It is essential to clearly understand the patient’s needs so I usually see patients three to four times prior to operating if major changes to appearance are planned. You must also be able to manage expectations and postoperative outcomes; for example, soft tissue responses to augmentation and reduction are often difficult to predict accurately. It is important to also bear in mind that there are higher than average numbers of body dysmorphic sufferers in this cohort than most other sectors of cosmetic surgery.
Over time you will develop a feel for facial harmony and be able to visualise deep tissue changes to the facial surface.
You should consider alternatives to implants, such as fillers and orthognathic surgery. Don’t be pushed into promising what you think are unrealistic expectations.
Diagnosis and treatment
- History: extent of previous cosmetic procedures to the face.
- Clinical examination: proportions and harmony. Beware of trying to correct minor discrepancies with surgery.
- Radiography of underlying facial skeleton:
i. Orthopantogram XR and a lateral cephalogram XR as a minimum to help plan placement and exclude underlying pathology, identify previous operative procedures not volunteered or forgotten!
ii. CT fine cut and streolithographic models of the face and jaw for planning and manufacture of custom made implants especially for asymmetries. - Thorough consent and complications. Up to 10% of implants can get infected and require removal.
- Photographic records.
- Identify and manage borderline dysmorphophobias, help the patient to recognise this or refer as appropriate with care and subtlety.
- Plan the least invasive procedures with no external scars if possible by using intraoral approaches for chin implants, paranasal and cheek / zygomatic implants and trans-conjuctival approaches for infra-orbital implants. Exceptions are small chin implants simultaneously placed to neck lifts and infra-orbital augmentation simultaneous to lower blepharoplasties.
Indications and cautions
I would consider the use of facial implants for: augmentation of the chin, cheek, paranasal, infra-orbital areas for camouflage of bony or soft tissue deficiency; alteration in appearance – minor to dramatic; asymmetry camouflage; age-related rejuvenation; or as an adjunct or alternative to orthognathic surgery in well selected cases.
The most common implant in use is the chin implant. Indications are a small advancement of no more than 3mm. Anything more than this usually means that projection of the chin and height often need correcting to camouflage the problem and implants are less resilient in addressing this. They should not be used to correct micrognathia. Chin implants or a sliding genioplasty should ideally be used only for the correction of microgenia. If camouflaging a deficient jaw (class II facial disproportion) with a chin procedure, a thorough analysis is required and profile diagrams shown of anticipated changes for the patient to understand the difference between a camouflage chin procedure for camouflaging a deficient jaw and a mandibular orthognathic procedure to properly correct the deficiency of the face. If one does not do this, proper informed consent of the alternatives has failed. The difference in chin contour and chin / lip shape and consequent facial harmony is sometimes profound.
Surgical Figures
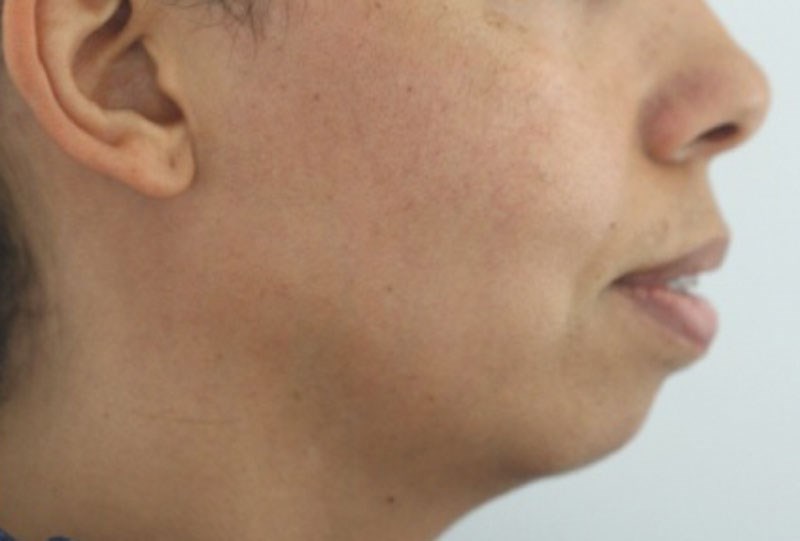
Figure 1: Pre-op. The patient shown here is both micrognathic and microgenic. Ideally, she would have needed a mandibular advancement and a sliding genioplasty, but she refused. A compromise osseous advancement genioplasty was done.
