The authors introduce us to the ‘pinpoint technique’ a variation in skin excision to eliminate the notorious T-junction in mammary revision augmentation.
The Wise-pattern skin excision is widely used to correct ptotic breasts, or in breast implant revision surgery when abundant skin excess has to be corrected [1]. The goal of the surgeon is to obtain an exact fitting skin envelope around the underlying tissue and implant.
A Wise-pattern skin resection technique leaves the patient with an inverted-T scar [2‑4]. The three-way-intersection or T-junction, where the medial and lateral breast tissue flaps meet, is known to be a troublesome point in wound healing occasionally leading to wound dehiscence [1,5,6]. This complication is certainly unwanted in revision augmentation surgery because of risk of infection of the underlying implant.
To reduce skin-healing problems at the T-junction, modified techniques have been described, although still reporting complication rates varying from 2.2-30% [5,7,8]. Only two studies, with small patient groups, reported no wound complications [6,9].
We would like to introduce the ‘pinpoint technique’, which presents a variation in skin excision to eliminate the notorious T-junction in mammary revision augmentation.
Patient case
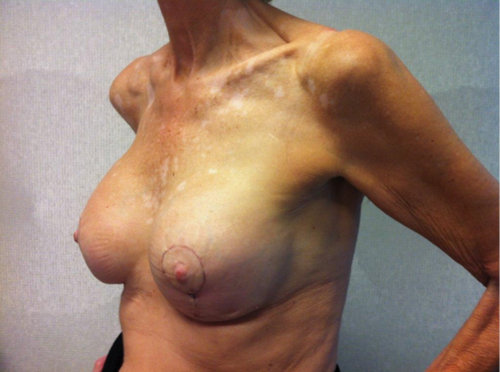
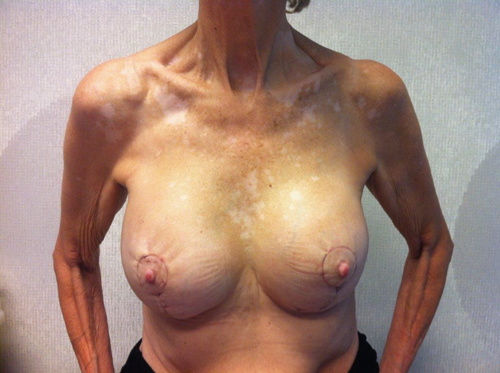
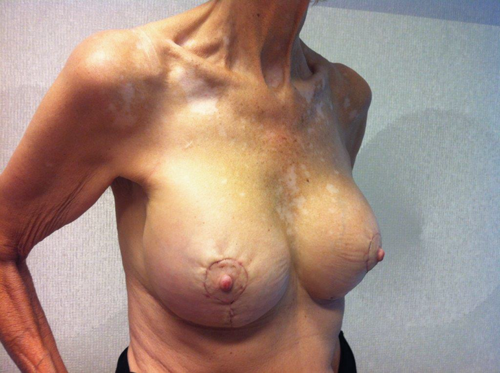
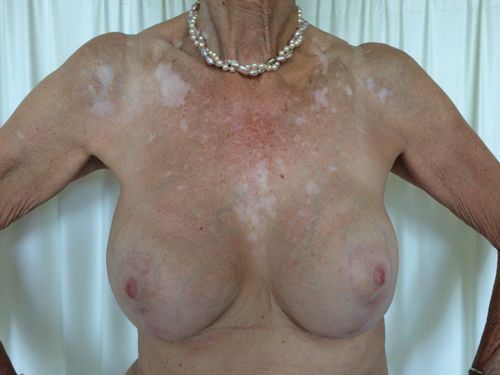
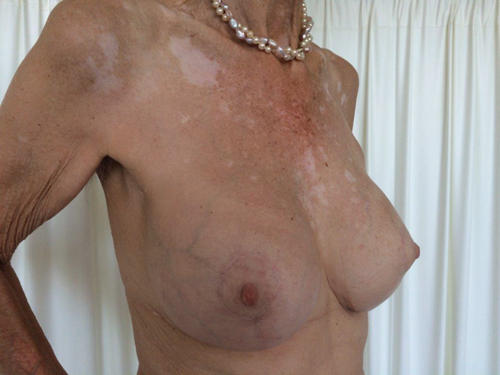
A 60-year-old patient presented with asymmetry of the breasts, 17 years after revision breast augmentation. On inspection, the right implant was placed in a prepectoral position; the left implant was positioned subpectorally, through an inframammary incision. Both breasts showed abundant skin and caudal displacement of breast tissue over the breast implant, causing a double bubble phenomenon and an asymmetrical caudal nipple position. In examination of the breast tissue, no abnormalities were palpable. The implant showed a capsular formation, classified as Baker 3 on the left side and Baker 4 on the right side (Figure 1).
