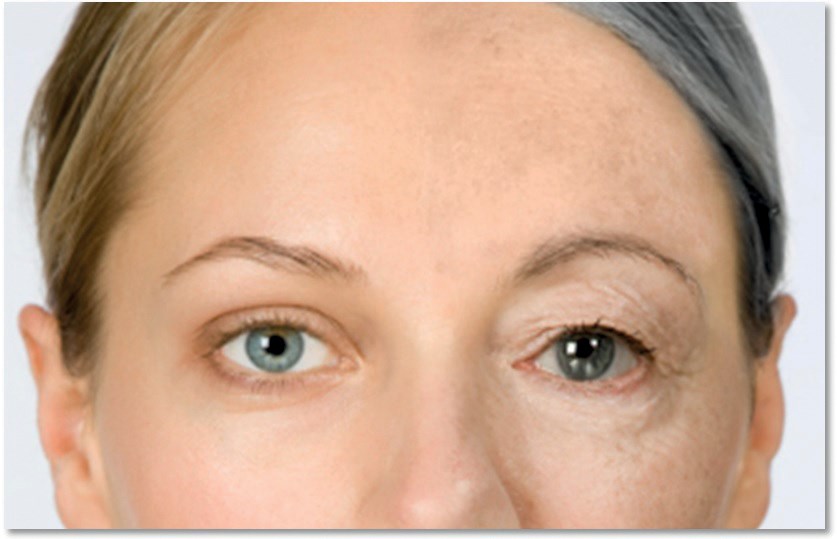
Figure 1.
Peri-orbital ageing
During ageing of the peri-orbital region we observe the following changes when considering the tissue layers from superficial to deep (see Figure 1):
- Skin – atrophy, laxity, sagging and excess due to photo damage related loss of collagen and elastin.
- Fat – peri-orbital and mid-facial lipo-atrophy resulting in deflation and subsequent inferior migration of the fat compartments.
- Muscle – hypertonicity and hypertrophy of orbicularis oculi and the glabellar complex which exacerbates brow descent.
- Bone – frontal, orbital and zygomatic resorption and remodelling which compromises soft tissue support in the anterior, lateral and vertical planes.
The combination of these age-related changes results in the following symptoms:
- Elongation of the forehead and frontal lines
- Brow descent and loss of angulation apex
- Skin excess and hooding of the lateral upper eyelid
- Descent of the lateral canthus and ‘sad eyes’
- Deepening of the infraorbital crease and tear trough
- Elongation of the lid / cheek junction
- Scleral show +/- ectropion.
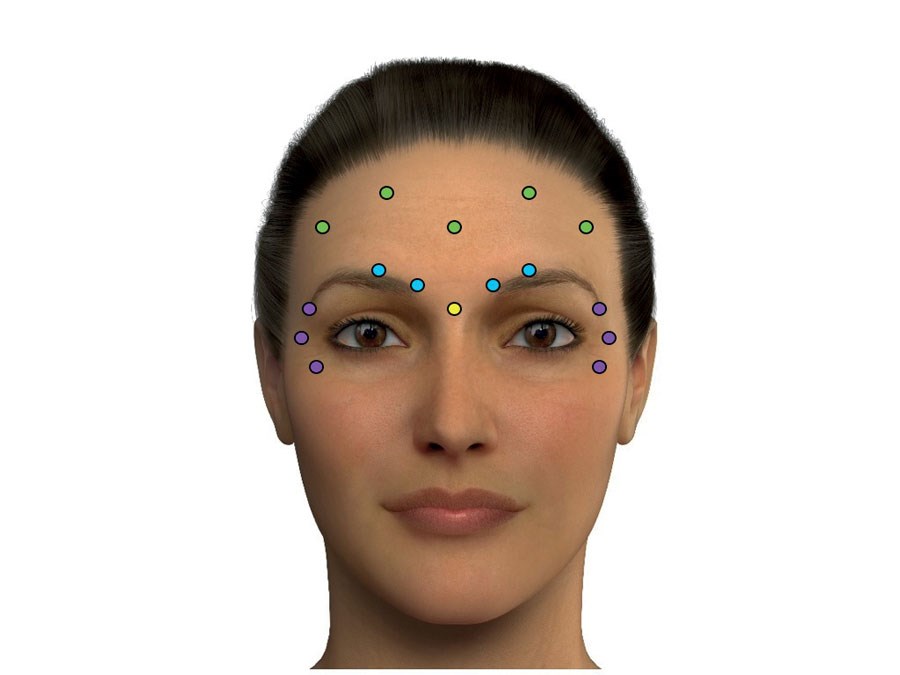
Figure 2.