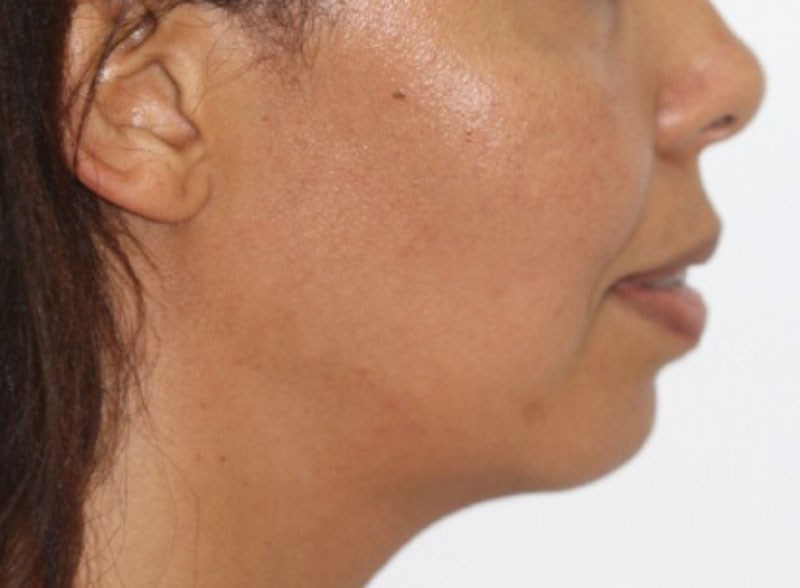
Figure 2: Post-op advancement osseous genioplasty of over a centimetre in projection and increase in lower facial height. A chin implant would have never achieved this advancement, contour accuracy or harmony, nor would it have achieved the increased neck chin sharpness the osseous genioplasty can achieve. This is still a compromised outcome, but with patient consent.
As a rule, a chin implant is a poor relative of the sliding genioplasty as they are prone to infection, distortion, displacement and long-term frequently cause resorption of the underlying bone, with consequent change in shape, disappointment and re-operation. Instead, an osseous genioplasty should be used for increasing shapely projection beyond 3mm and height or adjusting an asymmetry, while a sliding genioplasty can be used to substantially improve on the neck contour and neck chin angle. Chin implants are best used for minor advancements when doing a neck lift and can be inserted via a small submental incision.
Mandibular angle implants are used to widen, lengthen or define the mandibular angles for cosmetic purposes. Insertion is always intra-oral. Fixation of the implants and positioning are the most challenging aspects of these. I often use a transbuccal puncture incision to fix the implant with one or more titanium screws.
Likewise, paranasal, certain cheek and zygomatic implants are placed via an intra-oral approach in my practice. It would be very prudent in the diagnostic phase to identify whether there is genuine midface deficiency, and if so to identify if there is a skeletal class III facial disproportion. The diagnosis is easy: the maxilla and midface are retruded (dish-faced) and the lower part of the face (mandibular projection) relatively excessive. If this is the case, consider proper correction of the skeletal structures and therefore soft tissue outcome through orthognathic surgery.
I place high zygomatic and infraorbital margin implants through a trans conjuctival or blepharoplasty incision. Again, I tend to fix these with titanium mini-screws. These are often used in conjunction with orthognathic surgery in patients whose class III midface deficiency has been corrected by bringing the maxilla forward with a Le Fort I osteotomy, addressing the midface, paranasal and some lower cheek deficiency, but the retro-positioned infra-orbital rims and sometimes pseudo-exophthalmos is cosmetically unsatisfactory. Placement of the infraorbital implants / high zygomatic implants addresses this problem.
Declaration of competing interests: None declared.
COMMENTS ARE WELCOME