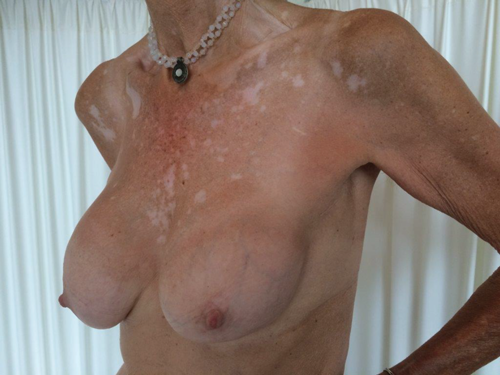
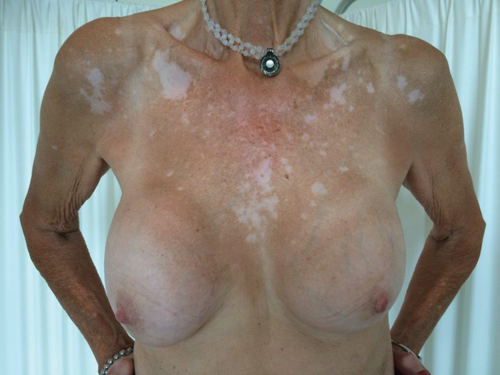
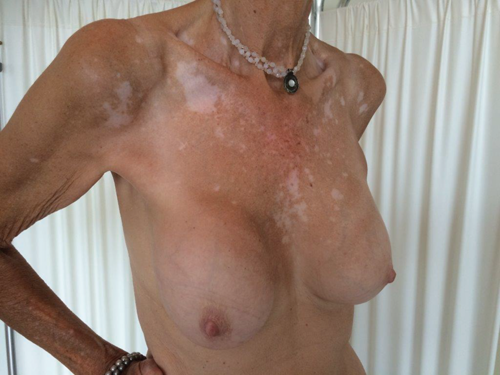
Figure 1. Preoperative left lateral (top) frontal (middle) and right lateral (bottom) view.
A revision augmentation was advised in combination with skin resection. Because of the mild skin excess we preferred to use the pinpoint technique. The term pinpoint was chosen because of the resemblance of the figure in road map utilities (Figure 2a).
2a.
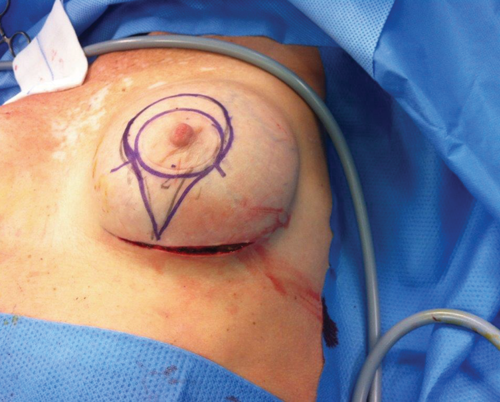
2b.
Figure 2. Pinpoint design (2a). Intraoperatively pinpoint design for skin reduction (2b).
The pinpoint technique
Preoperatively the amount of excess periareolar and inframammary skin was preliminary marked according to the pinpoint design (Figure 2b).
The patient was placed in the supine position under general anaesthesia, with preoperative administration of intravenous antibiotics.