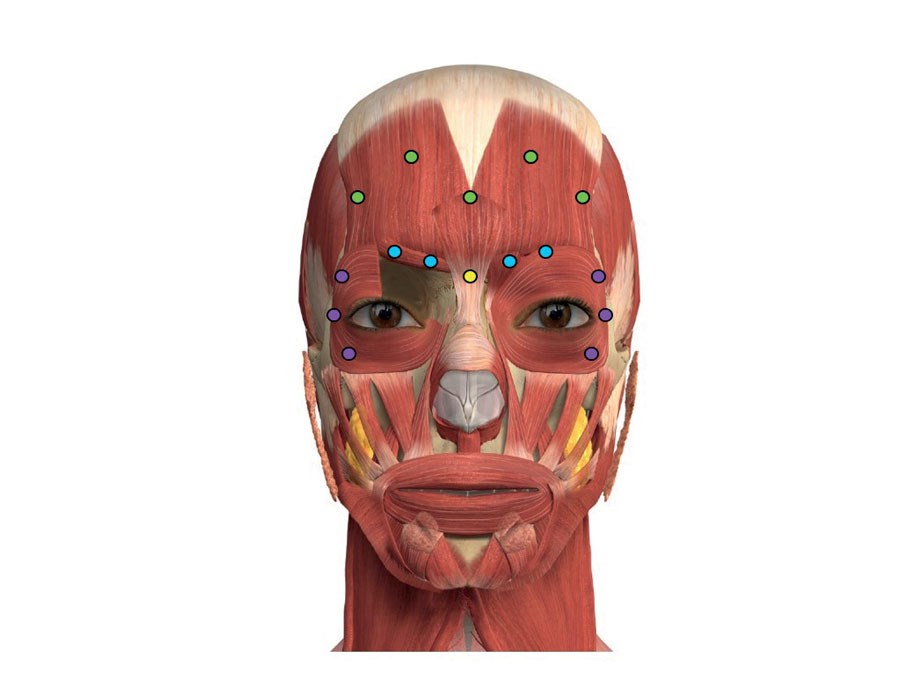
Figure 3.
