Acne is common among individuals who experience a condition of hyperactive pilosebaceous units (precipitation and mobility of keratinocytes). A specific T-cell mediated inflammatory response is the initiating event in acne pathogenesis, followed by comedone formation.
The mechanism of inflammation is hypothesised to be a Type IV hypersensitivity reaction, where Propionibacterium acnes (P. acnes) is the probable antigenic compound, although seborrhea is still a necessary co-factor.
Laser therapies to treat acne widen the therapeutic options available. In addition to offering treatment to those unable to take (or who have failed) standard therapy, they also improve compliance, reduce the need for long-term antibiotics and retinoid therapy, and do not add to the problem of antibiotic resistance.
Laser light targets tissues to produce thermal, mechanical or chemical damage of target chromophores such as melanin within the epidermis and hemoglobin in the vasculature, whilst sparing the surrounding tissues. Nd:YAG laser either indirectly targets P. acnes, through photo-excitation of porphyrins – inducing a bactericidal effect by release of reactive free radicals, or causes phototoxic and / or photothermal damage to the sebaceous gland, resulting in reduced gland size and sebum production.
Nd:YAG laser therapy in acne must be examined and tailored according to: the laser pulse duration and spot size, the patient’s skin characteristics (skin colour, amount of sebum production, number of pilosebaceous units, thickness of the skin, age, etc.) and the treatment schedule.
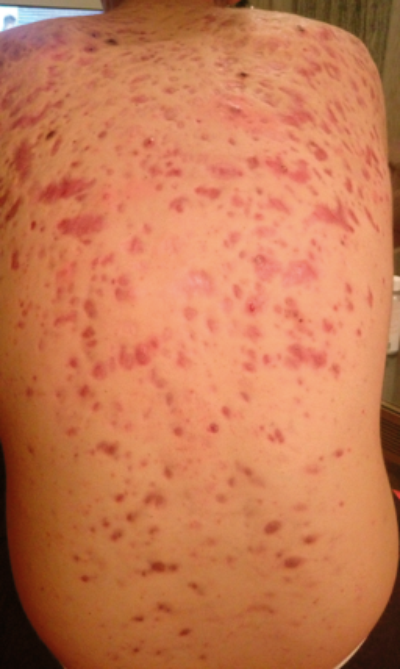
Figure 1: The patient’s back before treatment.
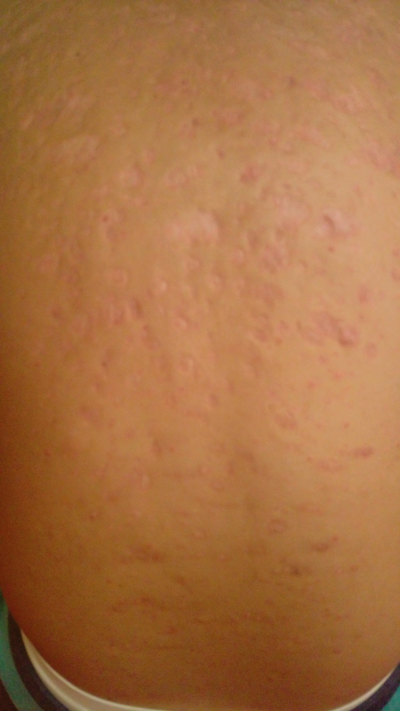
Figure 2: The patient’s back after treatment.
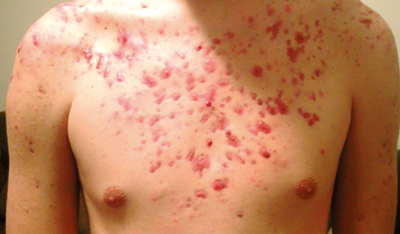
Figure 3: The patient’s chest before treatment.
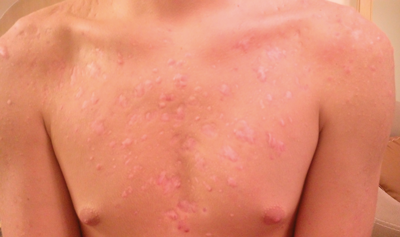
Figure 4: The patient’s chest after treatment.
The procedure
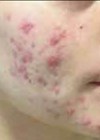
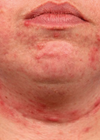
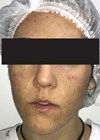
The patient was a 16-year-old male that presented with papules, comedones, painful nodules and cysts on the face, and a painful, ulcerating, and haemorrhagic clinical form of acne on the chest and back, as well as painful hip and knee joints. He was resistant to the usual acne antibiotics, but had tried topical non-prescription measures against acne, but no retinoids because of allergy to peanut oil. The patient didn’t have a meticulous skincare routine. His family refused the suggested combination of corticosteroids and isotretinoin.
We performed a series of therapies with a 1,064nm Nd:YAG laser (SP Dynamis Pro, Fotona, Slovenia). Every session included six full-face, chest and back passes with the R33 handpiece, 6mm spot size, 0.6ms, 15J/cm2, with a mild cold air cooling. We started with two sessions per week in the first month, followed by laser treatments once per week in the second and third month of treatment.
Visible improvement was gradually seen in the third week of treatment with a reduction of inflamed lesions, erythema, pain, and severity of new outbreaks. After two months, no recurrence of the superficial inflammation was present. After three months, the remission was complete with a residual scarring on the back area. In addition, he was prescribed a mild cleanser and Clindamycin 1% cream bid. The patient is still in remission after a year of follow-up.
Conclusion
The use of short-pulsed, low-fluence 1,064nm laser is a safe and effective treatment for even severe acne inflammation. The treatment was performed with minimal discomfort and no downtime. At the same time this treatment also reduced scar depth and produced a softening of scar contours. Future studies should aim to further quantify results while optimising treatment intervals and parameters.
Declaration of competing interests: None declared.
COMMENTS ARE WELCOME