The breasts were prepped and draped and the left inframammary scar was excised, followed by a total capsulectomy and removal of the implant (275 gram, textured, round). It was not necessary to perform a dual plane conversion because of the already existing subpectoral position of the removed implant. After placement of wound drains new implants (360 gram, textured, round) were positioned. According to the preoperative drawings, the vertical amount of excess skin was now resected in the inframammary fold, tailor tacking the skin caudal to the nipple. Subsequently, the pinpoint marked area was de-epithelialised, tailor tacking the horizontal and periareolar skin excess (Figure 3).
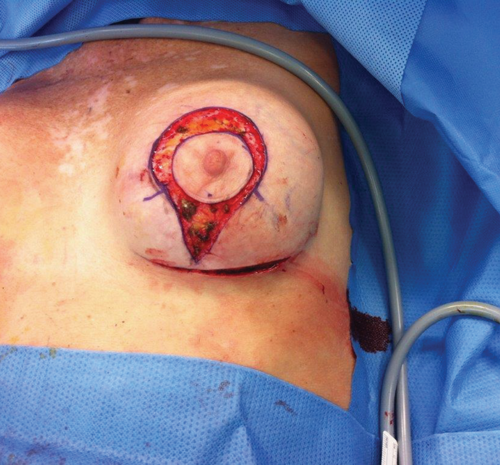
Figure 3. Intraoperatively after pinpoint markings were de-epithelialised
and the appropriate amount of periareolar skin was excised.
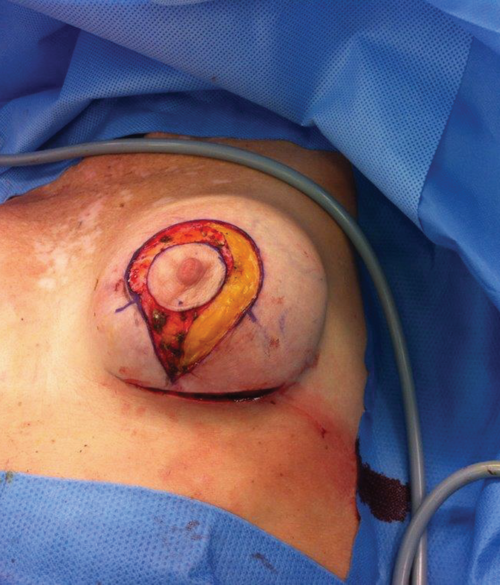
Figure 4. After incision of the lateral side in order to facilitate skin closure.
On the lateral side the subcutaneous tissue was incised in order to facilitate skin closure (Figure 4). In this manner a perfect draping around the existing breast volume was made possible. The vertical and inframammary incisions were closed in layers with vicryl 3.0 and 4.0 subcutaneously and monocryl 4.0 running suture was used for intracutaneous closure. Transcutaneous prolene 6.0 sutures were used for periaureolar closure.
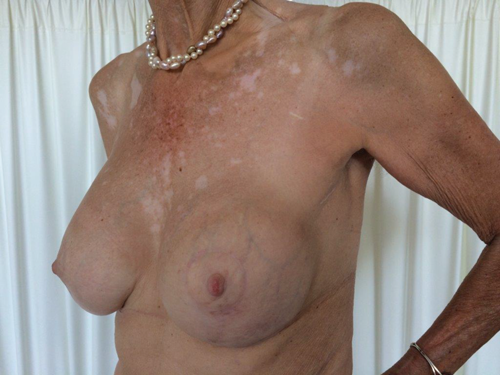
On the right side, an identical procedure was performed. A dual plane conversion of the position of the implant was realised in order to obtain symmetry with the opposite side. Postoperatively, good symmetry was obtained. Figure 5 and 6 show postoperative results from 10 days and four months postoperatively.
Figure 5. Ten days postoperatively left lateral (top) frontal (middle) and right lateral (bottom) view.
Figure 6. Four months postoperatively left lateral (top)
frontal (middle) and right lateral (bottom) view.
Discussion
In this case report we present a new variation in skin resection in revision augmentation plasty; the pinpoint technique. The aim is to prevent skin healing problems and wound dehiscence at the conventional T-junction in patients requiring mild excess skin resection.
“This minimally invasive technique preserves circulation in the inframammary fold and diminishes the chance of necrosis and / or infection.”