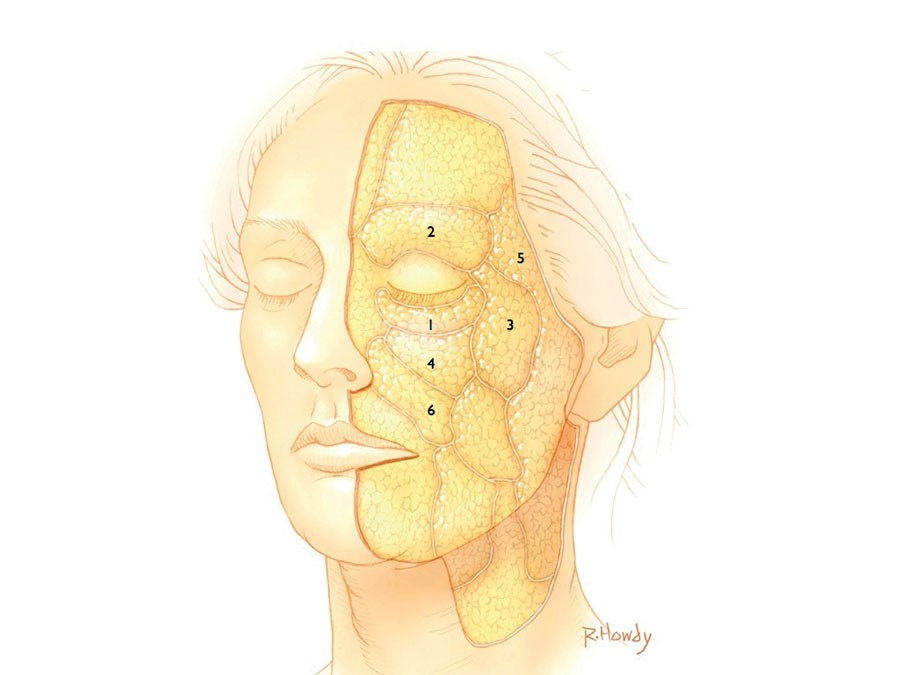
Figure 4.
Anatomy
Muscles
Upper facial muscle balance is influenced by the relative power of depressor vs. elevator activity and can be adjusted to optimise the beauty of the eyebrow and peri-orbital frame. In order to facilitate a more open orbital aperture we can use Botulinum toxin to selectively weaken upper facial depressors, whilst tempering the effect of frontalis and influencing brow position and shape. These injections should typically take place two weeks prior to hyaluronic acid (HA filler) in order to optimise lifting capacity (see Figures 2 and 3):
- Procerus – 2-4U deep (vertical injection).
- Corrugator – 4U deep medially and 2-4U SC laterally (oblique injection).
- Frontalis – 1-2U deep medially and superficial laterally (vertical injection).
- Orbicularis oculi – 2-4U intradermally and orientated away from the eye.
Fat compartments
In 2007, Rohrich and Pessa assessed 30 hemifacial dissections following injection of methylene blue dye into facial fat. The findings concluded that the subcutaneous fat is divided into discrete fat compartments separated by septi or ‘retaining ligaments’. The sequence in which these compartments change in volume and position with age was found to be an important factor in assessing and treating facial deflation and subsequent descent. These changes result in the closure or inversion of the orbital aperture, degrading the beauty and youthfulness of the eye.
The sequence that we observe age-related volume loss and dehiscence between facial fat compartments can be summarised as follows (see Figure 4):
- Anterior herniation of the infraorbital fat into the lower eyelid and held by the orbicularis retaining ligament. This leads to the appearance of ‘eye bags’ and deterioration of the tear trough deformity.
- Dehiscence and descent of the retro-orbicularis oculi fat (ROOF) into the lateral upper eyelid causing heaviness and skin excess.
- Atrophy of the lateral malar fat compartment without ptosis associated with reduced projection at the Ogee curve and lateral canthal descent.
- Deflation of the sub-orbicularis oculi fat (SOOF) and descent of the medial malar fat compartment worsening the tear trough and lid-cheek junction.
- Deflation of the temporo-buccal fat with mild lateral cheek descent.
- Infero-medial descent of the nasolabial fat compartment resulting in deepening of the naso-jugal groove and nasolabial fold.
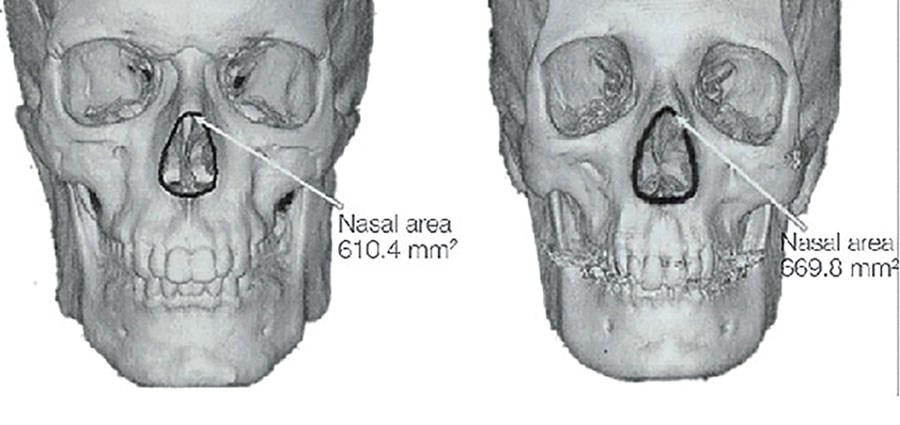
Figure 5.
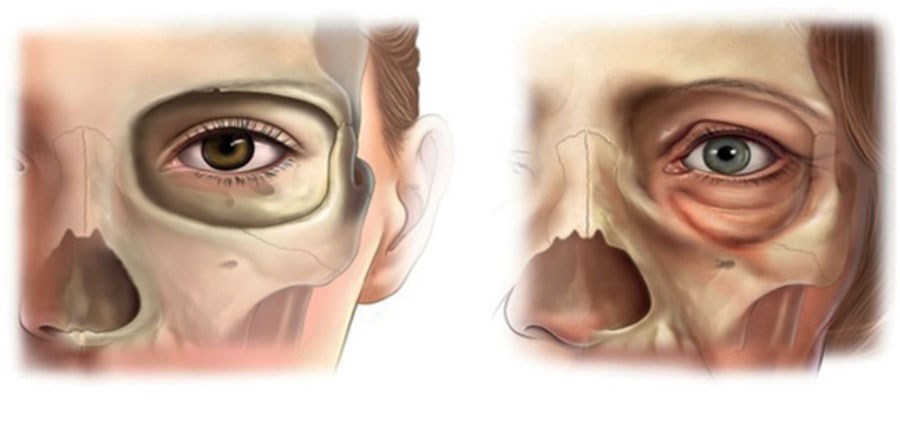
Figure 6.
Facial skeleton
During ageing there is a significant effect on bone density and remodeling (Figure 5). In the facial skeleton we can observe these changes in the transverse, vertical and anterior projection of the bony landmarks
as follows:
- Loss of the youthful convexity of the frontal skull, reducing support of the frontalis muscle and forehead skin causing elongation.
- Temporal hollowing and narrowing of the bi-temporal width associated with collapse of the lateral eyebrow.
- Orbital remodeling, flattening and oliquity of the orbital floor corresponding to the tear trough, lid-cheek junction and lateral canthal descent (Figure 6).
- Reduced projection of the zygomatic arch and maxilla exacerbating mid-facial deflation and descent of soft tissue.
Age-related orbital remodeling is associated with three principle presentations:
- Infero-lateral loss with deepening of the lateral lid cheek junction and lateral canthal descent.
- Infero-medial loss with exacerbation of the tear trough deformity.
- Supero-medial loss with hollowing of the medial upper eyelid in old age.