In the literature, total skin healing associated complication rates at the T-junction are reported in up to 30% of cases [5-9]. These complications are related to surgical techniques such as excessive suture tension or diminished blood flow by using the inverted T-incision or are related to internal patient related factors such as pressure from seroma or haematoma, ischaemia or infection. Also external patient related factors are described [5,7,10,11]. When the area of wound dehiscence is small, it is self-limiting. In case of deep tissue infection or fat necrosis, debridement is manditory [12]. When periprosthetic infection occurs, implant explantation might be necessary [13,14].
The pinpoint technique eliminates the T-junction in the Wise-pattern skin excision by leaving a skin bridge below the vertical incision line. This minimally invasive technique preserves circulation in the inframammary fold and diminishes the chance of necrosis and / or infection. In our opinion it reduces postoperative skin healing problems and provides a high patient satisfactory rate.
Other promising techniques to reduce skin-healing problems at the T-junction area in breast surgery do not eliminate the three-way-intersection and patients are still at risk of undergoing skin-healing problems [5-9].
Thus far, we have performed the pinpoint technique in 25 patients without any wound healing complications. In future efforts we will present larger case number on this technique.
Conclusion
The pinpoint technique is a variation of the skin excision technique applicable in mammary revision augmentation and ptosis corrections. When resection of mild excess of skin is necessary, this technique leaves a well-circulated skin bridge below the lower vertical incision line. This eliminates skin healing problems and subsequent infections or necrosis. In our opinion, this technique also delivers a comely aesthetic result. The pinpoint technique is safe, effective and applicable to mild to moderate skin revision in ptosis surgery of the breasts.
References
1. Eisenberg T. Simultaneous augmentation mastopexy: a technique for maximum en bloc skin resection using the inverted-T pattern regardless of implant size, asymmetry, or ptosis. Aesthetic Plast Surg 2012;36(2):349-54.
2. Hidalgo DA. Improving safety and aesthetic results in inverted T scar breast reduction. Plast Reconstr Surg 1999;103(3):874-86.
3. Wise RJ, Gannon JP, Hill JR. Further experience with reduction mammaplasty. Plast Reconstr Surg 1963;32:12‑20.
4. Wise RJ. A preliminary report on a method of planning the mammaplasty. Plast Reconstr Surg (1946) 1956;17(5):367-75.
5. Nahai FR, Nahai F. MOC-PSSM CME Article: Breast reduction. Plast Reconstr Surg 2008;121(MOC-PS CME Coll):1-13.
6. Liu TS, Crisera CA, Festekjian JH, Da Lio AL. Staged Wise-pattern skin excision for reconstruction of the large and ptotic breast. Plast Reconstr Surg 2010;126(6):1831-9.
7. DeFazio MV, Fan KL, Avashia YJ, et al. Inferior pedicle breast reduction: a retrospective review of technical modifications influencing patient safety, operative efficiency, and postoperative outcomes. Am J Surg 2012;204(5):e7-e14.
8. Hansen JE. Avoiding the unfavorable outcome with Wise pattern breast reduction. Clin Plast Surg 2016;43(2):349-58.
9. Ceydeli A, Freund R. Tear-drop augmentation mastopexy?: a technique to augment superior pole hollow. Aesthetic Plast Surg 2003;27(6):425-33.
10. Salgarello M, Visconti G, Barone-Adesi L, et al. Inverted-T skin-reducing mastectomy with immediate implant reconstruction using the submuscular-subfascial pocket. Plast Reconstr Surg 2012;130(1):31-41.
11. Knobloch K, Gohritz A, Reuss E, Vogt PM. Nikotinkonsum und plastische Chirurgie. Der Chir 2008;79(10):956-62.
12. Saleem L, John J. Unfavourable results following reduction mammoplasty. Indian J Plast Surg 2013;46(2):401.
13. Clough KB, O’Donoghue JM, Fitoussi AD, et al. Prospective evaluation of late cosmetic results following breast reconstruction: Implant reconstruction. Plast Reconstr Surg 2001;107(7):1702-9.
14. Elliott LF. Circumareolar mastopexy with augmentation. Clin Plast Surg 2002;29(3):337-47.
Declaration of competing interests: None declared.
Patient consent: The patient presented provided written consent for the use of her images.
COMMENTS ARE WELCOME