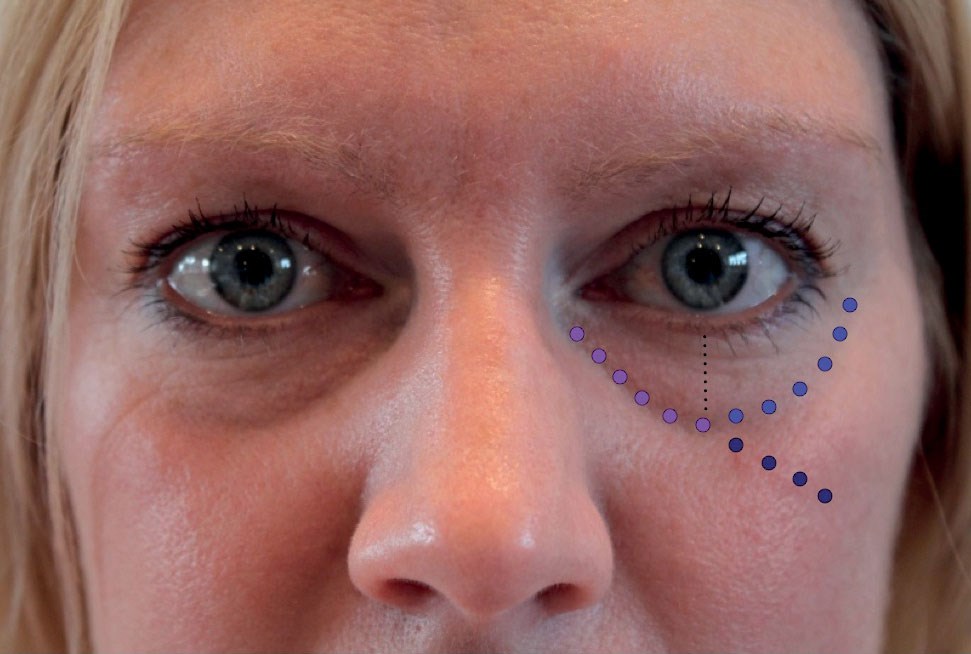
Figure 7.
Clinical presentation
The culmination of changes in the skin, muscle, fat and bone lead to an infraorbital complex deformity (Figure 7):
- Anatomical tear trough – from the medial canthus to the mid-pupillary line corresponding to the cutaneous insertion of the orbicularis retaining ligament.
- Lateral lid cheek junction – from the lateral canthus to the mid pupillary line. The deepest part of the infraorbital crease usually corresponding to the mid-pupillary line.
- Malar groove – inferolateral extension of the tear trough beyond the lid / cheek junction and corresponding to the cutaneous insertion of the zygomatic retaining ligament.
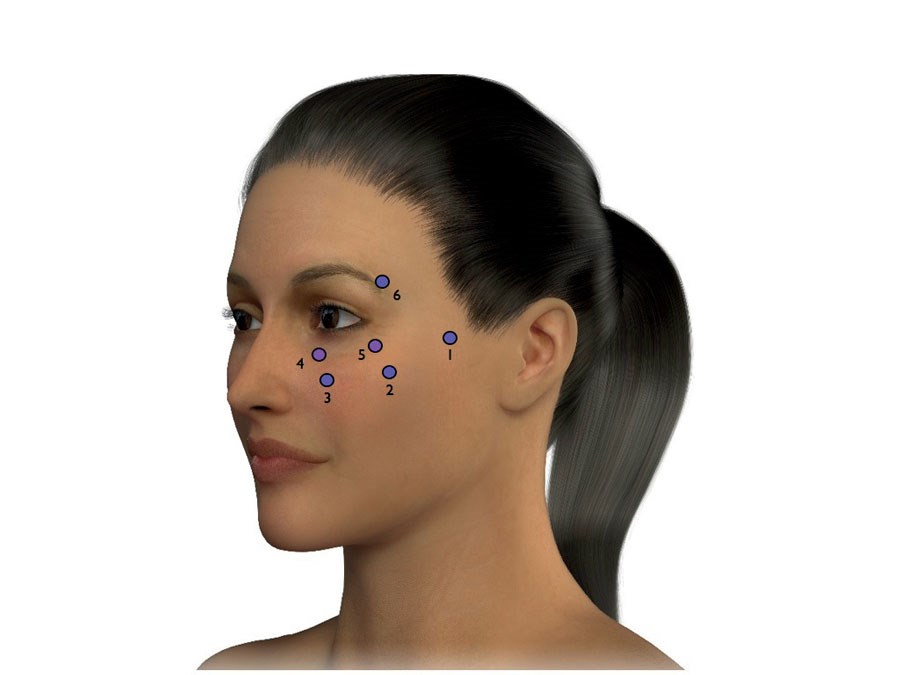
Figure 8.
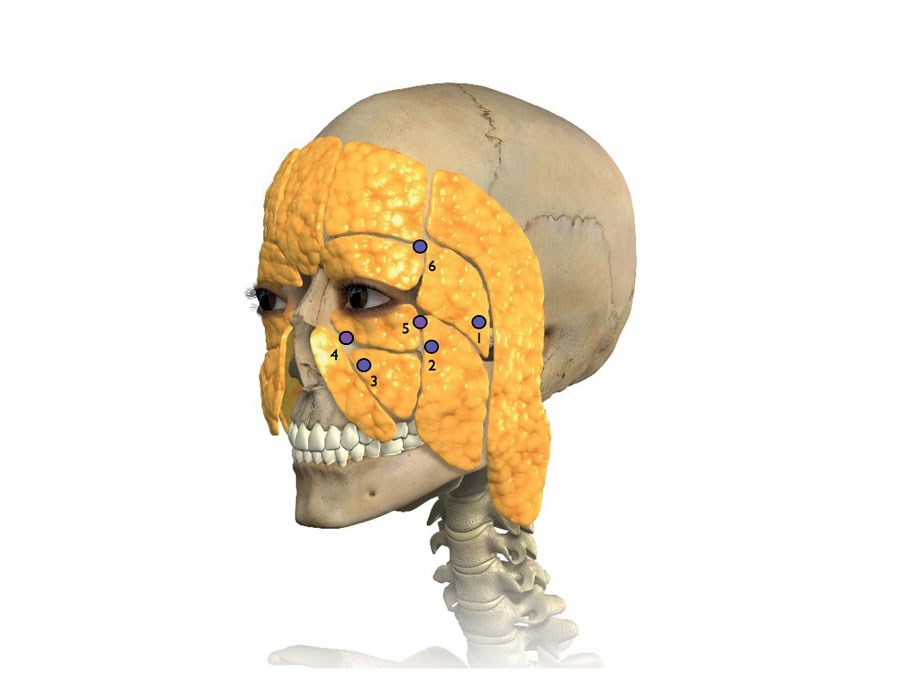
Figure 9.
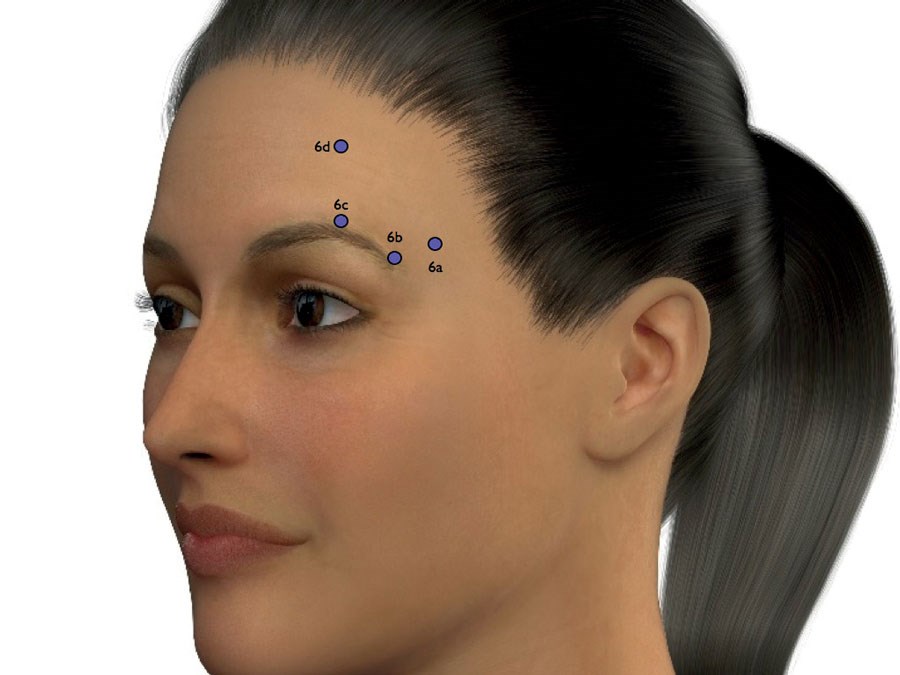
Figure 10.
Six point peri-orbital injection strategy
Two weeks after botulinum toxin injected (as above) the upper facial depressor muscles should be hypotonic and amenable to soft tissue lifting with HA injection as follows (Figures 8 and 9):
- Lateral malar fat compartment – to promote superolateral lift and improve surface tension of the mid-face.
- Beautification point (intersection of upper alar / tragus line with lateral brow line) to optimise convexity and projection at oblique Ogee curve. This point also indirectly improves the lateral lid cheek junction.
- Malar groove – to correct depression and promote anterior projection and vertical lift of the medial cheek. This point also improves the tear trough indirectly through volumetry of the SOOF.
- Anatomical tear trough – low volume injection on the medial infraorbital rim using a low molecular weight (LMW) HA.
- Lateral lid cheek junction – tiny depots of LMW HA injected on the lateral infraorbital rim to promote support to the lateral canthus.
- Brow lift complex – can be divided into the following sequence of injections to give structural support and lift to the eyebrow (Figure 10):
- Temporal fossa – volumetric correction under the deep temporal fascia gives supero-lateral lift to the tail of the eyebrow.
- Lateral eyebrow – injection into the lateral ROOF.
- Eyebrow apex – injection into the ROOF at the PHI point located 0.618 from the medial end.
- Forehead – serial micro depot injection into the deepest frontal lines in the sub galeal plane for vertical support of the eyebrow.
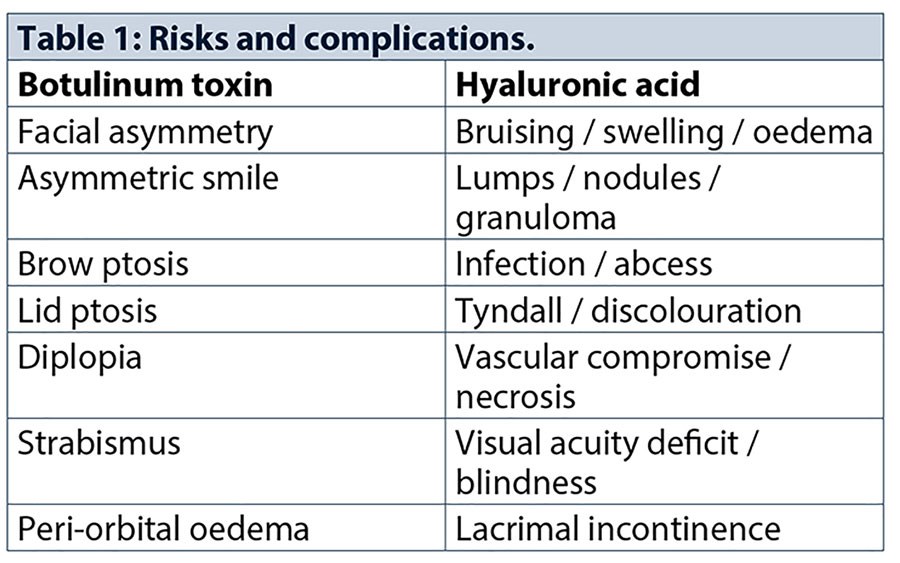
Risks and complications
Adverse events can be minimised by selecting the correct patient, product, dosage, placement and administered by the appropriate person in a suitable environment using an aseptic technique. Effective treatment planning and executing a robust protocol can help to reduce risks and complications.
Conclusions
Recent advancements through rigorous scientific study and development have culminated in a deeper and more cultivated understanding of peri-orbital ageing and rejuventation. We now have the knowledge and tools to deliver exceptional products using the most sophisticated techniques. These non-surgical interventions have never been more effective in influencing muscle, fat compartments, retaining ligaments, surface tension and genuine tissue lift. Furthermore, new generation low molecular weight HA fillers with exceptional tissue integration are able to deliver soft and natural results during repose and facial animation. Through ongoing refinement of the art and science of facial aesthetics, our results can only improve and surpass the expectations of our patients, raising the bar in our industry and promoting excellence as a prerequisite standard.
Case study
A 43-year-old patient with Juvederm Voluma 0.2ml injected at points 1 and 2, Juvederm Volift 0.05ml injected into the SOOF at point 3 and Juvederm Volbella 0.3ml injected into points 4 and 5. The eyebrow was contoured using 0.4ml Juvederm Voluma in the temporal fossa and 3 x 0.1ml Juvederm Volift into points 6b, 6c and 6d. The overall effect is a more open orbital frame and positive brow and canthal axis (optimum 12-14 degrees) resulting in beautification of the eye.
References
1. Carruthers J, KR Coleman. Combination therapy with BOTOX™ and fillers: the new rejuvnation paradigm. Derm Therapy 2006;19(3):177-88.
2. Rohrich RJ, Pessa, JE. The fat compartments of the face: anatomy and clinical implications for cosmetic surgery. Plastic and Reconstructive Surgery 2007;119(7):2219-27; discussion 2228-31.
3. Furnas DW. The retaining ligaments of the cheek. Plastic and Reconstructive Surgery 1989;83(1):11-6.
4. Coleman SR, Grover R. The anatomy of the aging face: volume loss and changes in 3-dimensional topography. Aesthet Surg J. 2006;26(1S):S4-9.
5. Cohen AJ. Mid face facelift. Medscape; 2012.
6. Hartstein MD, Morris E, Allan E, David EE (Eds): Midfacial Rejuvenation. Springer; 2012.
7. Drake RL, Vogl AW, Mitchell AWM. Gray’s Anatomy for Students. Philadelphia: Churchill Livingstone (Elsevier); 2005.
8. Draelos ZD (Ed): Cosmetic Dermatology: Products and Procedures. First edition. Chichester, West Sussex: Wiley-Blackwell; 2010.
9. Mendelson B, Wong CH. Changes in the facial skeleton with aging: implications and clinical applications in facial rejuvenation. Aesthetic Plast Surg 2012;36(4):753-60.
10. Papageorgiou KI, Mancini R, Garneau HC, et al. A three-dimensional construct of the aging eyebrow: the illusion of volume loss. Aesthet Surg J 2012;32(1):46-57.
11. Lowe NJ Maxwell CA, Patnaik R. Adverse reactions to dermal fillers: review. Dermatol Surg 2005;
31(11 Pt2):1616-25.
12. Weinberg MJ, Solish N. Complications of hyaluronic acid fillers. Facial Plast Surg 2009;25(5):324-8.
13. Cohen JL. Understanding, avoiding, and managing dermal filler complications. Dermatol Surg 2008;34(Suppl 1):S92-9.
14. Bostwick J, Eaves FF, Nahai F (Eds): Endoscopic Plastic Surgery. Quality Medical; 1996.
15. Clemente CD. Anatomy - A regional Atlas of the Human Body, Fourth Edition. Lippincott Williams & Wilkins, 1997.
16. de Maio M, Rzany B. Injectable Fillers in Aesthetic Medicine, Second Edition. Springer; 2014.
17. Hunter JC, Savin J, Dahl, M: Clinical Dermatology, Third edition. Wiley; 2002
18. Levy PM. The ‘Nefertiti lift’: a new technique for specific re-contouring of the jawline. J Cosmet Laser Ther 2007;9(4):249-52.
Declaration of competing interests: None declared.
COMMENTS ARE WELCOME